Support WBUR
Report Finds A 'Mixed Bag' Of Health Outcomes For Mass. Seniors
The mortality rate for Massachusetts residents 65 and older is down, but some specific health problems, like asthma and breast cancer, are getting worse.
Those are among the findings of the 2018 Massachusetts Healthy Aging Data report, out Monday from the Gerontology Institute at the University of Massachusetts Boston.
The report assessed 179 health indicators across 379 communities — including every city, town and identifiable neighborhood in Boston, Worcester and Springfield — and compared them to findings in 2011 and 2015.
Lead researcher Beth Dugan calls the new findings "a mixed bag" of good and bad news. While the overall prognosis is good — Massachusetts is the seventh-healthiest state for older people, according to America’s Health Rankings Senior Report — she says the ranking disguises wide variation within the state.
“We see communities that are disadvantaged in terms of education, income, living in unsafe environments,” Dugan says. “All these social factors end up having consequences for physical health.”
Here are seven takeaways from the report:
1. Massachusetts is getting older and more diverse.
Nationwide, the percentage of the population that’s 65 or older is growing, and Massachusetts is no exception. According to the report, about 15 percent of the state — or more than a million people — falls into this cohort. This is about 125,000 more people than when researchers conducted the last Healthy Aging Report in 2015. Also notable is the growth in what Dugan calls the “youngest older people,” i.e. the aging baby boomers. In 2015, 49.8 percent of senior citizens were between the ages of 65 and 74; this year, that percentage is 55.3 percent.
Other demographic changes to this population include greater racial and ethnic diversity, more education and higher reported income levels.
2. Where you live matters for your health.
Dugan attributes some of the regional differences in health indicators to the rural-urban divide, as seniors in urban areas usually live closer to medical facilities and have an easier time getting to them. But she says some of the outcomes have to do with the communities themselves. For example, does a given community have a higher-than-average crime rate or uneven, pothole-ridden sidewalks? Both of those things can make older people reluctant to go outside and exercise.
The report found that in general, health indicators in the following communities improved the most, since 2015: Brookline, Cambridge, Dartmouth, Falmouth, Gardner, Gosnold, Lynn, Marlborough, Medford, Newton, Peabody and Quincy.
Meanwhile, these communities were among places with worsening health indicators: Arlington, Brockton, Burlington, Fall River, Haverhill, Lawrence, New Bedford, Revere, Swansea and Wareham.
3. Rates of depression among seniors are rising.
In more than 40 percent of communities, rates of depression have "significantly increased" in recent years, according to the report. Overall, 31 percent of Massachusetts seniors have been diagnosed with depression at some point in their lives, and one in four has been diagnosed with anxiety.
Once again, the results were not equal throughout the state. Twenty percent of seniors in Princeton have been diagnosed with depression, whereas in Springfield, that figure is 49 percent.
“Increased risk for depression was associated with higher rates of older residents living alone, dealing with greater levels of chronic disease, and having access to mental health care,” the report says.
The number of seniors with substance use disorders also varies throughout the state. Overall, more than 6 percent of the 65 and older population has a substance use disorder, but the numbers were higher in areas with relatively high crime rates, chronic disease problems and a larger number of seniors who live alone.
4. Specific health challenges are shifting.
Across the state, Dugan and her team found higher rates of arthritis, asthma, atrial fibrillation, breast cancer, chronic kidney disease, depression, endometrial cancers, benign prostatic hyperplasia, high cholesterol, hypothyroidism and lung cancer.
What they didn't find is any indication as to why.
"We have guesses, but we can't really make definitive determinations at this point," Dugan said. "It could be that we're getting better with our diagnosis, or there could be less stigma and more awareness that treatment options are available and people are trying to get help. Or it could be that the conditions are increasing. So we have lots of guesses, [but] we don't really know why"
The good news? Rates of congestive heart failure, ischemic heart disease and heart attacks are down. Same goes for chronic obstructive pulmonary disease, anemia, colon cancer and prostate cancer. Also down are the number of people with multiple comorbidities, a fact Dugan calls “encouraging.”
5. Gateway Cities have generally worse health indicators.
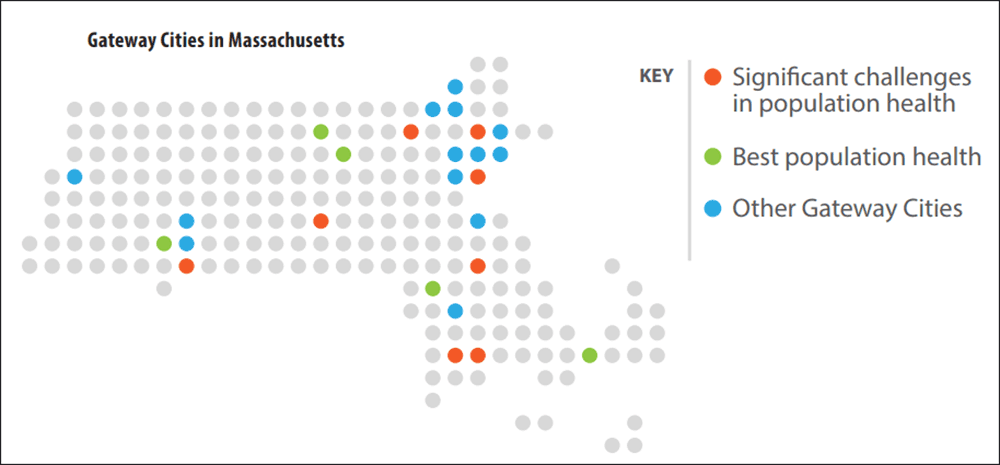
Of the state’s 26 Gateway Cities — urban centers that were once industrial hubs — almost all have significant economic and social challenges. And according to the report, “the population health of older adults is poorer in Gateway Cities than in other Massachusetts communities.”
But again, the problem is not uniform. Seniors in Brockton, Chelsea, Fall River, Lowell, New Bedford, Peabody, Springfield and Worcester score lower than the state average on dozens of health indicators. Brockton and Fall River are at the bottom of the list. Still, some of these locations have seen modest improvements since 2015, namely Worcester, New Bedford, Springfield and Peabody.
In short: “The results suggest Gateway Cities should be a focus of population health efforts as well as economic development initiatives," the report says.
6. There are health disparities between racial and ethnic groups.
After noting that there is considerable variation in health within any given racial or ethnic group, the report found the following about seniors in Massachusetts:
- Those of Asian descent tend to be healthier than others in the state.
- When compared with other groups, Hispanics had the greatest health improvements in recent years.
- African-Americans and Hispanics had higher rates of obesity, hypertension and chronic kidney disease than white seniors.
- Whites had higher rates of leukemia and other lymphomas, lung cancer, colorectal cancer, breast cancer and endometrial cancer.
- Whites had lower rates of dementia, epilepsy, glaucoma, mobility impairment, substance use disorders and schizophrenia than African-Americans and Hispanics. (They did, however, have higher rates of other personality disorders.)
7. When compared to other New England states, older Massachusetts residents fare better in some ways, and worse in others.
Since the last report in 2015, Massachusetts saw 14 health indicators improve and 16 worsen. According to the report, a similar pattern of changes was seen in other New England states, “[suggesting] that similar factors are influencing the population health of older adults in the region.”
That said, Massachusetts seniors had higher rates of chronic kidney disease, schizophrenia and other psychotic disorders, deafness or hearing impairment, and blindness or visual impairment than other states in the region.
Overall, Dugan says, Massachusetts is moving in the right direction when it comes to a growing senior population.
"First of all, most states don't think about the aging population,” she says. “And secondly, they don't think about how they can capitalize on it in terms of economic development. So I think we're ahead of a lot of states as it is, and then the resources that we have here in terms of academics, the health system, technology and financial services all lends itself to certainly positioning ourselves as the Silicon Valley of aging.”

