Support WBUR
Commentary
What It's Like To Help Families Say Goodbye
“Hello! Hola! Cómo estás?” I ask, peering into the eyes of my patient’s concerned adult children.
“Muy bien, Bridget.” “Gracias.” “How is Mamacita today?”
I have never met this family, but in the dozen or so video calls that we have had during the past month, I have gotten to know them.
I recognize their dining rooms, I know the names of their spouses and children who sometimes make appearances — and they know the limits of my Spanish. Their faces shuffle across the screen of my iPad as they take turns talking to their mother, the patient whose hand I hold.
COVID-19 brutalizes bodies, but it also disempowers families who are unable to see their loved ones, sit at their bedsides and hold their hands.
Most of the families that I have supported over the past three months have been people of color. Their first language is often Spanish or Creole. At the teaching hospital where I work, physicians rotate through the ICU, so families often wonder if their loved ones are receiving as good care this week as they did the last. I assure them they are.
[F]amilies often wonder if their loved ones are receiving as good care this week as they did the last. I assure them they are.
They fear worst-case scenarios that the hospital will run out of ventilators, and they carry feelings of helplessness, confusion, desperation and guilt. Implied in our conversations, they say to me, I gave her this virus. I should have done more to protect her. It is my fault that she might never come home. I would do anything to be with her.
While Massachusetts’ stay-at-home advisory and our hospital’s visitor policy prevent these families from being with their loved ones due to safety reasons, I, as a hospital chaplain, have the privilege of visiting patients in their rooms.
I hear the steady rhythm of the ventilators. I witness the care with which the respiratory therapists turn patients’ bodies from supine to prone and back again. I see the attentiveness of nurses who go in and out of rooms, donning and doffing their gowns, masks and shields throughout their 12-hour shifts. I overhear physicians’ thorough discussions as they make their rounds. In the midst of this hectic setting, I can be a consistent presence for these families and alleviate some of the stress of care team members, who wish they could do more to support these families.

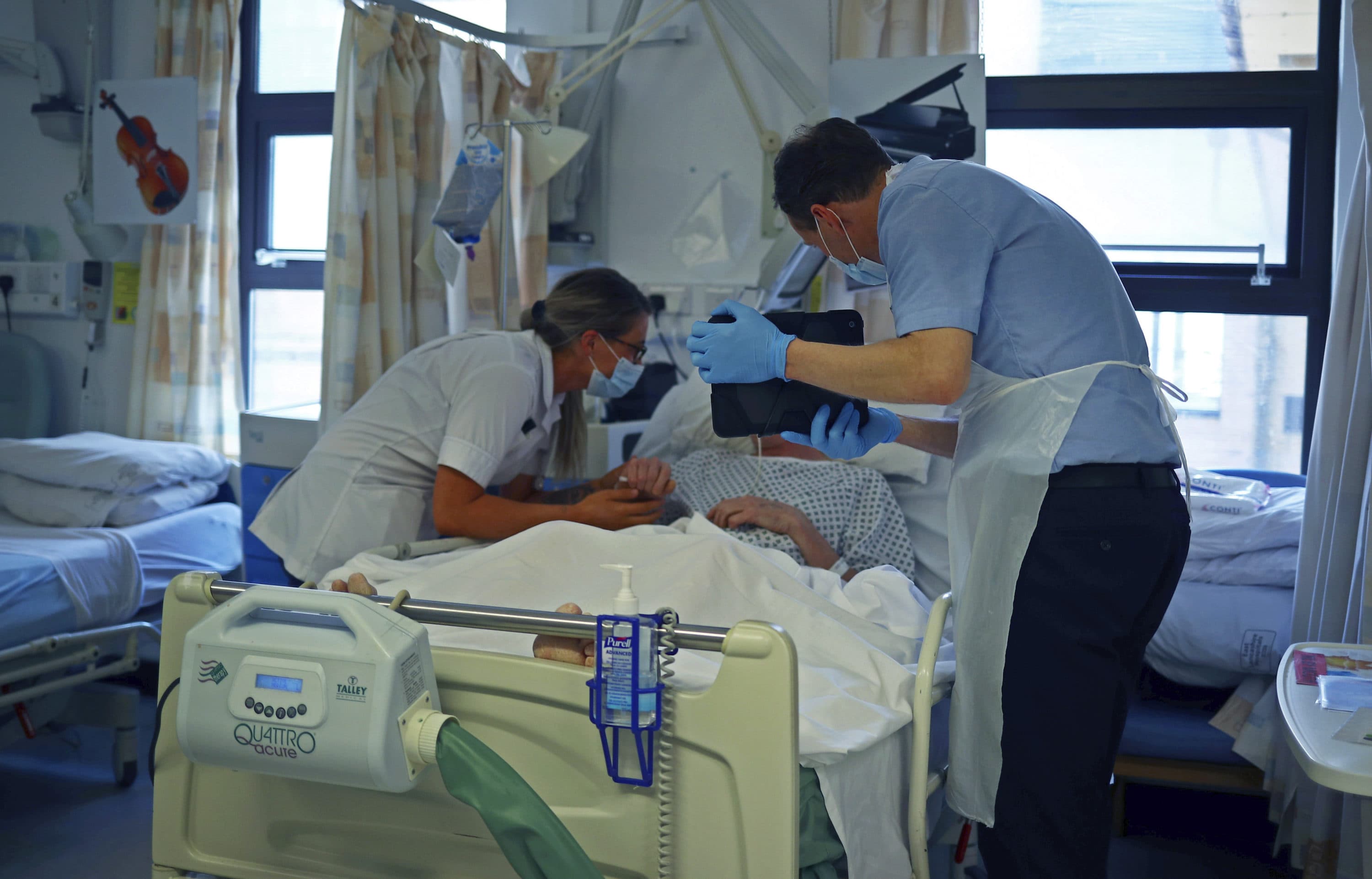
At the beginning of a video call with family members, I make sure to start with the camera on my face. Despite my shield and mask, I want the family to be able to see my eyes, to see that I am committed to supporting them, and that I am someone who recognizes and can be with them in their pain. I then flip the iPad's camera around to show them the view of Boston from their loved one’s window, orienting them to the space inside the room and beyond. The room is spacious. The nurse is there, right outside the door. The ventilator is pumping.
They can then see their mother, their father, their spouse, their child, and recognize that they are receiving good care. “Here’s her hand,” I say, tilting the iPad so that they can see my gloved fingers wrapped around the hand that they recognize so well. “She can hear you.”
I hold the iPad up to the patient’s face with my other hand, inviting the family to speak, to pray, to sing. The visit unfolds, each one different from the next. After the call, family members verbalize to me how grateful they are.
COVID-19 has reminded us all that there are limits to what we can control.
COVID-19 has reminded us all that there are limits to what we can control. These Zoom calls seem inadequate during times of such distress, and yet they do allow family members scattered across the world to express their love, give thanks and say goodbye together. “Seeing her resting there has given me peace,” one son said to me in the hour before his mother died.
Intubated and sedated, “Mamacita” spent a full month — including Easter and her birthday — in a COVID-19 ICU. Although she could not open her eyes or speak, I visited her every few days so that her children could talk to her and pray for her. None of us knew if she would make it, but as our visits continued, I grew more confident that these calls were healing for these siblings because they could articulate their fears, offer words of reassurance to their mother and pray with one another.
Recently, “Mamacita” was successfully extubated. Her next stop will be a rehab center. In our final Zoom call with her family, she told them that I was her amiga. “Adiós,” I said to her as I left the room.
“God Bless you,” she said, before I closed the door behind me.
