Support WBUR
Black Americans Tend To Live With Unmanaged Pain When Under-Prescribed Opioids Due To Racial Bias, Experts Say
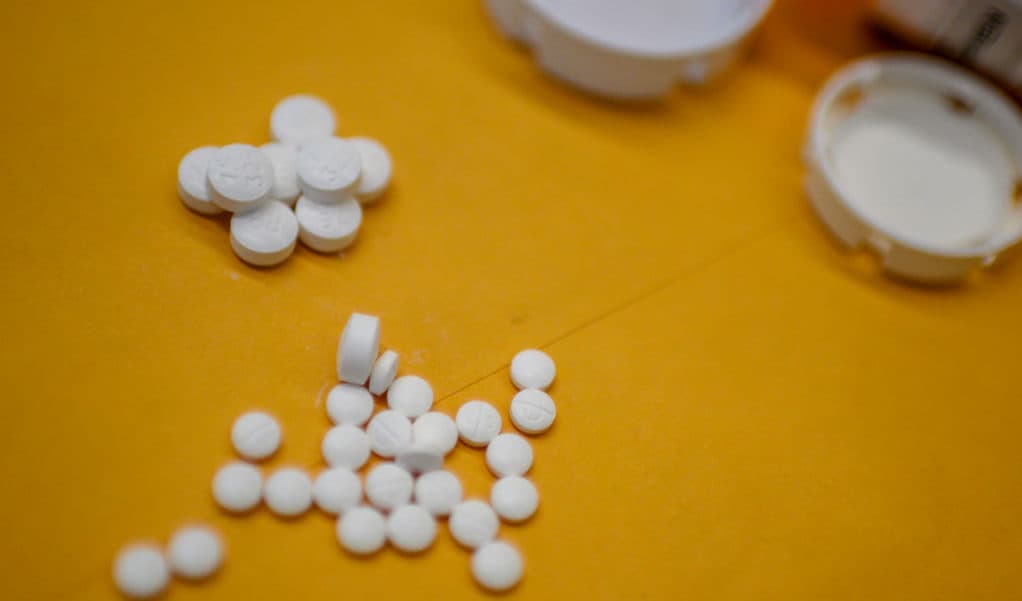
A study published in Epidemiology found because of racial bias, doctors are less likely to prescribe narcotics if a patient is black. Further analysis estimated 14,000 black American lives were spared as a result — a conclusion some experts take issue with because it ignores how much damage racism in health care can cause.
One aspect of this is the harms of being under-prescribed.
Dr. Utsha Khatri, a National Clinician Scholars Program fellow at the University of Pennsylvania’s Perelman School of Medicine, says it’s safe to say that black patients who are under-prescribed opioids end up living with unmanaged pain.
“Black patients are under-treated in pain globally, whether that means opioid analgesics or non-opioid analgesics,” she says.
And that can trigger long term consequences, such as trouble engaging with their families or participating in healing activities like physical therapy, says Shoshana Aronowitz, a doctorally trained nurse, family nurse practitioner and also a NCSP fellow at UPenn.
“I think one of the most troubling possibilities is that people will attempt to self manage pain,” she says. “And this is especially risky now as the availability of counterfeit pills — so pills that look like oxycodone but are actually fentanyl — has increased.”
Interview Highlights
On whether there are alternative pain treatment options and how effective those options are in treating pain compared to opioids
Utsha Khatri: “There are a lot of pharmacological and non-pharmacological pain regimens. And for many acute pain conditions, we often prescribe non-steroidals like ibuprofen. There are other medications like Gabapentin that are good for treating more neuropathic pain. When we talk about non-pharmacological treatments, there's just not a good body of literature, at least that I'm aware of yet. We know that patients anecdotally tell us that they have gotten a lot of relief from treatment regimen such as acupuncture, mindfulness, cognitive behavioral therapy. But in the health care system, we just haven't devoted enough of our resources to really study these treatment options head to head with some of the more pharmacological options we're used to.”
Shoshana Aronowitz: “And I'll just add that we know that physical therapy and acupuncture can be really helpful for patients. But a big issue for a lot of people is access. So they may not be able to afford the treatments. They may not be covered by their insurance or maybe their treatments aren't available in the place they live and they're unable to travel to a provider.”
On how accessible alternative pain treatment options are to black Americans who aren’t prescribed opioids by their doctors
Aronowitz: “There is a little bit of research showing that black Americans are less likely to use or have access to physical therapy or acupuncture — and there are disparities there as well.”
On how the U.S. health care system can address the issue of untreated and unmanaged pain for black Americans
Aronowitz: “The biggest issue I think here is the narrative that there's any sort of upshot to racism in health care. And I think specifically when we're talking about opioid prescribing, first, this ignores how much damage racism in health care causes. But second, it really stigmatizes black Americans who do suffer from opioid use disorder. It's almost like, ‘What's your excuse?’ ”
Khatri: “We know that these disparities exist both with pain treatment disparities as well as opioid use disorder treatment disparities. And when we have these conversations, we have to take targeted approaches to making sure we close them.”
Utsha Khatri, Shoshana Aronowitz and Eugenia South wrote an opinion article for The Philadelphia Inquirer called "The opioid crisis shows why racism in health care is always harmful, never ‘protective’."
Ciku Theuri produced and edited this interview for broadcast with Todd Mundt. Serena McMahon adapted it for the web.
This segment aired on January 15, 2020.
