Support WBUR
Coronavirus Coverage
Thinking Through The Unthinkable: How Mass. Hospitals May Decide Who Gets A Ventilator In The COVID-19 Surge

If a hospital has more critically ill patients than it can manage, who gets an intensive care bed and who doesn’t? Who gets a ventilator?
The Massachusetts Department of Public Health (DPH) is out with guidelines that address some of the most challenging questions doctors and nurses will face during the pandemic.
Released Tuesday, The Crisis Standards of Care guidance says those questions will be answered with the goal of saving the most years of life. Hospital staff will look at a patient’s chances of both short- and long-term survival.
As the guidelines put it, “such tragically difficult decisions must be based on criteria that ensure that every patient has equitable access to any care from which they might benefit.”
Doctors and nurses should not consider any of a long list of factors, including: race, disability, gender, sexual orientation, gender identity, ethnicity, ability to pay, immigration status or incarceration.
"Every clinician deserves sound guidance should we ever reach that unthinkable moment when our health care resources are stretched beyond their limits,” says Dr. Michael Wagner in a statement. Wagner co-chaired the Massachusetts Crisis Standards of Care Advisory Committee.
Under the guidelines, hospitals will create a team to make decisions about who gets scarce resources. That team will not include the doctors and nurses who are caring for the patient.
Team members will use a scoring system. They may reassess patients who are already in an ICU. If the team recommends withdrawing life support for use with a patient who has a better prognosis, the patient who is being moved off life support, or their designated proxy, could appeal.
When creating a score for critically ill adult patients, a hospital team will consider the state of a patient’s organs and whether they have a chronic illness or condition. Pregnant patients and first responders will be given a priority score. In the event of a tie, the youngest patient would likely get the ICU bed or ventilator.
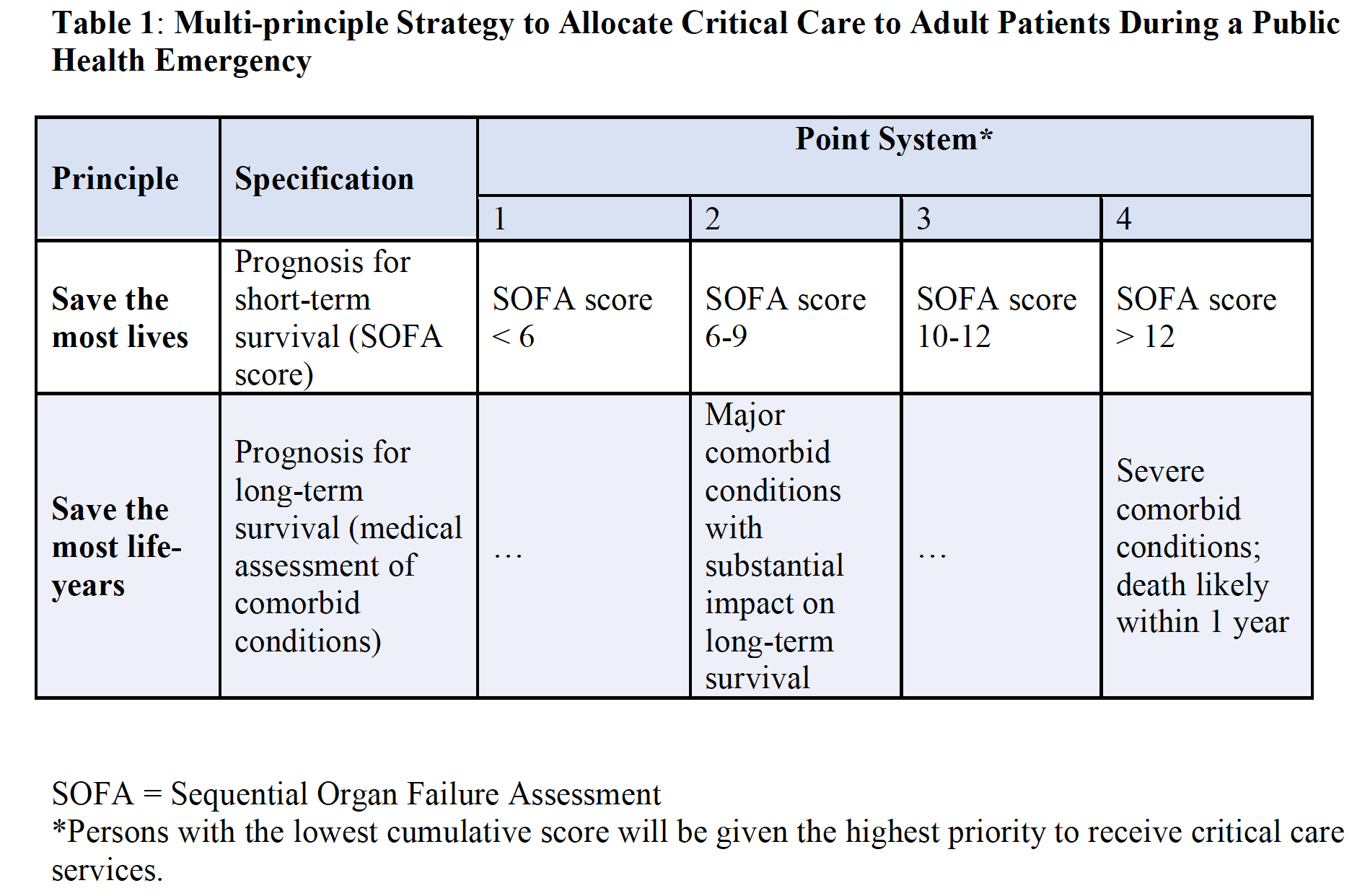
The Massachusetts guidelines closely align with those proposed in JAMA Network in late March. Hospitals across the country are wrestling with these questions. DPH says it created the committee and this report on crisis care at the request of the hospital and provider community.
“The guidelines just released are as thoughtful as any that any state has yet produced, because they built from so much important work that other states had done before us,” says Dr. Lachlan Forrow, director of ethics and palliative care at BIDMC and a member of the advisory committee.
The committee included physicians who specialize in emergency preparedness, medical ethics, respiratory care and anesthesia; a nurse; an attorney; and public health officials. There was no one specifically representing the disability community.
Still, Bill Henning, director of Boston Center for Independent Living, says he appreciates the committee’s work, especially the list of factors that cannot be used in determining who receives potentially life-saving care. But Henning, whose organization provides services and advocacy for people with disabilities, says such direct language doesn’t mean providers won’t be biased.
"Historically, there’s been bias against people with disabilities. It’s almost ingrained,” he says. “You’d hate to see that leach into any decisions."
Dr. Robert Truog says that the central message of DPH's guidelines for the public in a pandemic is that "the overwhelming priority is to increase the capacity of medical care so that everyone is able to get what they need."
"But if, and when, that capacity is exceeded, the public should know that we are not flying by the seat of our pants – we have a plan that has been carefully developed by clinicians, ethicists, and members of the public, and that is designed to be as fair, equitable, and non-discriminatory as possible," he added.
A few doctors who declined to speak on the record said they’ve already noticed that providers seem to be trying harder to save younger patients with COVID-19, usually without an explicit intention to do so.
The committee’s work is based on some assumptions about what’s ahead for Massachusetts. A surge of patients may overwhelm the state and regional health care capacity. There may be limited supplies, equipment and staff as clinicians become infected with the virus. Doctors, nurses, physician assistants and others may no longer be willing to report to work.
The guidelines urge hospitals to preserve ICU beds and ventilators by substituting, conserving and reusing supplies when possible. The crisis standard tool “will be triggered only when there is no acceptable alternative, and its use will be discontinued as soon as possible.”
Use of these guidelines will not be mandatory, but the committee says the intent is that all hospitals and providers will make consistent decisions.
“Most importantly, maintaining the trust of the public requires that the allocation of scarce critical resources should be uniform across the Commonwealth,” the committee wrote.
The report says DPH will monitor ICU-level care across the state and try to avoid the need to make decisions about who gets it and who doesn’t.
This article was originally published on April 07, 2020.
