Support WBUR
Partners Ramps Up Coronavirus Testing Of Patients As Hospitals Aim To Resume Regular Care
In an effort to safely get its hospitals running at full capacity again, Partners HealthCare is working on plans to increase testing of hospital patients for the coronavirus.
For more than two weeks now, Partners has tested patients whether or not they have symptoms of the coronavirus, and the numbers may be encouraging.
Tom Sequist, Partners' chief patient experience and equity officer, joins All Things Considered to talk about the testing efforts.
Here are highlights of the interview, lightly edited for clarity.
Interview Highlights
On Partners' testing project
We've tested approximately 2700 patients across all of our hospitals during that time period. And we found that among patients who are without symptoms that would otherwise be related to COVID-19, the prevalence of a positive test result is just a little bit north of 1%.
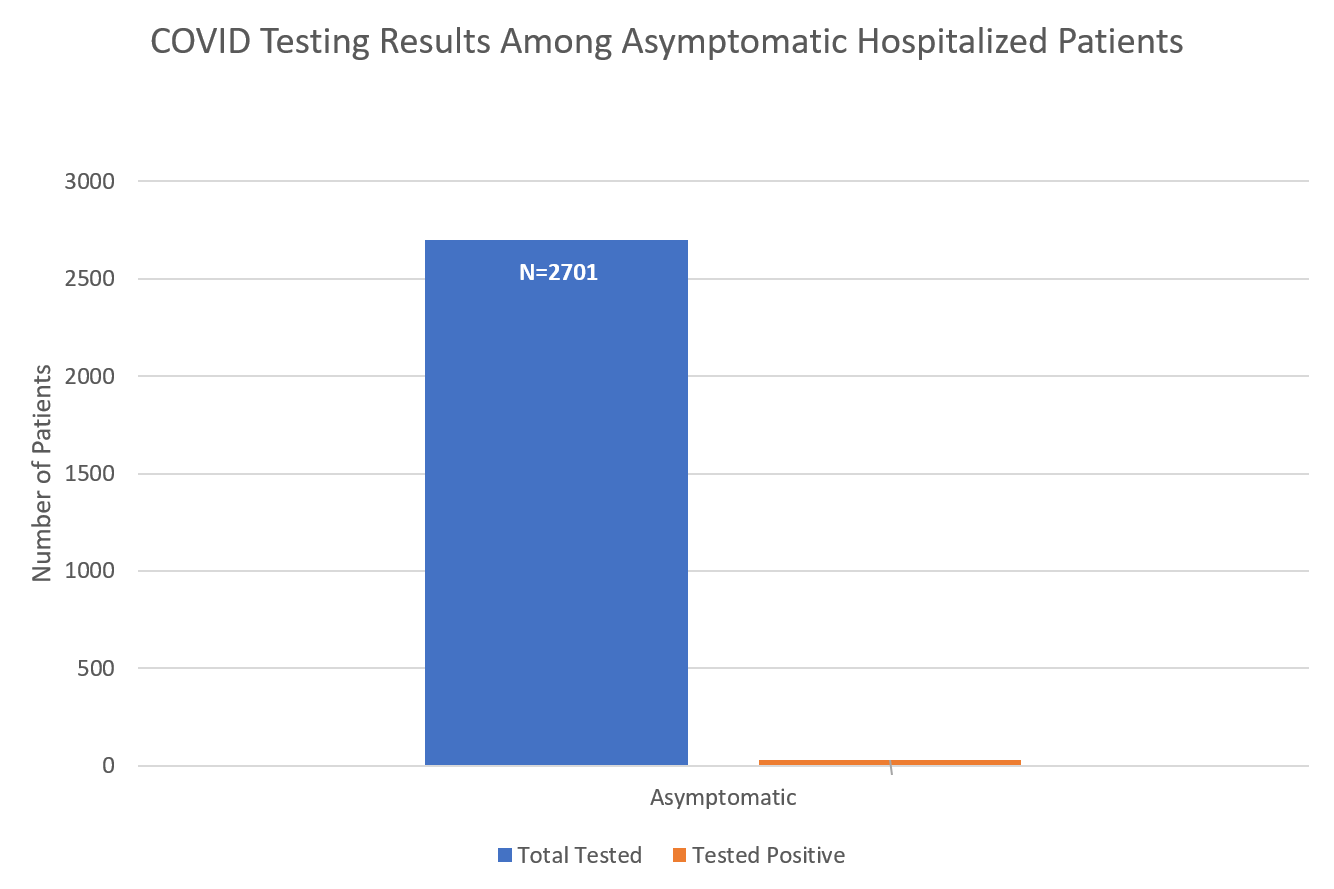
These numbers exclude anybody who came in and had a cough or a fever. People who come into our hospital and had symptoms like that were tested and had been being tested for the past couple of months. The new thing that we started doing a couple of weeks ago is to test everyone who is coming in without a symptom so that we can get an idea of what the prevalence of infection was in the community among these asymptomatic, lower-risk patients.
On what the testing numbers mean
This low prevalence of 1% in the community really gives us a lot of helpful information to help alleviate some of the concerns that people may have, but also will help us direct care better. So when you combine the fact that someone doesn't have symptoms and the fact that they have a negative COVID test with the fact that they live in a community where the prevalence is only 1%, you can have actually a much higher level of confidence that there is not some underlying covered infection that we have not detected.
It's not that it's so much that it makes it safer. It expands our options for how we can care for our patient populations. So it expands our options in terms of where we can provide the care and the types of personal protective equipment that we might be able to use, which we think in the long run is going to be the way that we're gonna want to be able to tailor the care that we're giving patients, that ultimately will keep people safe.
On the future of the testing project
So our plan moving forward is to continue to test every patient who's admitted to the hospital, whether they are symptomatic or asymptomatic. We also regularly screen every day every patient in our hospital for symptoms that might be related to COVID so that if they do develop symptoms, we can take immediate action on that. And we further have the capability and the capacity to do COVID testing for our ambulatory patients who are either symptomatic or who are undergoing different types of care and treatment, where we really do need to know what their COVID status is.
On the lack of "herd immunity" reflected in the data
I don't think that these data represent anything bad. What they are really telling us and what we are using them for is, how do we direct patient care in our hospitals and clinics and how do we make sure that our providers that are health care, frontline health care workers and that patients are receiving, you know, the personal protective equipment they need and being cared in the environment that they should be? That's a little bit of a different question than whether or not our community at large is achieving herd immunity. That's a process that's actually going to take a longer period of time to achieve. But before we can achieve herd immunity, which I think is going to be further out in the future, what we know from these data is that we can safely direct care for our patients and our providers.
This article was originally published on May 22, 2020.
This segment aired on May 22, 2020.

