Support WBUR
Commentary
What The U.S. Can Do Right Now To Help Vaccinate The World

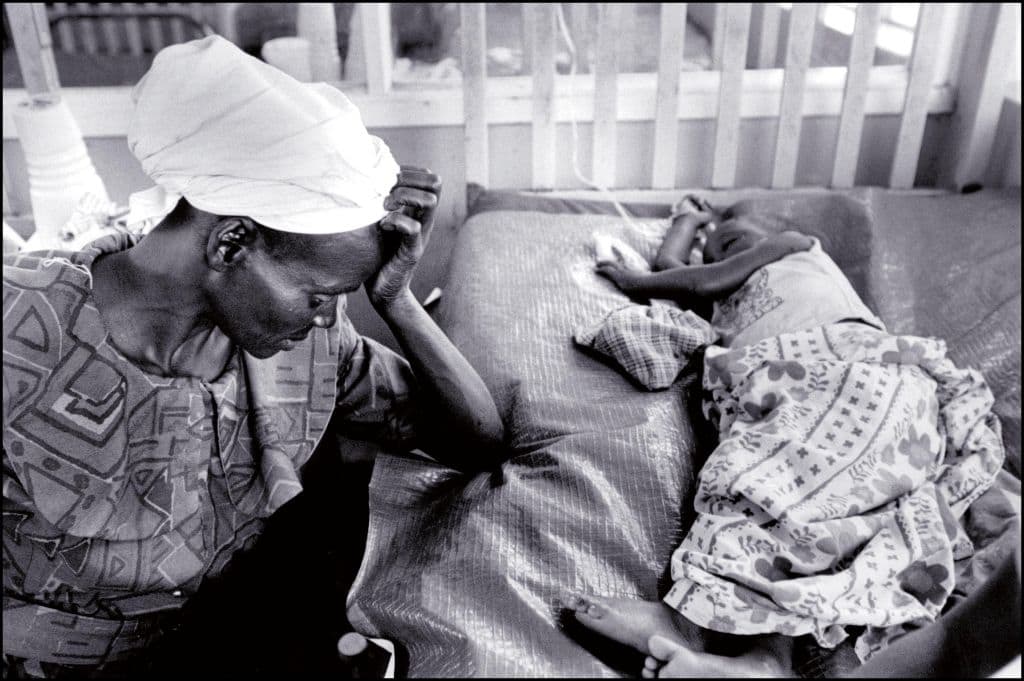
As a young medical student and doctor working in Africa in the 1990s, AIDS seemed like the apocalypse. Weekends were for funerals. Coffin shops ringed the major urban hospitals. Prevention — telling women to demand condom use, or abstaining from sex entirely were the only strategies on offer — no treatment, no vaccine.
The year I returned to the U.S., in 1995, the AIDS cocktail of three drugs turned the fatal disease into a chronic but manageable one. My American patients rose from their death beds in what the medical literature called “the Lazarus” effect. One patient I cared for in the ICU, who had discussed withdrawing life support with his partner, enrolled in a clinical trial for the cocktail. Several years after my infectious disease fellowship, I was invited to his law school graduation.
But the timeline between the discovery of life saving medicines and their distribution in the epicenter of the pandemic — Africa — was fully eight years. Between 1995 and 2003, 8,000 people died every day for lack of treatment, about 23 million people.
Some were friends I had made in Uganda and Kenya. All were human — brothers and sisters, sons and daughters, mothers and fathers. The yawning gap put me and so many of us — including prominent members of the Biden administration’s COVID team, from Dr. Anthony Fauci to Dr. Rochelle Walensky — into one of the most massive global human rights struggles of the 20th century.
The fight for AIDS treatment access was led by people living with AIDS who demanded treatment. Led by the belief that health and science are human rights, they demanded concrete steps to share the science of the HIV drug cocktail: its three drugs, all patented, developed by private pharmaceutical companies with huge public investments, and sold at a huge profit margin, only in wealthy countries.
As a doctor who had worked in Africa, I had already been stunned, and frankly broken by the lack of modern medical care. In my journey to understand how this could be, I started with the life-saving and life-affirming human rights enshrined in the 1948 Universal Declaration of Human Rights. Article 25 guarantees the right to health and Article 27 goes even a step further saying:
Everyone has the right … to share in scientific advancement and its benefits.
It is upon veracity of this last, short and often forgotten phrase, that the lives of billions of people rested then, and now.
The COVID pandemic can be ended with massive scale up of vaccine production. But it will require dismantling one of our basic, American tenets: patent protection of intellectual property. The reason the United States has never endorsed the concept that a “share in scientific advancement and its benefits” is a basic human right is that drug development and distribution is based on a free market model. Profit — not human rights or need — is considered the only feasible driver for the distribution of scientific advancements. Profit, we are told, drives innovation.
The COVID pandemic can be ended with massive scale up of vaccine production. But it will require dismantling one of our basic, American tenets: patent protection of intellectual property.
Patents prevent copy cats or generic manufacture of the innovation, allowing for a legal monopoly — often for 20 to 30 years — so a company might recuperate the cost of development, and assure profit for its CEO and shareholders.
But markets do not work for the poor, the oppressed, the marginalized. When life-saving drugs, vaccines and technologies are patented interventions, these market failures are fatal.
The COVID-19 pandemic has demonstrated the catastrophic impact of market failures of medical technologies. The rapid development of the mRNA COVID vaccines by Pfizer-BioNTech and Moderna were no doubt a feat of great scientific advancement; and based on the market model, should garner what profits the market can bear. The stock of these companies skyrocketed, as did their profits, resulting from orders by wealthy countries, for five- to ten-fold more doses than what they actually needed.
But as the percentage of Americans vaccinated approaches 50% and hope emerges here at home, the situation around the world is dire.

In India, the current epicenter of the pandemic, less than 1% of the population is vaccinated. Similar vaccination rates threaten the entire African continent, as well as much of Latin America and Asia. This reality assures not only a rising and apocalyptic death toll, but the generation of variants, the stagnation of the global economy, and worsening suffering of those already living in poverty.
The gap widens between those who benefit from the science of COVID-19 vaccines and treatment, and those who do not.
In this setting of great human suffering, the U.S. must waive patents. There are provisions in patent law for this purpose; specifically, the “trade related aspects of intellectual property” or TRIPS agreement, can be waived during a national emergency. President Biden could use the World Trade Organization meeting this week, on May 5, to take this critical step.
Twenty years ago, under pressure from activists and the gravity of the AIDS pandemic, such a waiver — or lack of enforcement of the patent — was granted. That year, in Doha, Qatar, George W. Bush administration’s trade representative declared: “We agree that the TRIPS Agreement does not and should not prevent members from taking measures to protect public health.”
In this setting of great human suffering, the U.S. must waive patents.
That statement opened the door to generic manufacture of AIDS drugs, which, 20 years on have successfully reached 27 million people.
Today, the need is even more urgent. A TRIPS waiver is just the first step in a cascade of steps that are required to radically change global vaccination rates.
While Moderna has promised not to enforce the patent on their vaccine for the duration of the pandemic, the reality is far more complicated than the waiver alone. The process of making the mRNA vaccine is novel, it requires other patented ingredients (most notably the lipid nanoparticles).
In addition, the Biden administration must work with Moderna and Pfizer, to insist that the companies share their know-how — the manufacturing process — with companies in the global South. This can be done through payment for the licensing and technology transfer.
The basis for the leverage that the U.S. government has to take these steps is the massive public investment that has gone to these companies, from the recent “Operation Warp Speed” to the countless National Institutes of Health grants that have gone to investigators of these vaccines. There are, indeed, laws that protect the government’s right to negotiate licensing on technologies developed with public funding.
Finally, real leadership demands funding. Not just small-scale funding, but funding to the scale of a 100-year global pandemic. Public Citizen and other groups have estimated that $25 billion are needed to scale production of the vaccine. This is a small price to pay for the multilayered benefit in human rights, health, diplomacy and security.
The U.S. endorsement of a TRIPS waiver, its work with companies on sharing know-how, and funding the scale of manufacturing to the size of the crisis, are the smart and strategic steps that the Biden administration must take to address a moral imperative of our time.
