Support WBUR
Despite Progress On Diabetes Treatments, Study Finds American Patient Health No Better
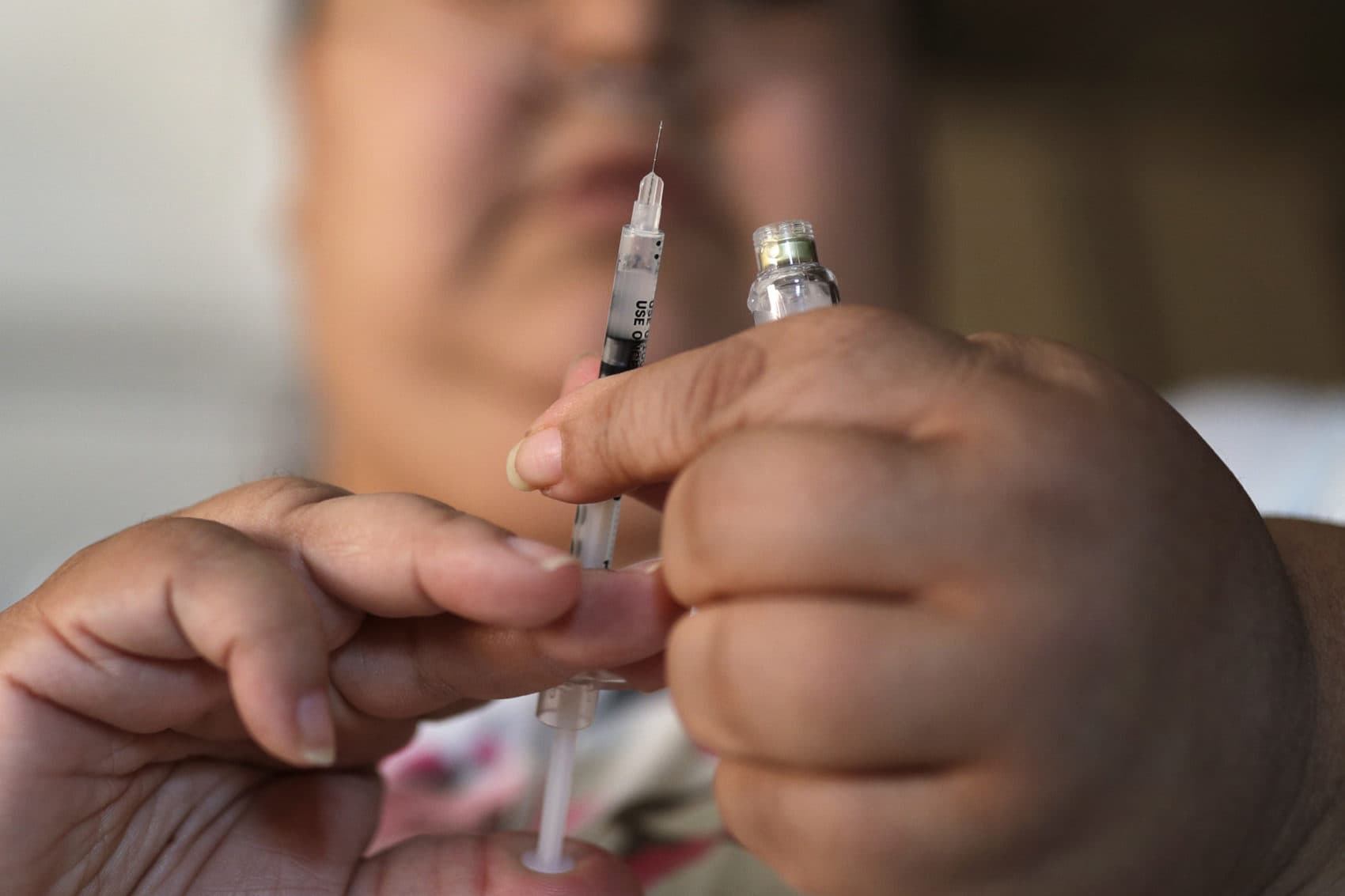
Recent progress on treatments for diabetes has not translated into better patient health nationwide, according to new research from Massachusetts General Hospital.
The study in the journal JAMA Internal Medicine looked at whether diabetes patients controlled their blood sugar and blood pressure, took drugs to lower their cholesterol, and stayed away from smoking. It found that among more than 1,700 representative patients, only 23% hit all four of those goals — no better than 15 years ago.
Lead author Pooyan Kazemian says there's been a heavy focus on better drugs and devices, "but maybe not enough attention has been given to actually making sure people are receiving these new tools and technology."
The study finds that younger adults, women and nonwhite patients have the biggest gaps in diabetes care. Dr. Kazemian describes the study, beginning with its background, in edited excerpts of our conversation below.
PK: There have been major advances in diabetes drug discovery, and movement to develop innovative care delivery models, over the past two decades. However, it was not known if these new advances and innovations have reached the U.S. population at risk.
In this study, we used 2005-to-2016 nationally representative survey and examination data from the Centers for Disease Control and Prevention. We conducted a statistical analysis to evaluate what proportion of U.S. adults with diagnosed diabetes achieved diabetes treatment targets. The treatment of diabetes is generally focused on meeting four targets: controlling blood sugar, blood pressure, cholesterol level, as well as promoting smoking cessation.
In this analysis, we found that among U.S. adults with diagnosed diabetes, only 23% achieved a controlled level of blood sugar, blood pressure, cholesterol, and do not smoke tobacco. In other words, fewer than one in four American adults diagnosed with diabetes achieved the diabetes care targets recommended by the American Diabetes Association.
Certain populations demonstrated persistent disparities in meeting diabetes care targets: younger-age adults, females and nonwhite adults with diabetes had lower odds of achieving diabetes care targets.
What are examples of recent progress on treatments?
In the early 2000s, there were new diabetes drugs developed to target and control high blood sugar. These are classes of drugs that are added to the drug metformin for better glycemic control. These are supposed to work really well, but our results show that these drugs have not reached the population at risk, and they have not been able to improve outcomes in the United States.
There have also been some innovative care delivery models such as, for example, continuous glucose monitoring devices. And there are innovations too — for example, to remind patients to take their medicine on time and then follow up with patients individually.
What's your best explanation for this incredibly disappointing finding?
One of the main findings of this study was that insurance coverage turned out to be the strongest indicator for achievement of diabetes treatment targets. Therefore, I believe by making health care more affordable and accessible, we can take an important step towards improving diabetes outcomes in the United States.
But you have less than a quarter of people achieving the four goals and yet the vast majority of Americans have some kind of health insurance coverage. So how do you explain that?
It is not only having health care. The high drug costs in the United States are also a barrier to access to health care. And the health care should also be efficient, and it should be personalized to patient needs.
What are the biggest factors in the failure of most people to reach those targets?
We find in the past 15 years, cholesterol control was consistently the least controlled parameter in diabetes care. And we found that less than six in 10 American adults with diabetes are taking a statin, a medication that can help control cholesterol levels. It should be 10 of 10 or very close to that. Glycemic control was also about seven in 10. But that is probably less important than cholesterol control.
One other interesting finding of our study was that the rate of diagnosis was not very high either. We find that one out of four American adults with diabetes are not aware of the disease and so they are not receiving care.
Any other policy implications?
Our findings indicate an immediate need for better approaches to diabetes care delivery, in particular reaching under-served populations with persistent disparities in care. I also believe that we should continue monitoring the achievement of diabetes care targets on a national level.
Were you surprised by the findings?
To be honest, I was surprised. There was another study done in the early 2000s that showed that the achievement of diabetes outcomes improved in the United States from the late 1990s to early 2000s. So when I was conducting this analysis, I was kind of expecting that maybe things would have improved a little bit in the past 15 years. But that was not the finding of this study, unfortunately.
There is a lot of talk about cool new technological solutions for diabetes like the artificial pancreas. But your findings would seem to suggest that a big part of the problem is much lower tech — that it's basically money.
Exactly. We have spent a lot of time and energy and focus on developing new tools and new technologies, but maybe not enough attention has been given to actually making sure that people are receiving these new tools and technology.
