Support WBUR
MassHealth expands long-term care to thousands of immigrants
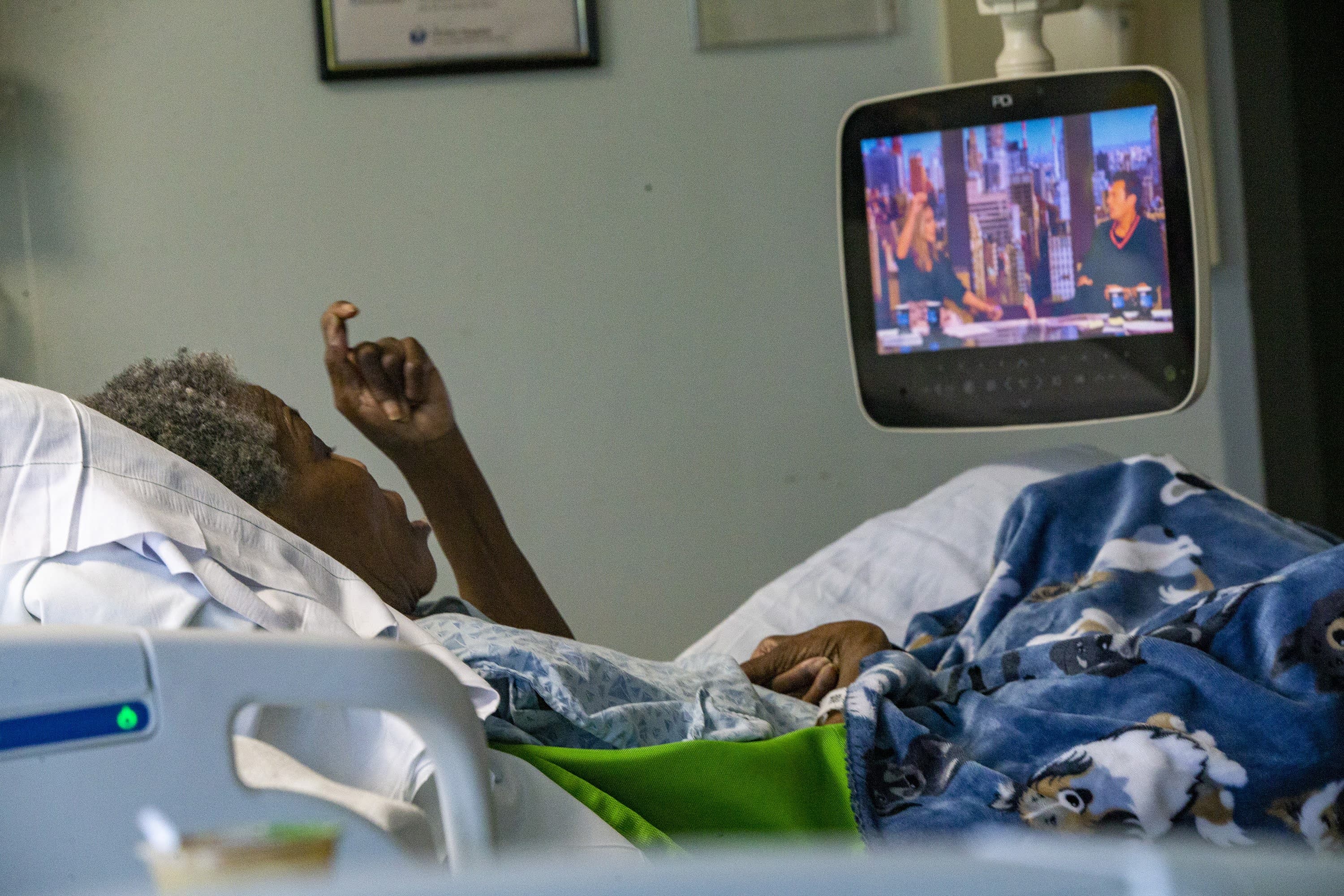
Editor's Note: On Nov. 3, Nora Ketter was released from UMass Memorial's HealthAlliance-Clinton Hospital, where she spent more than three years. She was transferred to a skilled nursing and rehabilitation facility in Leominster, according to attorney Andrew Cohen of Health Law Advocates, who's worked on her case. Due to the recent change in MassHealth policy explained in this story, Ketter became eligible for long-term care coverage on Nov. 1. Four days later, Ketter's immigration attorney, Eloa Celedon, learned Ketter's green card had been issued. That change in her immigration status would have allowed her to qualify for long-term care before the MassHealth policy change.
Traducido en español por El Planeta Media.
Thousands of immigrants will become eligible for long-term care coverage under MassHealth, the state's Medicaid program, thanks to a policy change that takes effect Nov. 1.
The MassHealth members that fall under the new policy are currently prohibited from long-term care coverage due to their immigration status, though their medical care is covered by the program.
One of those immigrants is Nora Ketter, about whom WBUR reported in May. Ketter is a 75-year-old Liberian immigrant who came to the U.S. in 1989. In recent years, she developed dementia. She was admitted to UMass Memorial's Clinton Hospital three-and-a-half years ago and has been stuck there ever since.
Ketter should be in a skilled nursing facility. But she hasn't qualified for that care because she's still awaiting the green card she applied for more than two years ago. Upon getting the green card and the lawful permanent residence it confers, she would have immediately qualified for long-term care due to how long she's been in the U.S. Under the new MassHealth guidelines, she won't have to wait for that change to her immigration status.

Ketter's sister, Georgia Dennis, took care of her until things got too risky due to her dementia. Dennis says she's prayed for a long time that her sister would be able to move to a nursing home.
"It means everything to me that she's going to be in a place where she can get therapy, where she can do exercise or things that she should have been doing," Dennis said. "Because it's not only for my sister that I'm thinking about. It's for all the other people in that same situation as she is in."
Dennis sought help from attorneys to try to improve her sister's situation, including Andrew Cohen of Health Law Advocates in Boston. Cohen, along with colleagues, pushed MassHealth for years to expand coverage for elderly, disabled immigrants who receive medical coverage from the program but not long-term care coverage.
"I am elated," Cohen said, describing the moment last Friday when MassHealth officials announced the new policy in a meeting with advocates.
"I literally became emotionally overwhelmed," Cohen said. "I started to cry for joy because it is such an important policy change when it comes to the lives of people like Ms. Ketter. This really is going to mean so much in terms of allowing her to be able to get care the care that she needs in the right setting."
Cohen and Dennis praised the nurses and doctors at UMass Memorial for caring for Ketter, and hospital administrators for allowing her to stay. But they point out the hospital isn't equipped to give her memory care or other specialized services. Since she entered the hospital, she stopped walking.
UMass Memorial and other hospitals have collectively foot much of the bill for Ketter's long stay. They pay into a fund that covers care for the uninsured — or in her case, under-insured.
The state's Executive Office of Health and Human Services, which oversees MassHealth, did not answer questions about how much the policy change will cost or how the state will pay for it. Approximately 120,000 people are in the plan that the new guidelines will cover — MassHealth Family Assistance — the agency said. About 10,000 of them are immigrants, according to a spokeswoman. They will qualify for six months of care in a skilled nursing facility, rehabilitation hospital or other setting, as needed — up from the current allowance of 100 days. But if they need long-term care beyond six months and meet medical requirements and other criteria, they'll be eligible to enter other MassHealth plans that cover that care.
According to Andrew Cohen, the new policy makes immigrants with disabling conditions — including DACA recipients, people awaiting green cards or immigrants who recently obtained one — equal to U.S. citizens in their ability to access long-term care in Massachusetts. He believes recent dynamics here and around the country added to the pressure on MassHealth.
"I think there was a greater appreciation of disparities due to the COVID-19 pandemic — also because of the broader racial justice awakening," Cohen said. "And I think MassHealth leadership has realized that treating immigrants differently in terms of their access to long-term services and supports was ultimately a huge problem in terms of racial disparities."
Daniel McHale, vice president of healthcare finance and policy for the Massachusetts Health and Hospital Association, issued a statement saying the organization is grateful for the state's "bold action" to expand long-term care coverage for immigrants.
"This important benefit addresses long-standing challenges by ensuring these patients have access to the resources they need to transition from acute hospitals to other settings," the statement reads.
Correction: An earlier version of this post misstated the number of immigrants covered by the plan due to incorrect data from the state.
This article was originally published on October 15, 2021.
This segment aired on October 15, 2021.

