Support WBUR
Coronavirus Coverage
With Rise In Variants, Mass. Scientists Warn Of Evolutionary Arms Race Between Virus And Vaccines
The original coronavirus is being overtaken in Massachusetts by newer and more infectious variants. The Broad Institute of MIT and Harvard regularly sequences the genomes of coronaviruses taken from COVID-19 patients and, lately, the analyses have been showing more of these variants than the original or "wild-type" strain, which contains no major mutations.
“In the past few weeks and as of last night in particular, we are seeing over 50% of the cases we are sequencing at the Broad being variants of concern,” Bronwyn MacInnis, a genomicist at the Broad Institute, said at a state legislative hearing on Tuesday. “A large proportion of those being the B.1.1.7 variant first identified in the U.K., but also P.1, the variant first identified in Brazil.”
These variants are circulating through Massachusetts communities now, MacInnis said, and will likely continue taking up a greater proportion of COVID-19 cases in the state. Throughout the hearing, in which some of the state’s top epidemiology and infectious disease experts testified, scientists highlighted data suggesting the newer variants may be more transmissible and could be better able to resist COVID-19 immunity from the vaccines or a natural infection.
“Many of these variants show enhanced transmission and, in some studies, enhanced disease,” Dr. Dan Barouch, an immunologist at Harvard Medical School who helped develop the Johnson & Johnson vaccine, said at the hearing.
Barouch mentioned several concerning variants including the P.1 strain first identified in Brazil and domestic mutations that have emerged in California and New York, noting these variants “also have the property of being able to partially evade antibodies, and therefore raise the specter as to whether they may reduce vaccine efficacy.”
Scientists point to the rapid spread of these variants in their countries of origin and around the world as one line of evidence that they’re more infectious than the original coronavirus strain. In Brazil, the P.1 variant quickly became dominant in the country and surged into nearby nations. In the United Kingdom, the prevalence of B.1.1.7 rapidly overtook other coronavirus variants in multiple parts of the country. It appears to be on track to do the same in Massachusetts as well.
One possible reason these variants are taking off in Massachusetts now is because people are moving around more, said Dr. Nahid Bhadelia, an infectious disease physician at Boston University, in testimony at the hearing. Citing data from Apple, Bhadelia pointed to a steady rise in walking, driving and transit use in Massachusetts since January. That also means that as people engage in more activities that might lead to exposure to the coronavirus, they’re also more likely to get infected.
“Any activities that were being held are potentially likely to lead to more cases,” Bhadelia said.
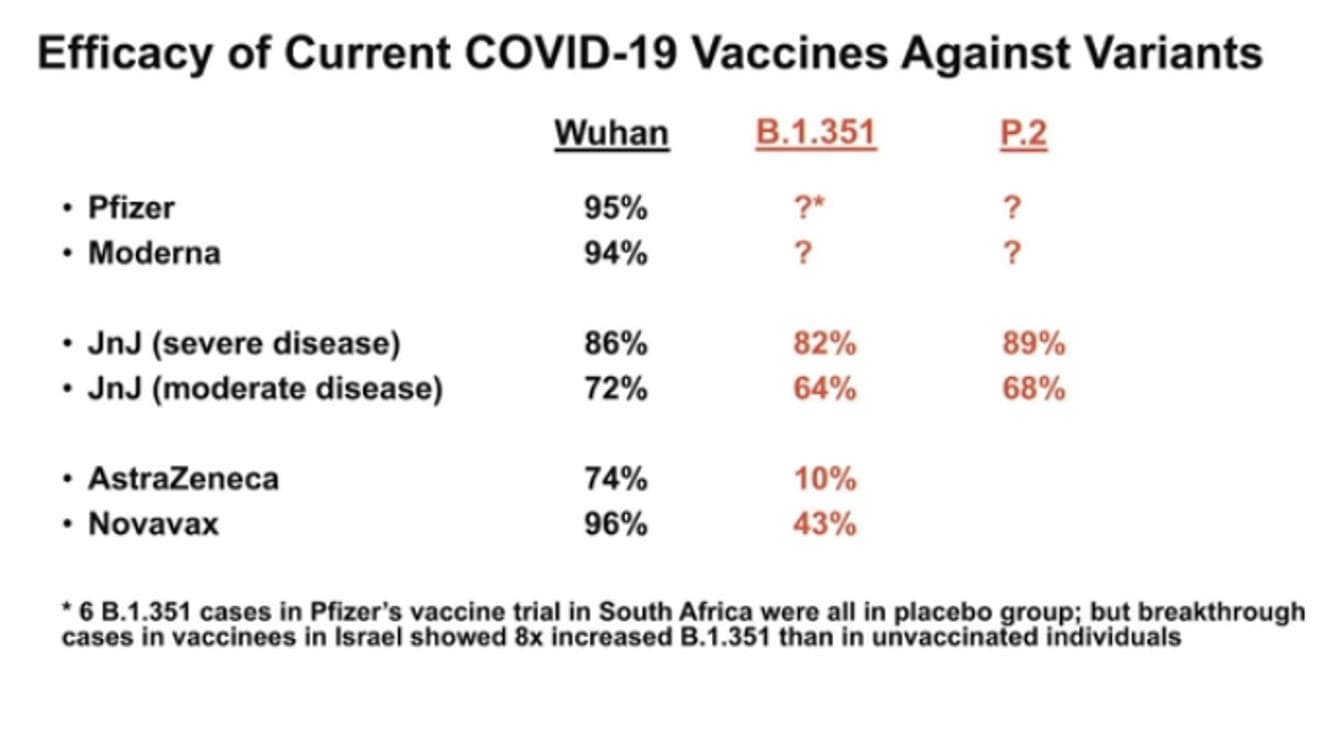
Data from the Johnson & Johnson, AstraZeneca and Novavax vaccine trials suggest that both the B.1.351 variant — which was first found in South Africa — and the P.2 variant may have some ability to resist vaccine immunity, Barouch said. In particular, these vaccines had less efficacy against the B.1.351 variant. However, the latest data suggest this variant appears to be gaining less of a foothold in Massachusetts. And the Johnson & Johnson vaccine still had high efficacy against variants, particularly when it came to preventing severe disease, Barouch said.
“Protection against severe disease was in the mid-80s against all three variants [the wild-type coronavirus, B.1.351 and P.2], which is actually very good news, because it suggests that the vaccine still retains robust protection at least against severe disease against these more worrisome variants,” Barouch said.
Vaccines seem to work well against the B.1.1.7 variant as well, Dr. Paul Biddinger, director of emergency preparedness at Massachusetts General Hospital, pointed out at the hearing. As long as vaccination can move faster than coronavirus variants can evolve to evade vaccine immunity, Biddinger says vaccines should win out, in what is essentially an evolutionary arms race between medical technology and the virus.
“The good news is we are vaccinating while this is happening, trying to win that race, between vaccination and rise in case rates,” he said.
On the other hand, should we fail to quickly vaccinate enough people, that could give rise to even more potentially dangerous or vaccine resistant variants, Broad genomicist MacInnis warned. If the virus continues to be prevalent in a partially vaccinated community, it may mutate in ways that can overcome the obstacle of vaccinated individuals.
“The evolutionary pressures on the virus are changing and will continue to change,” MacInnis told lawmakers. “Most notably through the impact of large-scale vaccination, which will almost certainly drive the emergence of new variants of interest and potentially variants of concern. It's really an arms race between what we can throw at this virus, and its ability to evolve strategies to evade our toolkit.”
The genomic surveillance that her lab does will help find those variants, if and when they emerge, MacInnis said.
“We’re constantly surveying the landscape for variants that are sputtering kind of beneath the surface, that haven’t been identified as formal variants of concern but could be emerging threats,” she said.
No matter what variants emerge, they still cannot overcome basic safety precautions, said Dr. Benjamin Linas, an epidemiologist at Boston University. As long as people continue following measures such as mask-wearing and physical distancing, certain public activities and in-person learning should be able to continue, Linas said.
“These variant viruses do not gain superpowers. They’re the same virus. They’re just a little bit stickier on the receptors, so if a person is exposed, there is a greater probability they become infected,” Linas said. “The mitigation remains the same: masks, distancing, hand-sanitizing and simple ventilation improvements.”
