Support WBUR
Coronavirus Coverage
Got COVID? Here's what to know about drug treatments, and who is getting them
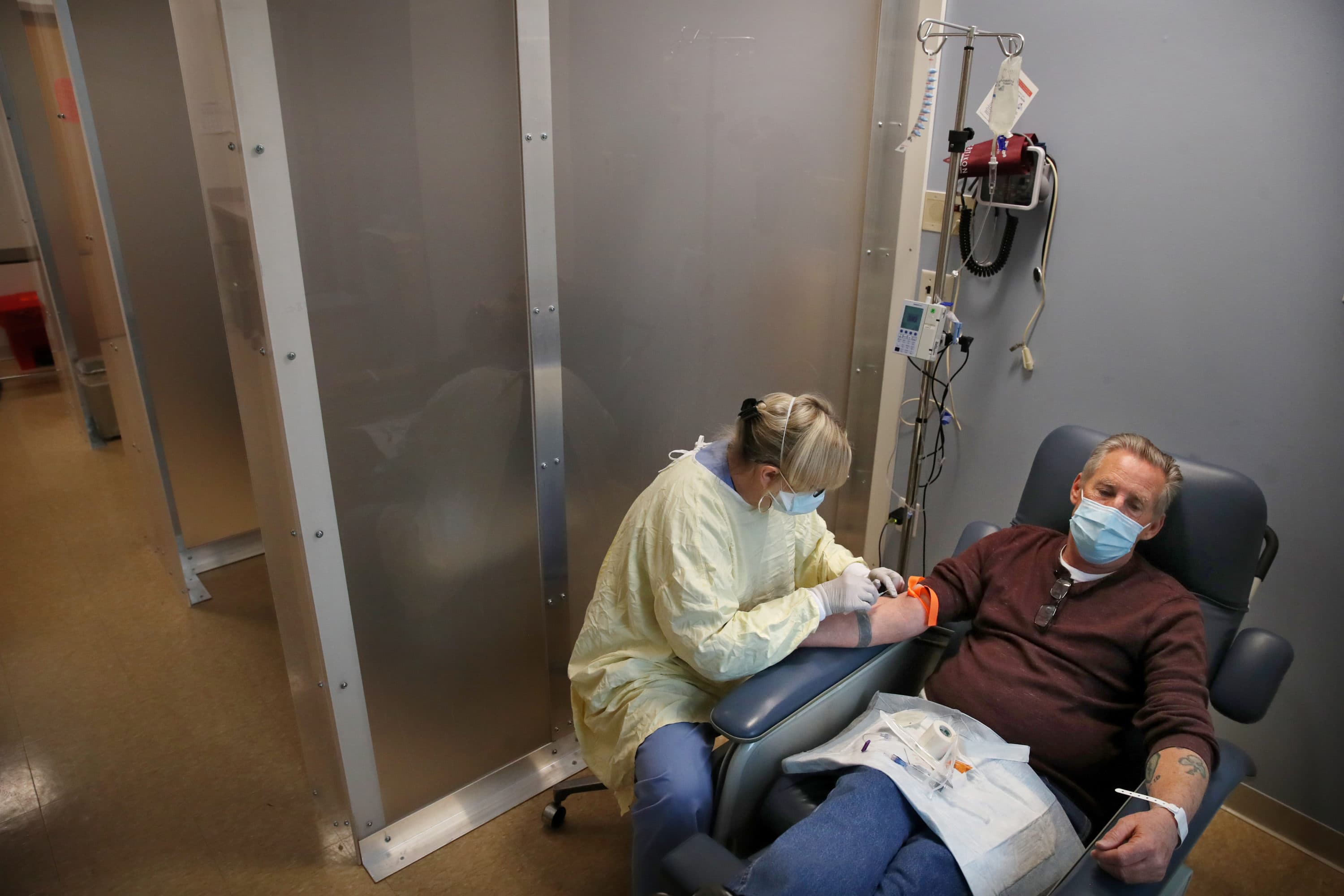
COVID case counts in Massachusetts are trending down, but they are still higher than at any point pre-omicron. That means, there are still a lot of people getting sick with COVID.
Several treatments are available that promise to help keep patients out of the hospital, but they are in short supply. We talked to doctors about the COVID treatment options, who is getting them and when supply will improve:
What Treatments Are There For People Who Get COVID?
In an outpatient context, there are four medications being used to help people with omicron infections.
Two are given intravenously: a monoclonal antibody treatment called sotrovimab and an antiviral drug called remdesivir. They’ve both proven very effective at preventing severe disease. However, there are challenges. There's a limited supply of sotrovimab. Plus, giving the medications through an IV adds logistical complications, especially since there are staffing shortages throughout the health care system.
The other two medications are antiviral drugs given orally. Both of these drugs were authorized just over a month ago and are the first at-home treatments available.
Pfizer's treatment — called paxlovid — is almost 90% effective at preventing hospitalization and death. But it is in very short supply and only recently became available to patients in Massachusetts. Merck’s pill, molnupiravir, is closer to 30% effective and is being seen as a back-up option. Both of these treatments need to be taken soon after the first signs of infection.
Despite the challenges, these treatments are helping, doctors say.
“It's hard to overestimate the impact of these medicines, if given to the highest priority group — the people who are most vulnerable,” said Scott Dryden-Peterson, an infectious disease doctor and the medical director of Mass General Brigham’s COVID outpatient therapy. “If you get three doses out, you prevent approximately one hospitalization.”
That’s critical, he said, given that hospitals are very, very full.
Who Is Getting These Treatments?
Currently, there aren’t enough of these drugs for everyone who is catching the coronavirus. And, to really work, these drugs have to be given to patients quickly, without knowing who will become gravely ill. (Most of the medications must be given within five days of symptom onset. The monoclonal antibody treatment can be given up to 10 days after symptoms start.)
This means doctors have to prioritize the people they believe are most likely to end up in the hospital with severe COVID.
There are federal and state guidelines that help doctors determine who should be eligible. They’re based on four factors: age, vaccination status, immune status and other clinical risk factors.
The population at highest risk — called Tier 1 — includes people who are moderately to severely immunosuppressed, people who are not fully vaccinated and over 75 years old, and people who are not fully vaccinated, over 65 and have another risk factor such as heart failure or lung disease.
Up until very recently, there were insufficient staff and supplies to treat all the patients in Tier 1 in Massachusetts. That meant many hospitals turned to lottery systems to determine who got the limited doses.
Now, things are improving. That's because Pfizer’s antiviral oral medication started getting to patients, and the number of very vulnerable patients has begun declining as overall case counts in the state fall.
Sandeep Jubbal, an infectious disease physician and the medical director of the COVID Treatment Center at UMass Memorial Health, said as of last week his center was able to provide treatment to all Tier 1 patients and people in the next priority group, Tier 2. The staff is even looking at opening up for Tiers 3 and 4.
“This is absolutely good news,” Jubbal said.
What Should I Do If I Have COVID And Think I Might Be Eligible For Treatment?
The reality on the ground can be messy. Some patients are going from doctor to doctor, or emergency department to emergency department, trying to find someone who can get them an authorized treatment.
But that's not how the system is supposed to work. In Massachusetts, as soon as you get a positive test, medical professionals say you should reach out to your primary care doctor or your specialist. Your doctor will help determine if you might be eligible for treatment and check your medical record — for example, people with severe kidney issues should not take paxlovid. Then, if you might qualify, your doctor can get you on the list for a treatment center.
Some states are relying on commercial pharmacies to distribute treatments, but Massachusetts has focused on medical centers and mobile sites. Many of these treatment sites are now accepting at-home rapid test results and not waiting for PCR tests, since it can sometimes take a while for PCR test results to come back.
Jubbal says there is some discussion about creating a system where patients can call up a treatment center themselves and not go through their physician. But, he said, that is not happening soon.
Has There Been Pushback Around Distributing Treatment To Unvaccinated People?
Yes, there has been frustration about this. However, experts say, it’s important to remember that the goal is to keep as many people as possible alive and out of the hospital. This is partly so hospitals are not overwhelmed and can treat patients with COVID as well as non-COVID conditions.
Jubbal said he’s heard this concern a lot. “The rationale is, given the current surge of patients who are unvaccinated, they have the highest risk of being hospitalized. And the patients who are vaccinated, they usually don't get to the point or get sick enough to be admitted to the hospital,” he said.
As UMass’s treatment center begins offering COVID drugs to patients in Tiers 3 and 4, Jubbal said it will prioritize people who are vaccinated but not boosted. That’s because vaccination plus boosting already does a really good job at preventing hospitalization and death.
Is The Limited Supply Being Distributed Fairly?
Unfortunately, there are signs nationally that the available treatment is not necessarily reaching everyone equitably. A recent report from the CDC found that earlier in the pandemic Black, Hispanic and Asian individuals were less likely to receive monoclonal antibody treatments.
When Will Supply Improve?
Although the release of paxlovid and the drop in cases has improved the picture in Massachusetts, Dryden-Peterson expects the supply of COVID therapies will be very tight at least through February.
The hope is that, eventually, treating COVID will be more like treating influenza. If you get the flu and your doctor deems you’re at risk of serious illness, you can go to your local pharmacy and pick up an antiviral medication. But Dryden-Peterson says this reality is still “far in the future.”
This segment aired on January 26, 2022.
