Support WBUR
Coronavirus Coverage
Another COVID-19 Medical Mystery: Patients, Post-Ventilator, Who Don’t Wake Up
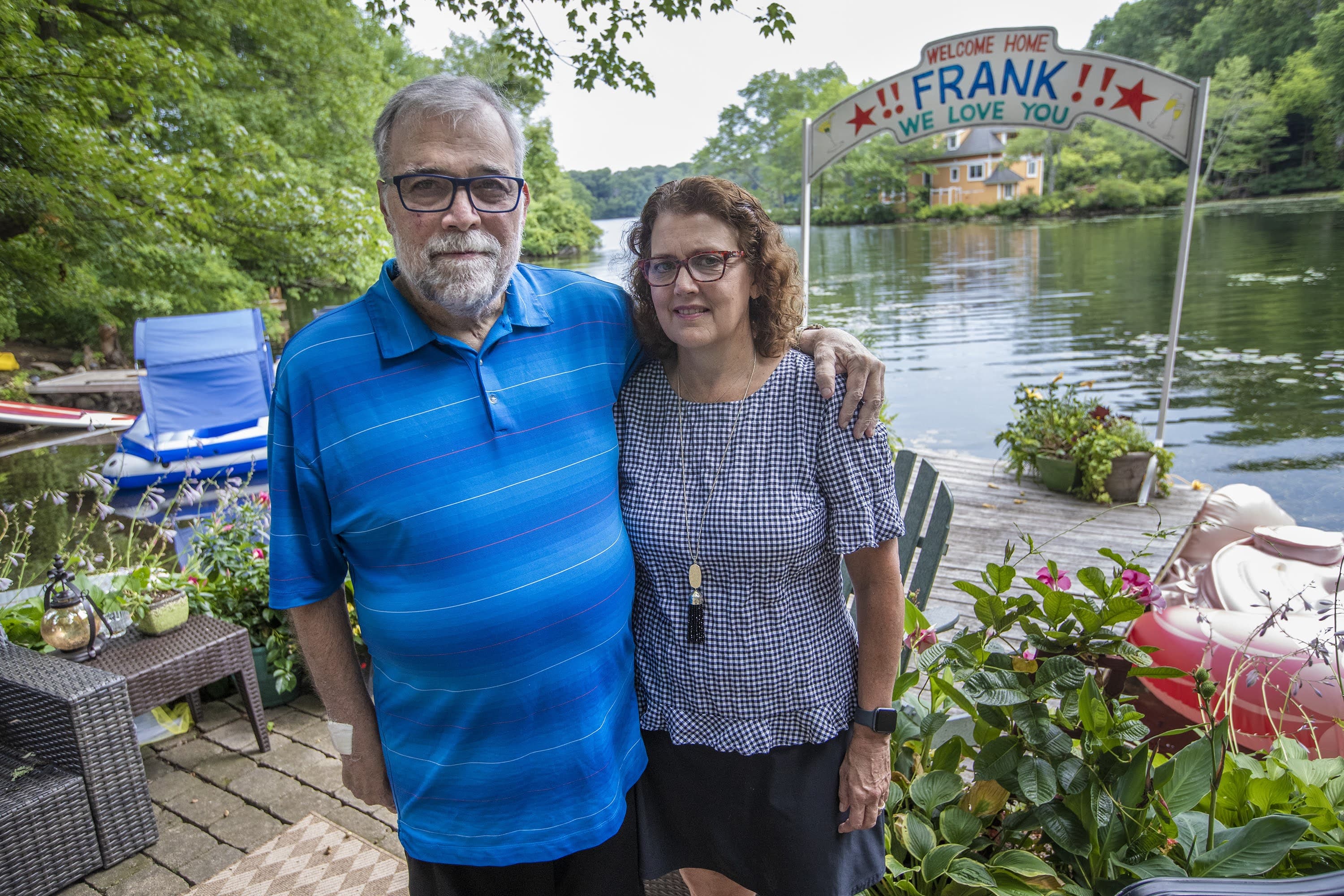
Leslie Cutitta said yes, twice, when clinicians from Massachusetts General Hospital called asking if she wanted them to take — and then continue — extreme measures to keep her husband Frank Cutitta alive.
The first conversation about whether to let Frank go or try some experimental drugs and treatments was in late March. The second in early April.
“Frank used to joke that he wanted to be frozen, like Ted Wiliams, until they could figure out what was wrong with him if he died,” said Leslie Cutitta. It wasn’t a serious end of life wish, but Cutitta knew her husband would want every possible life-saving measure.
So the Cutitta’s and a small army of caregivers hung on. On April 21st, after 27 days on a ventilator, Frank’s lungs had recovered enough to remove the tube. Patients coming off a ventilator typically take hours, maybe a day, to clear the drugs that helped them tolerate the machine. But with COVID-19, some patients remain in what’s being called a prolonged or persistent coma for days, weeks, or longer.
Frank Cutitta, who is 68, didn’t wake up.
“It was a long, difficult period of not, just not knowing whether he was going to come back to the Frank we knew and loved,” said Leslie Cutitta. “It was very, very tough.”
Frank’s unresponsive condition prompted another conversation about whether to continue life support.
“If it looks like Frank’s not going to return mentally, and he’s going to be hooked up to a dialysis machine for the rest of his life in a long term care facility,” Leslie Cutitta recalled a doctor asking, “is that something that you and he could live with?”
Leslie Cutitta struggled to imagine the restricted life doctors said Frank might face. She couldn’t see Frank in person; hospital visits were banned. But every day, sometimes several times a day, she would ask Frank’s doctors, for more information: What’s going on inside his brain? Why is this happening? When might something change?
The candid, consistent answer was: We don’t know.
“Because this disease is so new and because there are so many unanswered questions about COVID-19, we currently do not have reliable tools to predict how long it will take any individual patient to recover consciousness,” said Dr. Brian Edlow, a critical care neurologist at Mass General.
Offering guidance to families is even more challenging. Some patients at Mass General have been removed from life support and died. Edlow can’t say how many.
“It is very difficult for us to determine whether any given patient’s future will bring a quality of life that would be acceptable to them,” Edlow said, “based on what they’ve told their families or written in a prior directive.”
There are lots of theories about why COVID-19 patients may take longer to regain consciousness, if they wake up at all. COVID-19 patients appear to need larger doses of sedatives while on a ventilator, and they’re often intubated for longer than typical periods of time. Low oxygen levels due to the virus's effect on lungs may damage the brain. Some of these patients have COVID-19 related inflammation that may disrupt signals in the brain, and some have blood clots that have caused strokes
“So there are many potential contributing factors,” Edlow said. “The degree to which each of those factors is playing a role in any given patient is still something we’re trying to understand.”
One of the first questions researchers hope to answer is how many patients end up in this prolonged, sleep-like condition.
“In our experience, approximately every fifth patient that was hospitalized was admitted to the ICU and had some degree of disorders of consciousness,” said Dr. Jan Claassen, the director of neurocritical care at New York’s Columbia University Medical Center. “But how many of those actually took a long time to wake up, we don’t have numbers on that yet.”
An international research group based at the University of Pittsburgh Medical Center expects to have initial numbers on COVID-19 brain impacts, including persistent comas, in September.
To try to get a handle on this problem at Columbia, Claassen and colleagues created a coma board that continues to meet weekly. Claasen says he’s guardedly optimistic about the prospects for recovery in some of these patients. A study he published in 2019 found that 15% of unresponsive patients showed brain activity after verbal commands. A case reported by Edlow in July tracked a patient who moved between a coma and minimal consciousness for several weeks and was eventually able to follow verbal commands.
This Spring, as Edlow saw dozens of Mass General patients linger in this unresponsive state, he joined Claassen and other colleagues from Cornell’s Weill Medical College to form a research consortium. Researchers are sharing data to determine the cause of this condition in COVID-19 patients, better predict which patients might recover and find treatments.
The global research effort has grown to include more than 222 sites in 45 countries. Prolonged or persistent comas are just one area of research, but one that is getting a lot of attention.
Dr. Sherry Chou, a neurologist at the University of Pittsburgh Medical Center who leads the international effort, says it will be challenging to uncover what’s happening here as quickly as patients need the information.
Families want to know “whether a patient can wake up and be themselves”. Chou says. Answering that question “depends on how accurate we are at predicting the future, and we know we’re not very accurate right now.”
A CT scan of Frank Cutitta’s brain showed some residue of blood clots but was otherwise “clean.”
“From what they could tell there was no brain damage,” Leslie Cutitta said.
And then on May 4th, after two weeks of no signs that Frank would wake up, he blinked. Leslie and her two daughters watched, via FaceTime making requests: “Smile Daddy” and “Hold your thumb up."
“At least we knew he was in there somewhere,” she said
A week later, the Cutittas got to hear Frank’s voice.
“We’d all be pressing the phone to our ears, trying to catch every word,” Leslie Cutitta recalled. “He didn’t have a lot of them at that point, but it was just amazing, absolutely amazing.
Frank Cutitta spent a month at Spaulding Rehabilitation Hospital. He’s back home in Wayland now, doing physical therapy. He says he slurs words every now and then but has no cognitive problems.
While in the ICU, Cutitta’s nurses would play taped messages from his family, as well as some of Cutitta’s favorite music from the Beach Boys and Pavarotti. Frank Cutitta says he believes the flow of these inspiring sounds helped maintain his cognitive function.
The Cutittas say they feel incredibly lucky. A doctor told the family that 97% of patients in Frank’s condition in New York, for example, died because hospitals couldn’t devote so much time and resources to one patient.
“If Frank had been anywhere else in the country but here, he would have not made it,” Leslie Cutitta said. “That’s a conversation I will never forget having, because I was stunned.”
Frank Cutitta credits the Mass General doctors and nurses who became his advocates.
It “could have gone the other way,” he said, with clinicians deciding, “look this guy’s just way too sick, and we’ve got other patients who need this equipment, or we have an advocate who says, 'throw the kitchen sink at him,' and we happened to have the latter.”
But as COVID-19 patients fill ICUs across the country, it’s not clear how long hospital staff will wait for those patients who do not wake up after a ventilator tube is removed. Many hospitals use 72-hours, or 3 days, as the period for patients with a traumatic brain injury to regain consciousness before advising an end to life support.
Dr. Joseph Giacino, who directs neuropsychology at Spaulding, says he’s worried hospitals are using that 72-hour model, now, with COVID-19 patients who may need more time.
Some patients, like Frank Cutitta, do not appear to have any brain damage, and whatever caused his extended period of unconsciousness cleared.
“In the absence of very clearly stated desire not to have aggressive treatment,” Giacino said, “we need to really go slow because we are not at a point where we have prognostic indicators that approach the level of certainty that is necessary before making a decision that we should stop treatment because there is no chance of meaningful recovery.”
Doctors interviewed for this story urge everyone to make sure a loved one knows what each of us would expect a “meaningful recovery” to include. Family members should ask doctors about their level of certainty when talking about possible outcomes.
Some medical ethicists are also urging clinicians not to rush decisions about how quickly COVID-19 patients may return to consciousness.
“A significant number of patients are going to have a prolonged recovery from the comatose state that they’re in,” said Dr. Joseph Fins, chief of medical ethics at Weill Cornell Medical College. “This is a time for prudence because what we don’t know can hurt us and can hurt patients.”
Leslie and Frank Cutitta have a final request: Wear a mask.
“This disease is nothing to be trifled with,” Leslie Cutitta said, “it’s a devastating experience.”
Frank Cutitta worries about all of the patients still suffering and those with lasting damage.
“I’m not considering myself one of those,” he said, “but there are many, many people who would rather be dead than left with what they have after this.”
This segment aired on July 24, 2020.
