Support WBUR
The omicron surge in Massachusetts has subsided. Now what?
Editor's Note: This is an excerpt from a special coronavirus edition of WBUR's morning newsletter, WBUR Today. You can get regular weekday morning updates about the evolving pandemic and all other essential Boston-area news by signing up for WBUR Today.
We restarted these coronavirus special newsletters a few weeks ago because we were back in the soup, with cases rising at an uncontrolled rate.
A little more than a month later, that wave hasn't just crested, it's ebbed considerably. You can see it in the 14-day per capita case numbers:
And you can see it in the MWRA wastewater data, which has proven itself to be one of the most reliable barometers of the pandemic. The poop data shows COVID-19 levels peaked on Jan. 3. A day later, cases reported by date peaked. About two weeks later, hospitalizations crested on Jan. 14. Four days after that, so did deaths. We are definitely on the back end of this wave.
And just like the end of last year's surge, people are talking about the future. But this time, it isn't just dreams about hot vax summer. This time, the conversation is a little more serious, and to some, a little more scary.
People are now talking about COVID as endemic, aka as something we're gonna have to live with, even as it remains a dangerous illness.
The concept came up this week, when Gov. Charlie Baker rolled back the state's masking advisory.
You've also heard the word from Dr. Anthony Fauci, who lamented that we will not eradicate COVID the way we did with smallpox, but instead we'll see the disease transition to one we manage.
“Hopefully it will be at such a low level that it doesn't disrupt our normal social, economic and other interactions," he said.
This time, the conversation is a little more serious, and to some, a little more scary.
So, why all this talk about endemic now? We've come through other significant surges in Massachusetts and other parts of the country. What, aside from an understandable frustration with the pandemic, has so many people talking about reframing COVID as an endemic illness? To be sure, there are people who just want to turn the page, everything else be damned. But lots of smart people — people you have gone to for thoughtful, consensus takes on where things stand — are also talking about the COVID-19 pandemic becoming an endemic. Here's why:
- Vaccines
- Therapeutics
- At-home and PCR testing
- The observed difference in outcomes in cases because of the above
- Declines in hospitalizations
Given that lens, Massachusetts is in a very strong place to try this transition, which, to be clear, does not mean giving up on trying to reduce the risk of COVID. But the commonwealth (and the Northeast in general) has one of the highest vaccination rates in the world. On top of that, more than half of the fully vaccinated people in the state have received a booster shot. The result, despite lots of press about breakthrough cases, has been very positive, as this chart shows:
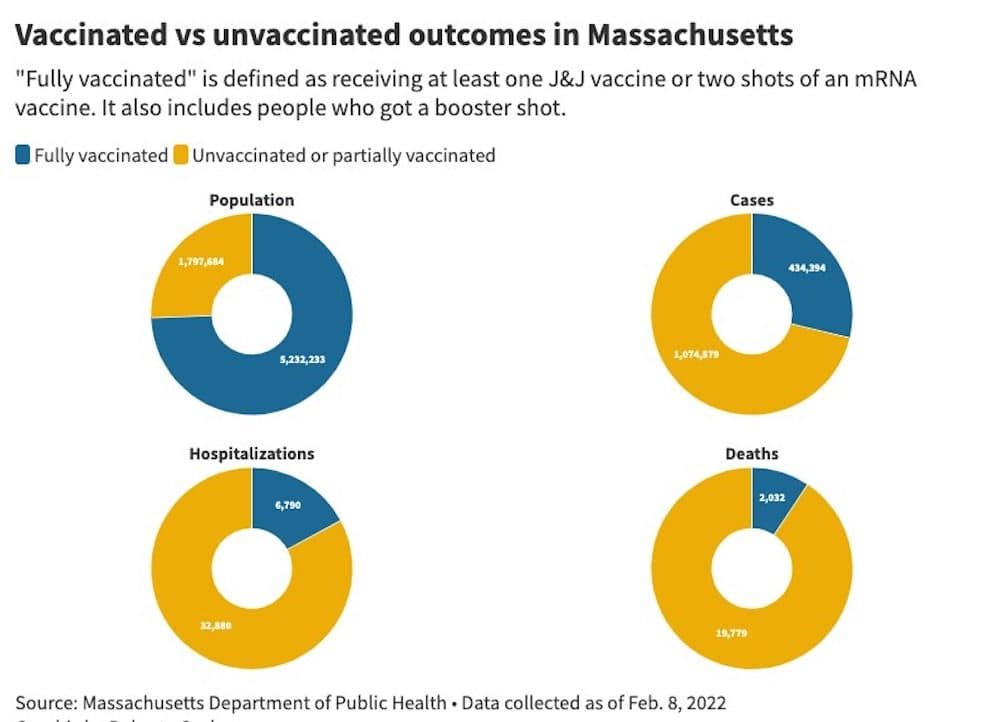
You can click here to see a bigger version of the chart. Here's the underlying data, provided by the state.
The data is clear: the COVID vaccines, delivered years faster than any previous vaccine, have worked very well, especially in curbing the severity of illness.
Doctors and nurses have a better understanding of COVID-19 and have new therapeutics added to their arsenals. And researchers are providing more insights seemingly every day.
And it took too long, maybe, but we're approaching a point where there's much better access to free at-home testing kits and continued PCR tests for when more accurate detection is required.
In short:
- We're better prepared to prevent the illness.
- We're better prepared to detect the illness.
- We're better prepared to treat the illness.
As the Washington Post writes, "None of these tools are silver bullets. They can’t eliminate the coronavirus. But together, they can help turn the virus into a manageable risk, allowing people to hug relatives, go to the movies and travel without fear."
(That Post piece goes into great detail about all of the facets above, and is laid out in a very engaging way. It's definitely worth a bookmark.)
There's another reason for scaling back on all the precautions we've been taking, and this is one many people may have a hard time accepting: The fatigue is real, and if left unrecognized, will make it harder to get people to gear back up during another surge. As Dr. Ashish Jha wrote recently on Twitter, "preserving people's willingness to do things is critical."
Despite all of this, there are still people who are especially susceptible to severe illness from COVID, and there are people suffering long-term effects from the bug. Many of us have lost friends and loved ones to this pandemic. Endemic doesn't mean COVID is no longer dangerous. As Jacob Stern and Katherine J. Wu write in The Atlantic, we have plenty of very virulent endemic diseases, like measles and whooping cough.
Efforts to protect the immunocompromised, to redouble vaccination efforts among older people, and to better research and treat long COVID are a critical part of addressing endemic illness. (WBUR's Gabrielle Emanuel gets into this subject more in this separate excerpt of our newsletter.)
It also means staying frosty; our civic leaders must be ready to respond during any future surges. Being prepared could include setting clear metrics that would trigger specific actions, like a return to masks for short periods. Axios explores that idea more fully here. And CDC Director Rachelle Wallensky on Wednesday said hospital capacity will remain a key metric moving forward, since the ability to quickly treat the ill is a hallmark of properly managing a disease.
None of this is to say we're going "back to normal," if by "normal" you mean a pre-COVID world. But, if you mean you can now go and live your life, grabbing a mask when you feel sick or if you’re not vaccinated, skipping a party when cases rise, and taking tests to make sure you're good to see nana, then yeah, "normal" may be coming back.
