Support WBUR
Commentary
A year after Dobbs, the abortion care I provide is more important than ever
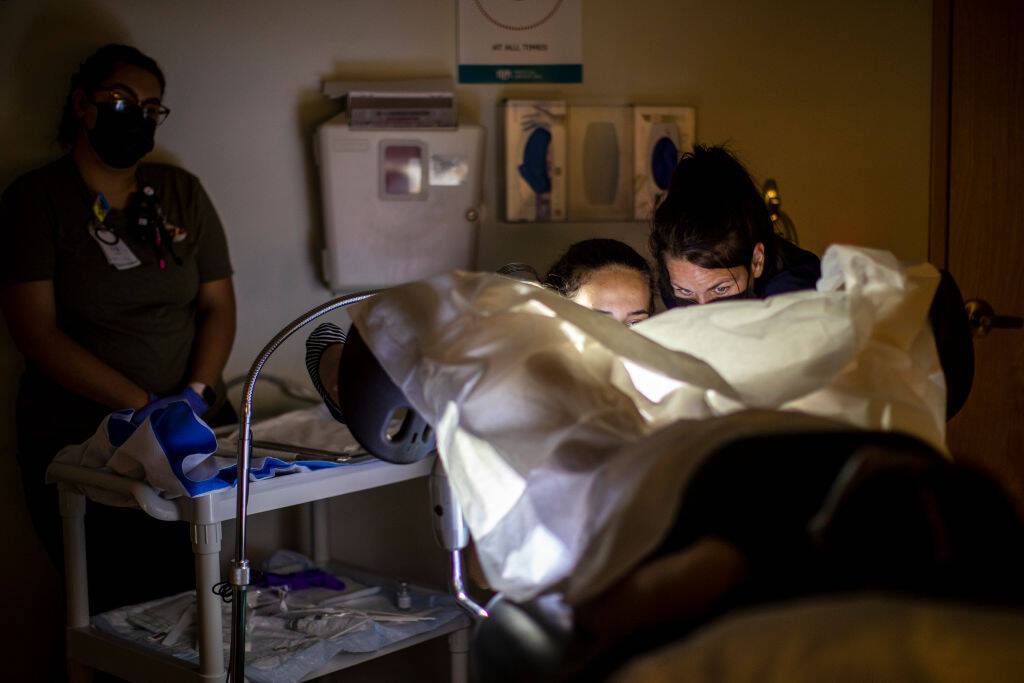
In the OB/GYN clinic my patients cautiously discuss new symptoms “down there,” talk about pain during sex for the first time or ask how to end an unexpected pregnancy. It is not unusual for patients to look at the floor, wring their hands or hang their heads in shame as they speak. I’m a third-year resident physician and one of the things that drew me to obstetrics and gynecology was the opportunity to help patients release that shame: I do my best to make it acceptable to simply exist in a body with reproductive organs. There is no other organ system so politically and socially fraught as the reproductive system — hearts and lungs remain uncontroversial.
Whether I'm recommending a new medication, obtaining informed consent for a surgery, or providing abortion care, I often return to the same refrain: “It is your body. It is your choice.” I see a shift in my patients after I say this, a subtle posture change and new strength in their voice when they respond. I invite them to reclaim their body as their own, empowered to choose what they need.
I like the phrase abortion care because it speaks to the intention underlying the medication or procedure.
June 24 marks one year since Dobbs, the Supreme Court decision that reversed some 50 years of precedent granting a constitutional right to abortion under Roe. I provide abortion care because I believe in reproductive justice, defined by SisterSong as the human right to maintain personal bodily autonomy, have children, not have children, and parent the children we have in safe and sustainable communities.
And I like the phrase abortion care because it speaks to the intention underlying the medication or procedure. I care deeply about my patients who need abortions. I care about their families and their futures, their physical safety; I care about keeping them alive.
Over the last year of my medical training, I spent about three months on rotation in family planning, a subspecialty focused on complex contraception and abortion care. Most of my patients were from Massachusetts; but some traveled from states where abortion is illegal. Many explained how angry they were about Dobbs decision and we commiserated, talking about our fears about what would happen to the patients who couldn’t travel. Unfortunately, our worries are well-founded — there is a growing body of evidence, including this study by a policy group at the University of Texas, showing the harm the Dobbs decision has caused. Additional research by the Commonwealth Fund suggests that states with restrictive abortion policies have maternal and infant death rates that are 62% and 15% higher.
I never ask patients why they want an abortion, but often people want to share. I heard about pregnancies as the result of rape, students with plans to complete their degrees, parents who could not get enough food on the table for the children they already had, fetuses with fatal anomalies, missing kidneys or partial brains.
And then there are the patients for whom abortion is not really a choice — they may not survive without one. I took care of a mother who was bleeding heavily at 19 weeks from a placental abruption, a dangerous condition where the placenta separates from the wall of the uterus. Her pregnancy was planned and desired, but she and her husband made the difficult decision to end the pregnancy for her safety. As my mentor, high-risk obstetrician Dr. Erika Werner has written, abortion helps us save lives.
I’ve been thinking about where to plant my roots when I complete my training, and there’s a map I can’t stop thinking about. A colleague said it haunts her so much she sees it in her dreams. “Dark times,” we say, heads shaking, “dark times.”
It’s the Guttmacher Institute’s map, U.S. Abortion Policies and Access After Roe, which categorizes state abortion policies from protective (blue and teal) to restrictive (orange and red). I can do my job in blue and teal states. Yellow states are a toss-up, while orange and red cover swaths of the country that are off limits. The colors have changed over the course of this year as more restrictive laws were passed. Each time I check back, it looks like the country is going up in flames.
I only applied to residencies where I knew I would get comprehensive abortion training. I will not practice in a place where I’m not allowed to provide the full spectrum of reproductive healthcare; and my fellow residents are making similar calculations. But as the years go on, the number of providers who are trained to provide abortion care will shrink and the quality of the OB/GYN workforce in restrictive states will suffer.
In Massachusetts, we are more insulated than most from the danger of a post-Roe country. While abortion was effectively outlawed in many states across the South and Midwest, we passed laws to protect abortion access. We eliminated cost-sharing for abortion care, to make sure no one gets surprise bills due to high deductible insurance plans. Public colleges and universities are required to provide medication abortion on campus. Abortion providers like me are protected under Massachusetts law from restrictive states like Texas, that are attempting criminal prosecution.
I do research on integrating abortion care into primary care. It’s an approach that destigmatizes and normalizes abortion care and is essential to improving access while avoiding overburdening specialty clinics. Interviewing primary care physicians for a study in 2020, I asked: “What would it mean for your patients if Roe v. Wade was overturned?” It was hypothetical then, a far-off fear. A few people even laughed when I asked, saying it would never happen. These were New Englanders, and most of them expressed that their states would be protected, but that they feared what it would mean for patients elsewhere.
They said lives would be irrevocably changed; lives would be lost. No one is laughing now. We can’t take our rights for granted.
Charlotte Lee MD, M.Sc. is a graduate of the Warren Alpert Medical School of Brown University. She is currently an OB/GYN resident physician at Tufts Medical Center.
