Support WBUR
Coronavirus Coverage
The Coronavirus May Never Go Away. But This Perpetual Pandemic Could Still Fizzle Out
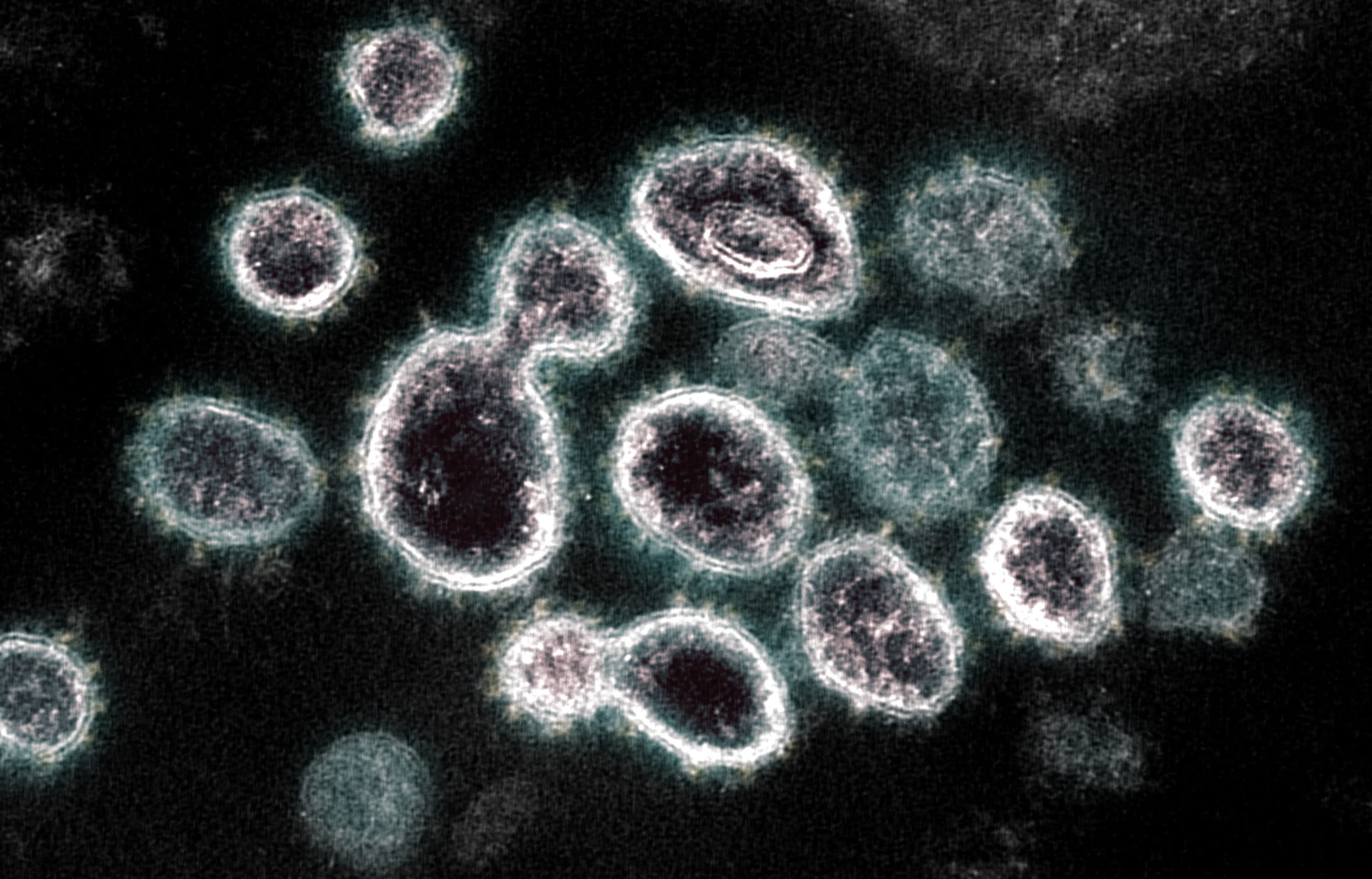
When the novel coronavirus burst into the world, and 2020 was still young and full of hope, many imagined the pandemic would last for just a few weeks of "lockdown." Later it became: Okay, just one more year of this.
Then the vaccines came out, and even health experts were finally starting to talk about population-level immunity, relaxing restrictions and living it up like it was ’19. Cases were dropping, at least in the United States, and it looked like the end times might soon be at an end.
“For the first time, even as we were loosening restrictions, and the Red Sox came back and etc., cases continued to drop. I was like, ‘This is categorically new epidemiology. This is vaccine,’ ” says Dr. Benjamin Linas, an epidemiologist at Boston University. “We had that moment of hope that perhaps we could generate complete herd immunity. I had adjusted to the idea of like, ‘This is awesome.’ ”
Turns out things are not awesome. With the surge of delta variant infections around the world and the revelation that the strain can cause fully vaccinated people to experience infections and transmit the virus, Linas and other health scientists say it’s time to recalibrate our expectations once again. The coronavirus might very well be around forever, and Linas says it’s high time we accept that.
“I don’t think we’re ever going to eradicate or even eliminate SARS-CoV-2 [or the novel coronavirus],” Linas says.
That leaves public health at a crossroads. If COVID-19 cases cannot be eliminated, and the window for herd immunity has passed, then health officials need new goalposts. Linas says that so far, they haven't been well-defined.
"I’m not sure that I can do the winter the way I did last winter. I think it’s actually starting to tear apart the fabric of our society.”
Dr. Benjamin Linas
If the goal is to stop transmission, then everyone should follow 2020-style COVID restrictions, since delta can spread among vaccinated people as well as unvaccinated people. Linas says that may have the benefit of preventing new, even more dangerous variants from arising, but it also comes with costs.
The deprivation of regular social interactions, time with family, travel and other activities has already taken a toll over the last year and then some. Linas says some restrictions — like public indoor mask mandates — are needed for now, but the idea of carrying them on in private is depressing.
“I don’t know how you feel, but I don’t think I can do it again this year. I’m not sure that I can do the winter the way I did last winter,” Linas says. “I think it’s actually starting to tear apart the fabric of our society.”
There is another option, Linas says. Vaccinated people could stop trying so hard to avoid coronavirus exposure at all costs. It’s becoming increasingly clear that even with the delta variant, vaccinated individuals are much less likely to become ill, end up in an intensive care unit or die. According to data from North Carolina public health officials, vaccinated individuals are four times less likely to get COVID-19, and 15 times less likely to die of it.
“We might need to distinguish the difference between COVID-19, the disease, and SARS-CoV-2, the virus," he says. "With the vaccine, it might be possible to eliminate COVID-19 disease even if we can’t stop all the transmission.”
That will take a serious mental adjustment. Linus says accepting more coronavirus risk, even as a fully vaccinated person, still feels like blasphemy. But if the consequences of getting COVID-19 are much less severe for vaccinated people, then it may be time to start getting more comfortable with a little more risk.
This might become easier in a future when the coronavirus is still present, but it’s largely lost its teeth. At some point, every adult will have either gotten a COVID vaccine or survived the disease so that most future infections result in only mild illness, says Dr. Shira Doron, a hospital epidemiologist at Tufts Medical Center. Then, she thinks, COVID will slowly “fade into the background and be one of those viruses that just circulate.”
"People will mostly get mild COVID and won’t think about it too much.”
Dr. Shira Doron
“If you think down the road, and I don’t know how long from now this is, every adult [will] have some immunity to COVID," she says. "People will mostly get mild COVID and won’t think about it too much.”
In rare cases, people will still get severe COVID and end up in the hospital, Doron says, but this was already happening with other viruses such as the common cold.
Here's a possible wrinkle: The pandemic may have changed our attitudes about disease transmission, Doron says. Just because we were fine with the flu, RSV and common colds dancing about each winter, that doesn't mean we should have been.
With the coronavirus in the seasonal mix, Doron says it's possible we're in for a perpetual pandemic, one that resumes each winter — even if the virus ceases to be a fatal risk for most people.
Doron says we’ll reach a new stage in the pandemic when case numbers are no longer coupled with rising hospitalizations and deaths. We’re definitely not at a point where restrictions can go away just yet, Doron says.
The best way to get there is by vaccinating everyone who currently lacks immunity to the coronavirus. In that way, the short-term goal hasn’t changed, says Dr. Sabrina Assoumou, an infectious disease physician at Boston Medical Center.
“Remember, we don’t vaccinate for the common cold,” she says. “The goal is to prevent severe disease, hospitalization and death. And right now, we’re very fortunate that in the U.S. we have vaccines that provide a high level of protection.”
It’s also possible we might never see a future where COVID-19 fades slowly away. Spikes continue to happen and, Doron adds, delta pulled the rug out from under us. If vaccination doesn’t happen quickly enough, it’s still possible a new variant might emerge that causes more disease.
“No one has any idea how to predict what the future looks like in waves of illness,” she says. "So we just don't know."
