Support WBUR
'Forever Altered': Health Care Workers Face Mental Health Struggles After Caring For COVID Patients

Boston Medical Center trauma surgeon Dr. Tracey Dechert is used to tragedy. She has to rush into operating rooms to perform complex surgeries on people who've been in terrible accidents or shot, or have suffered other trauma and the outcome isn't always good.
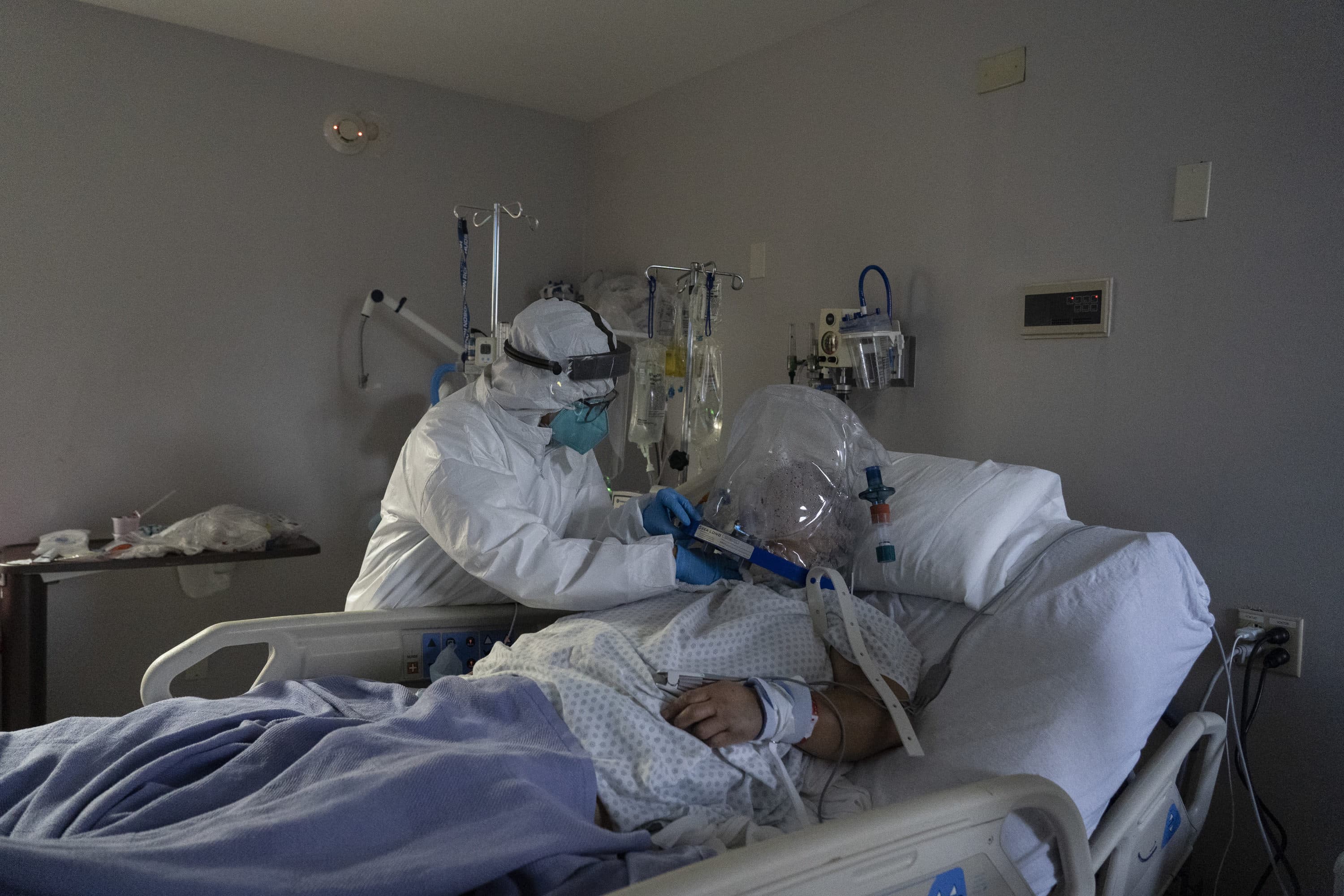
But when she oversaw a COVID-19 intensive care unit at BMC for a couple of months, she was overwhelmed by the quiet of the floor. Patients were walled off in their rooms, alone, with no family. Dechert and her colleagues had to cover themselves from head to toe in personal protective equipment to enter the rooms and approach the patients.
"It's just something so sad and eerie — even when you do touch them, it's through, you know, gowns and gloves and hats and masks," Dechert said. "And it's almost as if it's not as human. And that is disturbing."
It was impossible for her to leave the sadness and grief behind, even after her 12-hour shifts ended.
"... You can be exhausted emotionally. That actually feels physical."
Dr. Tracey Dechert
"It was pretty awful," Dechert recalled. "The patients I was taking care of, most of them died. ... It was so many, all at the same time, all from the same disease. ... Normally we do have patients who are getting better, and they're the ones that keep us going and get us through the tough patients who maybe don't get better. ... So you had no little thing to hang onto to keep you going, and then that just builds."
When she woke up on days she was working in the COVID ICU, Dechert said, she felt "dread."
"It was depressing to ... think all the work we are doing wasn't helping enough people," she said. "It helped some, for sure. But ... it was tough to keep going back in.
"And then you're getting tired because you're working so hard," she added. "So then it seems like as you get more tired, you get more discouraged. You know, it kind of builds on itself. ... You can be exhausted emotionally. That actually feels physical."
'A Pandemic Of Mental Health Issues'
Some health care professionals are worried the immense stress and grief that nurses, physicians and other front line medical workers are experiencing will lead to a wave of mental health issues among people in the field. Published research on the impact of the pandemic on health care workers in the U.S. is very limited at this point.
Some surveys have found significant rates of acute stress, depressive symptoms and anxiety during this and other outbreaks. Research in China points to considerable distress among medical workers caring for COVID-19 patients. A study in Italy found female health care workers experienced more heightened psychological effects than males.
Dr. Beth Lown, chief medical officer at The Schwartz Center for Compassionate Healthcare in Boston, said she's hearing accounts of "tremendous psychological distress" in the industry, particularly among those directly taking care of people with COVID-19 or working in emergency departments.
"There is this phenomenon that occurs [that] experts in trauma have described, where at the beginning [of a large-scale medical event], there's a heroic and a sort of a honeymoon phase where people do rush forward to want to help. And we certainly have seen that," Lown explained. "But then the longer the disaster persists, people over the course of time will start to become demoralized, disillusioned, even despairing, and start to really spiral down."
She said she fears health workers will face "a pandemic of mental health issues and crises," including medical professionals leaving the industry and higher risks of suicide and post-traumatic stress disorder.
The Schwartz Center offers seminars and support services to highlight and increase the compassionate side of the care medical workers give — both toward patients and toward themselves. Several hundred medical institutions in the U.S., Canada, Australia and New Zealand take part in the organization's Schwartz Rounds program. Workers at the hospitals and clinics get trained to facilitate sessions in which colleagues share stories regarding the emotional, human side of their medical cases and how their patients, the patients' families and they themselves have been affected.

During the coronavirus crisis, the sessions have switched from in-person to virtual. Some of the meetings have had upwards of 800 health care workers from a particular institution gathered on Zoom or another online platform to share their experiences and feelings, according to the Schwartz Center. Subjects range from navigating loss, grief and uncertainty to concerns over bringing the coronavirus into one's home.
Dr. Lown, who has hosted multiple Schwartz Rounds sessions at Mt. Auburn Hospital during the pandemic, said many medical practitioners are expressing a feeling of being "de-skilled" in the face of COVID-19.
"I remember talking to a palliative care physician colleague who said one of the things she's [normally] most proud of is her ability to prognosticate and to communicate that in a caring and compassionate way with family members," Lown said. "And that just was completely impossible [with COVID-19] because of the uncertainty ... in terms of prognosis. No one could really predict who is going to survive and and who was not."
Dechert, who will be a presenter in a Schwartz Rounds session for BMC employees in early September, can relate. Although certain aspects of coronavirus complications such as pneumonia are very familiar to doctors, she pointed out, there are many facets of the disease that are different from anything they've previously encountered.
"So as you're caring for the patients, you're kind of figuring that out as you go," she said. "That's not usually a way we practice medicine, of course. So that feels uncomfortable for us because it's not how we trained and not how we practice."
"Something's changed and something still is not right, or it's just kind of forever altered after going through COVID ... Things I'm really passionate about and I love to do, the passion is not quite there."
Between shifts, Dechert said she would go home, where she entered through a different door and stayed on a different floor than her husband, a psychiatrist. Not only did she worry about transmitting the virus to him, but she couldn't get the support she would typically get from him.
They rented a little place in Rockport for her to "escape," she said. Walking and being out in nature are the things she says come closest to clearing her head.
"I find that I can't concentrate. So, I normally love to read and do other things," Dechert said. "But I'm finding that hard to do right now. So [I do] things where I just sort of sit and look at the ocean or take a walk or a hike. Pretty basic things."
After taking care of patients in the COVID unit, she went right back to her normal work doing trauma surgery and overseeing a surgical ICU.
But, she said, the psychological effects of the previous two months remained with her.
"Something's changed and something still is not right, or it's just kind of forever altered after going through COVID. There really was no down time to think or process or reflect on what we all had just been through," Dechert said. "And then with the idea that it can come back at any moment ... I mean, if someone could promise me I would never do this again, I think I'd have an easier time getting back to my normal self in my normal work and feeling good."
Dechert said, for the moment, she is struggling to find joy in her day-to-day life outside of work and to feel passionate about professional endeavors she used to love.
"You know, teaching or mentoring, I'm trying. Of course, you want to do your best, but it just feels like I'm going through motions and my heart's not quite in it the way it would normally be," she explained. "And so I've just got to figure out how to get that back."
Seeking Care For The Caregivers
There are cultural barriers to health care workers in need of psychological or psychiatric help, according to Dr. Lown of the Schwartz Center.
"I think that we are trained as health care professionals not to complain, to compartmentalize our feelings and to not reach out for help. And that is really a significant problem," Lown explained. "We need to really address the stigma of feeling vulnerable, weak and the stigma of needing care for mental health issues. It is really counterproductive and will have significant negative outcomes for our health care workforce."
Toward that goal, the Schwartz Center is training hospital teams to implement another psychological peer support program called Stress First Aid, which was first developed by the National Center for PTSD, a division of the U.S. Department of Veterans Affairs. It's meant to help identify health care workers who are suffering psychologically and help them connect with coping tools and resources.
Such outreach can also help reduce medical errors and keep people in the health care industry, according to Lown, who stressed that burnout is correlated with medical mistakes and people leaving the field.

Dechert said she considers herself very lucky to work with a great group of colleagues who are open about their emotions and the help they are seeking.
"That is huge, for sure," she said. "If I felt isolated and didn't have partners that were supportive — and not just supportive, but, like, really caring and loving people — I definitely couldn't get through this."
But she acknowledged she might need other forms of help, and the thought of leaving medicine has flitted through her mind.
"It just feels as if there's this huge weight, like, right above our heads," she said. "If [a spike in COVID-19] comes again ... I don't know how many more surges I could do."
Resources: Anyone in mental health crisis can contact the National Suicide Prevention Lifeline at 1-800-273-TALK (8255) and the Samaritans Statewide Hotline (call or text) at 1-877-870-HOPE (4673). Call2Talk can be accessed by calling Massachusetts 211 or 508-532-2255 (or text c2t to 741741).
This article was originally published on August 25, 2020.
This segment aired on August 25, 2020.

