Support WBUR
Coronavirus Coverage
Fear Vs. Need For Care: How Fast Will Patients Come Back?

As doctors, nurses and physician assistants open appointments for non-urgent care, the big question is: will patients come back and how fast? One answer, in a study of data from more than 50,000 providers, is both hopeful and sobering. From a low-point in early April to mid-May, about 50% of patient visits were back. But even with that rebound, patient volume is still about 30% lower than it was before the coronavirus began tearing through the U.S. health care system.
“There is a bounce back, and that’s important both for patients’ health as well as the financial difficulties that practices are in,” said study co-author Dr. Ateev Mehrotra, an associate professor of health policy and medicine at Harvard Medical School.
But Mehrotra said the relatively rapid return of some patients does not mean the dramatic, 60%, decline in visits during the COVID-19 surge has evaporated.
“That’s certainly not the case,” he said.
The analysis uses patient registration, payment and other interactions managed by Phreesia, a health care technology company, whose software is used by medical practices in all 50 states.
The most pronounced rebound so far is in Texas, Oklahoma, Alabama and Mississippi. Patients appear to be slower to return in New England and the Mid-Atlantic states.
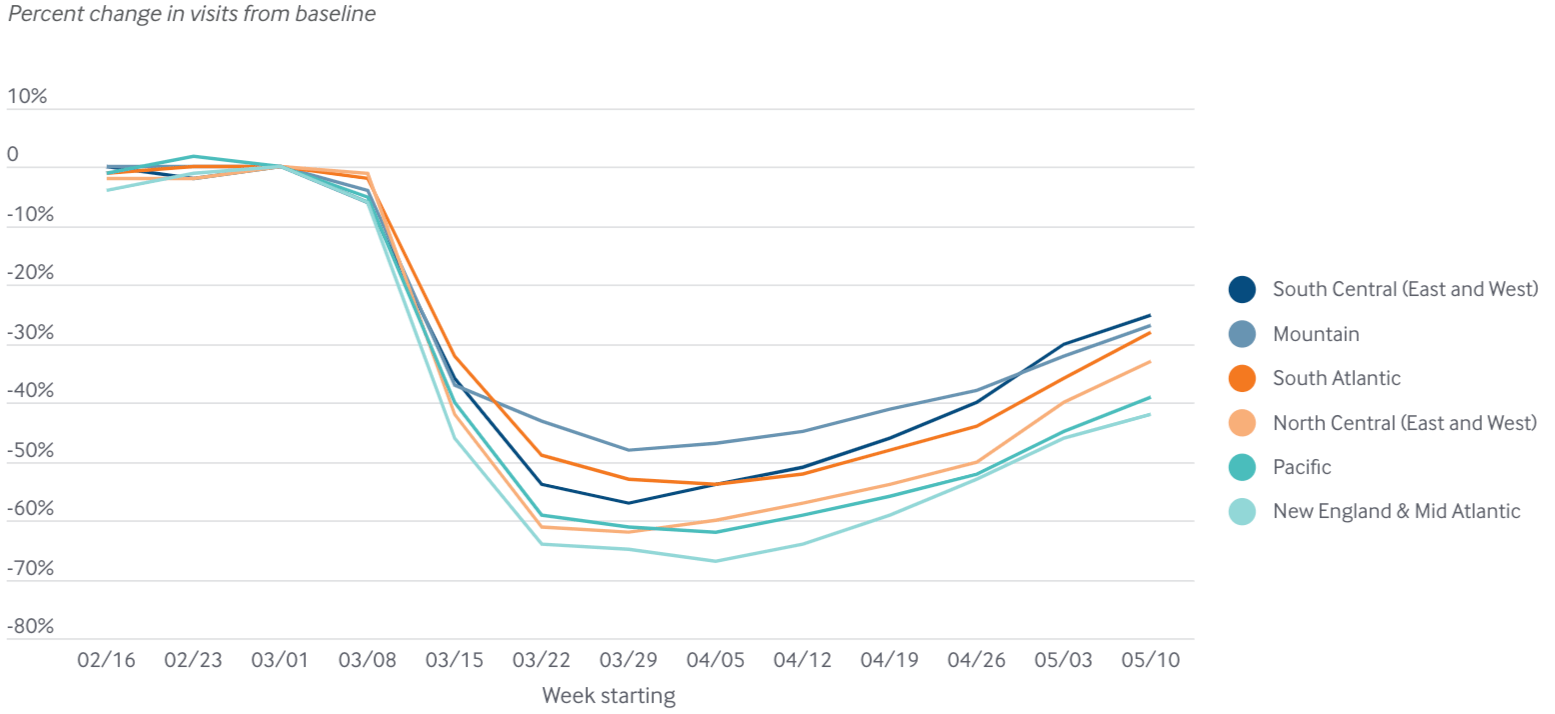
Across the country, patients are returning more often for in-person visits, as compared to telephone or video appointments, which may have plateaued. All specialties are seeing more patients again although the loss remains most pronounced for opthamologists, ear, nose and throat specialists and dermatologists. There are more adults and infants coming in for care than children ages 3-17.
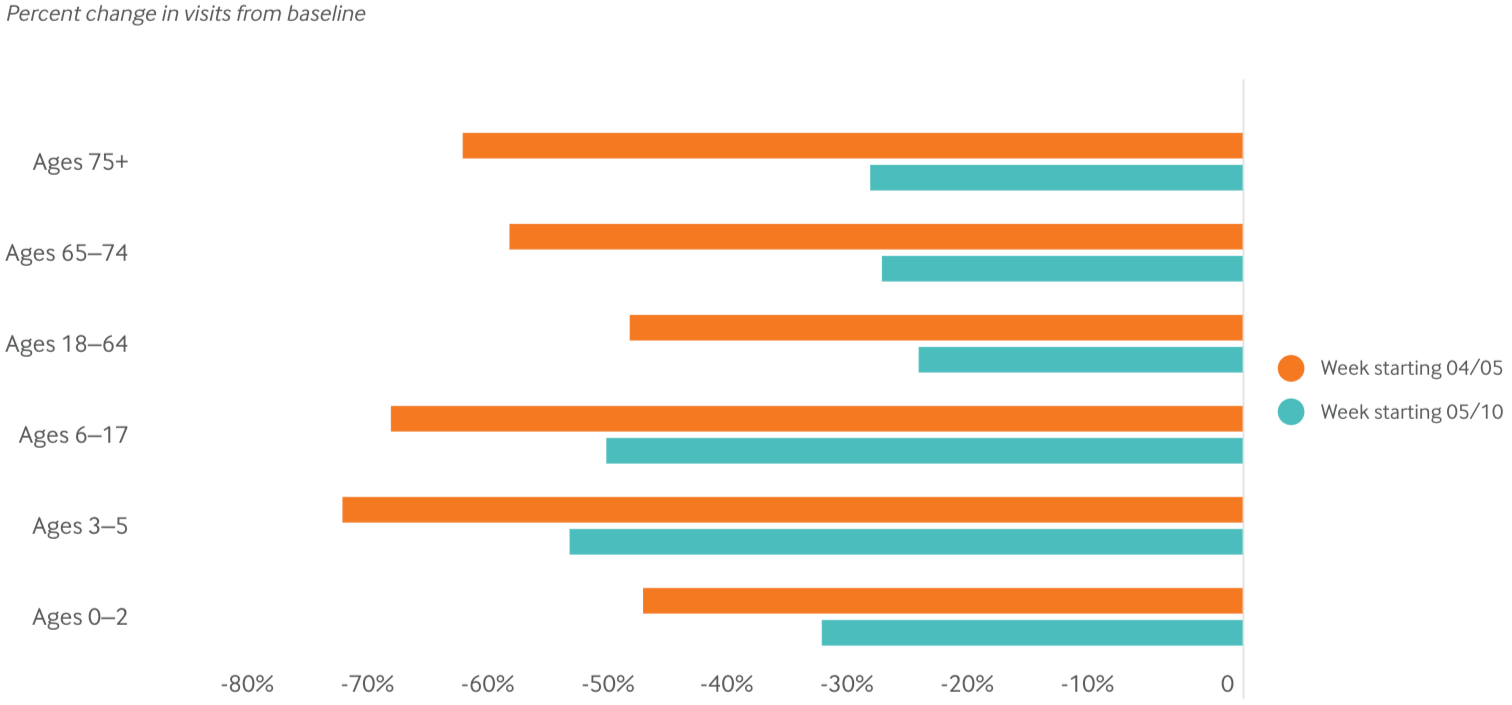
Mehrotra said the returning adults are likely those with complex chronic illnesses, diabetes or high blood pressure who need to be seen or have a test. In many cases, providers are reaching out to these patients, encouraging them to come in. And the fear of going into a clinic or doctor’s office may be waning for adults with pent up needs.
“As the pandemic has progressed, we see this general sense that people are going out more than they were previously,” Mehrotra says, “and we’ve started to accept this new strange and scary normal.”
But that fear may be growing for parents as they read about an emerging coronavirus threat to children.
While this snapshot of outpatient care offers some good news for struggling practices, there are still deep concerns about the impact of the pandemic on some specialists and primary care providers. In a survey earlier this month, 42% of them reported layoffs. American Medical Society leaders said during a recent webinar that most primary care clinicians worry about whether they can remain open into June.
A bill approved in the U.S. House includes specific assistance for primary care providers. In the Senate, Republican leaders are refusing to consider the measure. They say much of the $3 trillion package is not relevant to the pandemic.
