Support WBUR
Commentary
Forcing my COVID patients to die alone is inhumane — and unnecessary
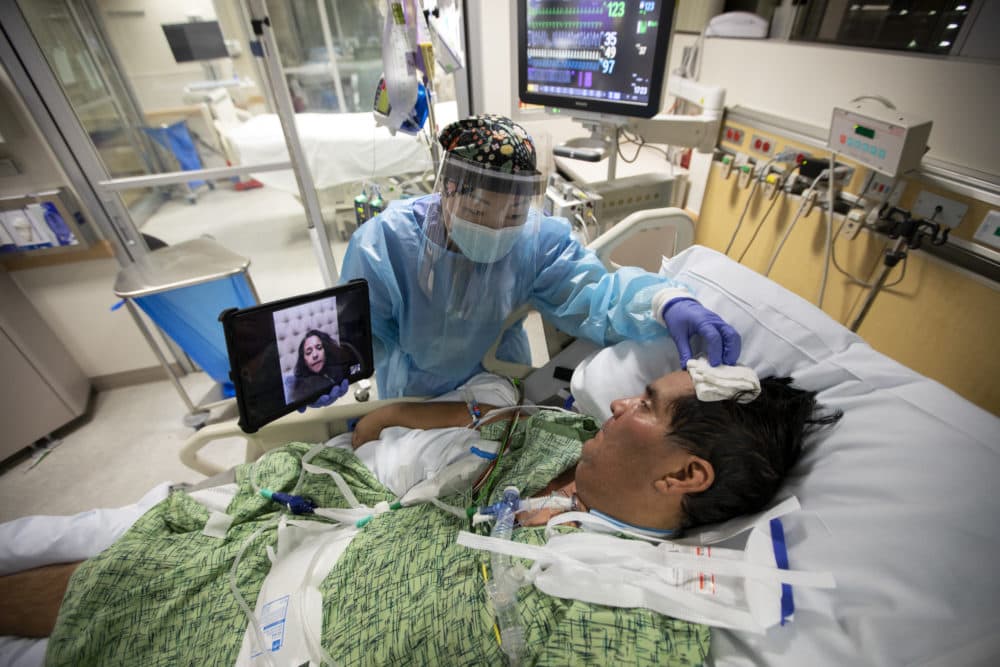
Mark, one of my patients in the ICU, continued to worsen, as his lungs grew stiffer and his other organs began to fail. I told his family the bad news over the phone.
“What does that mean?” his young son asked with a quivering voice, trying to sound brave.
“He’s going to die. I’m so sorry,” I replied.
There was silence as he processed. Mark (I changed his name to protect his anonymity) took his last breath later that night. His children kept him company by video on a tablet next to his bed and asked us to hold his cold hand for them.
We're approaching 1 million U.S. deaths from COVID-19, but the numbers can't capture how these deaths occur: alone. Patients take their last breaths amid the alarms of the Intensive Care Unit (ICU), without their families.
Despite a dizzying pace of policy change to keep society going, policies condemning COVID-19 patients to die alone have not changed.
In pre-pandemic times, families often kept vigil at their loved ones' bedsides. When COVID-19 hit in March 2020, the majority of U.S. hospitals shut down to visitors in conjunction with other societal shut-downs. As society attempted to move on, hospitals largely remained shuttered to visitors, with few exceptions. In many hospitals, non-COVID patients can have one visitor per day for limited hours. COVID patients, including those on ventilators, are not allowed any visitors.
Hands reach out to each other, millimeters apart on the screen but cruelly, never able to touch.
This near-universal policy of forced isolation in the ICU is not conclusively supported by data and is clearly traumatic to patients, their families, and clinicians like me caring for the dying in the ICU.
Patients critically ill with COVID-19 usually spend several weeks in the ICU before they are discharged or die, weeks of agony separated from families. Before we place patients on a ventilator, we, the ICU staff, often make video calls home. Hands reach out to each other, millimeters apart on the screen but cruelly, never able to touch. Real kisses are replaced with air kisses. I recall innumerable patients gasping for air, tears streaming down their faces, and fear etched in their eyes while calling their families in what were their last conversations.
For patients tethered in bed by tubes and lines, the trauma of critical illness and delirium contributes to long-term post-traumatic stress disorder and Post-Intensive Care Syndrome (PICS). PICS is a constellation of cognitive and physical impairments, along with mental health disorders, that plague patients long after they leave the ICU. We clearly know that depriving patients of the healing comfort of their loved ones’ presence only worsens this trauma and these health complications of critical illness.
We try to substitute comfort from family by holding patients’ hands with our gloved hands. But the sheer burden of providing comfort through sweaty PPE to more than 950,000 dying Americans is soul-crushing to our burned-out health care workforce.
But the sheer burden of providing comfort ... to more than 950,000 dying Americans is soul-crushing to our burned-out health care workforce.
In an effort to bring humanity to an otherwise sterile environment, nurses often decorate the ICU rooms with pictures and stories. They set up video chats for families to talk to their loved ones. We also make daily calls to families whose voices are filled with fear as they try to picture their relatives in the ICU.
Inevitably, we make the final phone calls to share that their loved ones are dying and it is time to say goodbye, often over a blurry video from a tablet kept in a plastic bag. We know well what an abysmal option this is. It is devastating to me that two years later, we are still making these fuzzy video calls for families to say goodbye.
During an end-of-life visit in which two visitors come for one paltry hour, an arbitrary time limit, we are unfairly tasked by hospital leadership with pulling loved ones away after this mere hour. Families must now choose who gets to say goodbye. These loved ones say goodbye knowing they are leaving their relative to die alone.
Families lament the inhumanity and cruelty of the visitor restrictions, and they are not wrong.
We can arbitrarily ask hospital leadership for exceptions to visitor restrictions. This is a deeply problematic approach that only perpetuates the bias and discrimination in American healthcare laid bare by the pandemic. Families who don't speak English, aren't technology savvy, who don't have powerful connections, or who feel less empowered are often non-white and immigrant families. They are less likely to get exceptions to visitor restrictions.
And yet, the health risk of visitors to the ICU is minimal. ICU patients are in single rooms with high-efficiency particulate air (HEPA) filters that remove 99.97% of particulates as small as 0.3 microns in size, smaller than the size of aerosol particulates carrying the COVID-19 virus. The ventilator is a closed-circuit system, which means that anyone in the room is not exposed. The risk of transmission is extremely low.
The other risk to consider in allowing visitors is the risk to hospital staff. Given that ICU staff are fully vaccinated, masked, and wear N95 masks or respirators in COVID-19 rooms with HEPA filters, I believe that the risk to them from visitors is also minimal. In fact, the risk of transmission inside an ICU room pales in comparison to the risk of transmission at grocery stores, sporting venues, airports, bars and restaurants.
As society forges ahead, the critically ill and dying are left behind without data supporting reactionary rules condemning them to suffer and die alone. A few changes to visitor policies would alleviate much of the trauma caused by isolation in the ICU. Visitation in the ICUs can be regulated (e.g. limited number of people per day) but should not be shut down entirely even during times of increased community spread given the increased safety measures in the ICU.
Patients on mechanical ventilators, including COVID-19 patients, should be allowed visitors. Families should be allowed at the bedside of the dying. As physicians, we take an oath to do no harm. Yet overly restrictive visitor policies force us to harm patients and families in ways with which we will still be contending for years to come after the pandemic is over.
