Support WBUR
AI can detect breast cancer risk before humans. Why it may take hospitals a while to adopt the tech

When 68-year-old retiree Ellen Costello received an email asking if she wanted to participate in a medical study about artificial intelligence and breast cancer, she hesitated at first. Did she really want to involve AI in her health?
The AI had already determined Costello was at high risk of developing breast cancer. After thinking it over, she decided to give it a try.
Testing revealed a growth. And surgery confirmed it was precancerous. Now, doctors are watching Costello closely.
All because an algorithm noticed something about her health that humans had missed.
“I’m so glad it led to this,” said Costello, who lives in Rutland. “I’m glad I have the information.”
She is among the first wave of patients in Massachusetts to make medical decisions from this kind of AI risk detection tool. It works by analyzing mammogram images. The goal is to predict cancer before it happens, or find cancer before it spreads, so patients can live longer, healthier lives.
How soon this technology becomes widely available depends on a variety of factors including research studies, medical treatment guidelines, health insurance rules and rollout costs. But gradually, more people are gaining access to this machine learning-powered warning system.
“It’s really hard to know that there are a lot of women that are at high risk of developing breast cancer — but are walking around not knowing that they’re at risk,” said Dr. Leslie Lamb, a breast imaging radiologist at Massachusetts General Hospital who studies AI. “If we could just intervene earlier, it’d be life-changing.”
The AI that flagged Costello as high-risk identifies subtle details in breast x-rays that are undetectable to the human eye and could lead to cancer.
The algorithm calculates a probability — the likelihood that a person will develop cancer in the next five years. Doctors can use this information to guide their recommendations for tests and treatments.
The technology came from a lab at the Massachusetts Institute of Technology run by Regina Barzilay, a professor of electrical engineering and computer science. She describes it as a high-tech weather forecast for breast health.
“We really need to have tools that can help, rather than just staring at an image and trying to guess,” she said.
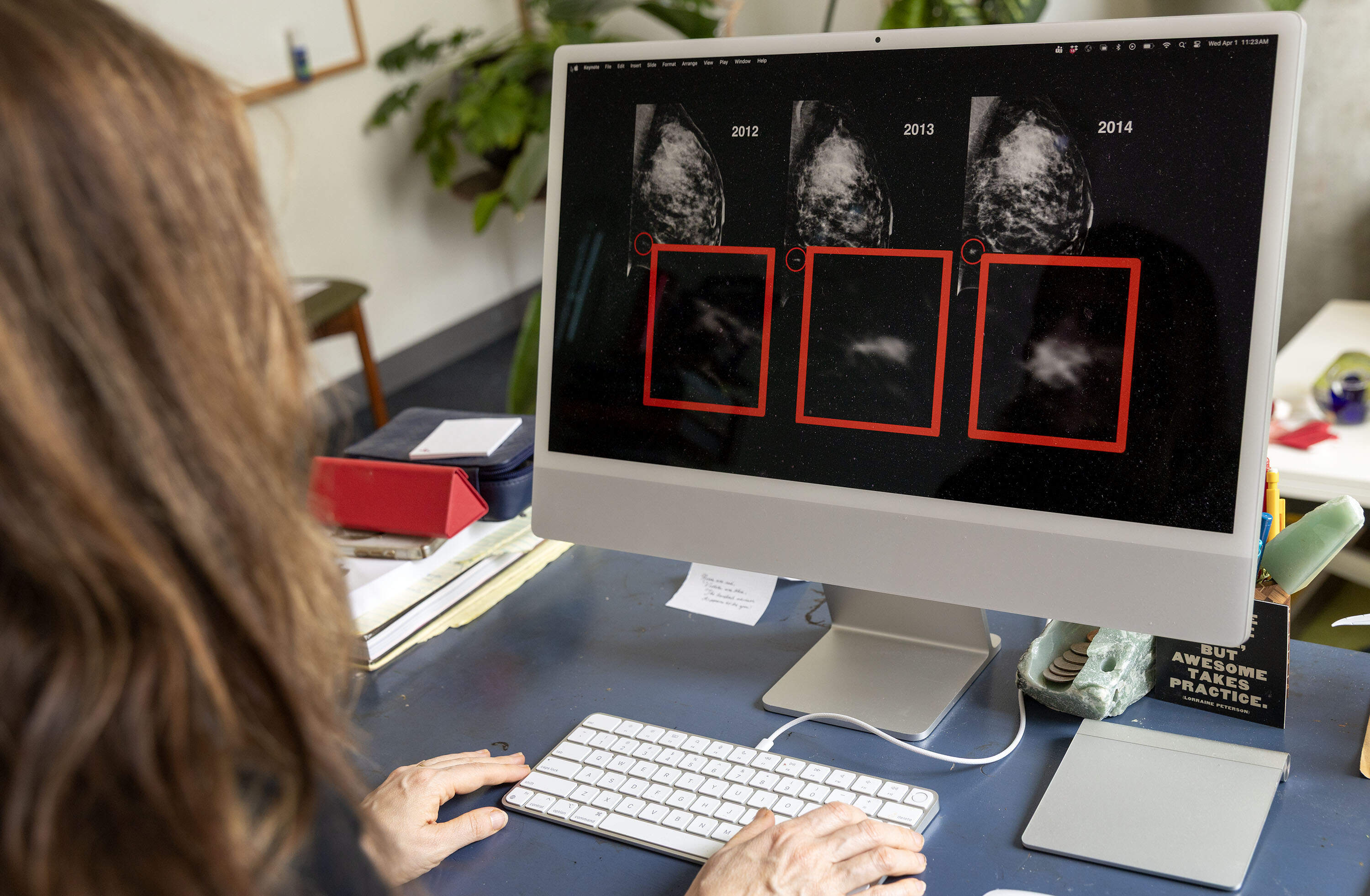
Doctors generally predict a patient’s cancer risk based on factors such as genetics, family history and breast density. But these are far from perfect, and many cancers occur in people without any known risk factors.
“Those of us who don't have a genetic mutation and who don't have breast cancer in our families — we think that we are safe, but some of us are not,” Barzilay said.
Her work is driven by her personal experience. Twelve years ago, as a 43-year-old mother of a young child, Barzilay was diagnosed with breast cancer.
"... that's how I got into this field. I didn't have any credentials that would make me uniquely qualified — besides despair. And it enabled me to push myself through."
Regina Barzilay
As she went through treatment, worrying about her future and her family, she said she was angry. She wondered: Why was there no technology to predict cancer in patients without known risk factors — patients like her?
“I really felt I had to do something,” Barzilay recalled. “And that's how I got into this field. I didn't have any credentials that would make me uniquely qualified — besides despair. And it enabled me to push myself through.”
In 2018, Barzilay and her team launched a breast cancer prediction model trained on data from Mass General. They called it Mirai, the Japanese word for “future.” They and their collaborators around the world have since tested the algorithm on more than 2 million mammograms.
The research has been building. A 2023 study of past mammograms at Mass General found that doctors were able to detect three times as many cancers among women identified as high risk by the AI, compared with women flagged by older methods of calculating risk.
Other studies show the model works across women of different races and ethnicities.

Right now the tool remains mainly in a research phase. It’s been used in over 100 hospitals from North America to Asia that are helping test its accuracy, but it is not a routine part of American healthcare.
“As a computer scientist, my first priority was always to think we need to make the algorithm better, and we are making the algorithm better,” Barzilay said. “But I realize a much harder task is actually to take this technology and bring it to clinic.”
There are several challenges. For hospitals, new AI programs can be expensive and technically difficult to implement.
Health insurance companies don’t routinely pay for newer technologies until they’ve been cemented into national guidelines set by medical groups. In a statement to WBUR, the health insurance trade group AHIP said insurers decide to cover new tests if there is evidence of “substantial” benefit.
At the University of Massachusetts Chan Medical School, researchers built a makeshift data center — a tower of humming servers — to power their work on breast cancer prediction.
They tested Barzilay’s Mirai technology on 65,000 patients who get regular mammograms at UMass Memorial Health. The AI found that 4,000 were at high risk for developing cancer, even though doctors hadn’t noticed any suspicious signs in their mammograms.
"There are a lot of hurdles. That's part of the reason why all these AI things are only being done in rich hospitals ..."
Dr. Gopal Vijayaraghavan
Ultimately, 145 high-risk patients took part in a study, the first in the country using Mirai to predict patients’ future risk, instead of looking at older data. Each participant received a breast MRI, a test that is more precise and about four times more expensive than a mammogram. The MRIs revealed that half a dozen patients already had cancer.
“It was like, ‘Oh my god, we have to use this tool more often,’ ” said Mohammed Salman Shazeeb, an associate professor of radiology at UMass Chan who co-led the study.

The other lead researcher, Dr. Gopal Vijayaraghavan, said the AI tool appears to be useful, but bringing it to more patients will be costly. One reason is that insurance companies are unlikely to pay for a patient’s MRI based solely on an AI projection. The average breast MRI in Massachusetts costs $1,400, according to state data compiled at WBUR’s request.
“There are a lot of hurdles,” said Vijayaraghavan, a professor of radiology and breast imaging specialist. “That's part of the reason why all these AI things are only being done in rich hospitals … who are willing to eat a bit of the cost.
“It's certainly not out in the public for the benefit of all.”
Costello, the patient from the UMass study, said she’s grateful that AI helped her gain some control over her health. After a year of weighing the potential benefits and side effects, she decided to begin a hormone therapy called tamoxifen, which can be taken to prevent cancer.
And she’s getting screened for cancer every six months, instead of once a year.

“I'm always the type of person who wants to just deal with it — deal with it, whatever it is,” Costello said.
All those extra tests make her a little anxious. But Costello said she wants to stay healthy, for as long as possible, for her two daughters and four young grandchildren.
“I did this for my family,” she said. “Because I feel breast cancer is so treatable, and early detection is the best way to treat it.”
Earlier this year, Beth Israel Deaconess Medical Center began offering a breast cancer prediction AI tool to its patients from a company called Clairity. It’s FDA-authorized, but insurance plans don’t cover it. So patients have to pay about $200 for the test.
“There’s equity issues there,” said Dr. Elizabeth Mittendorf, the hospital’s chief of breast surgery. “We don't want a sophisticated test only to be available to our patients who have the financial means to pay for it.”
As the test becomes more affordable, she hopes to expand it to at least 10,000 patients a year.
There are signs of change already. One prominent association, the National Comprehensive Cancer Network, updated its cancer screening guidelines this year to include AI tools.
Mittendorf said she envisions a future in which AI can personalize cancer prevention for everyone. Those at high risk could take steps to detect illness early, or avoid it altogether. And those at low risk could get screened less often — every two years, perhaps, instead of annually.
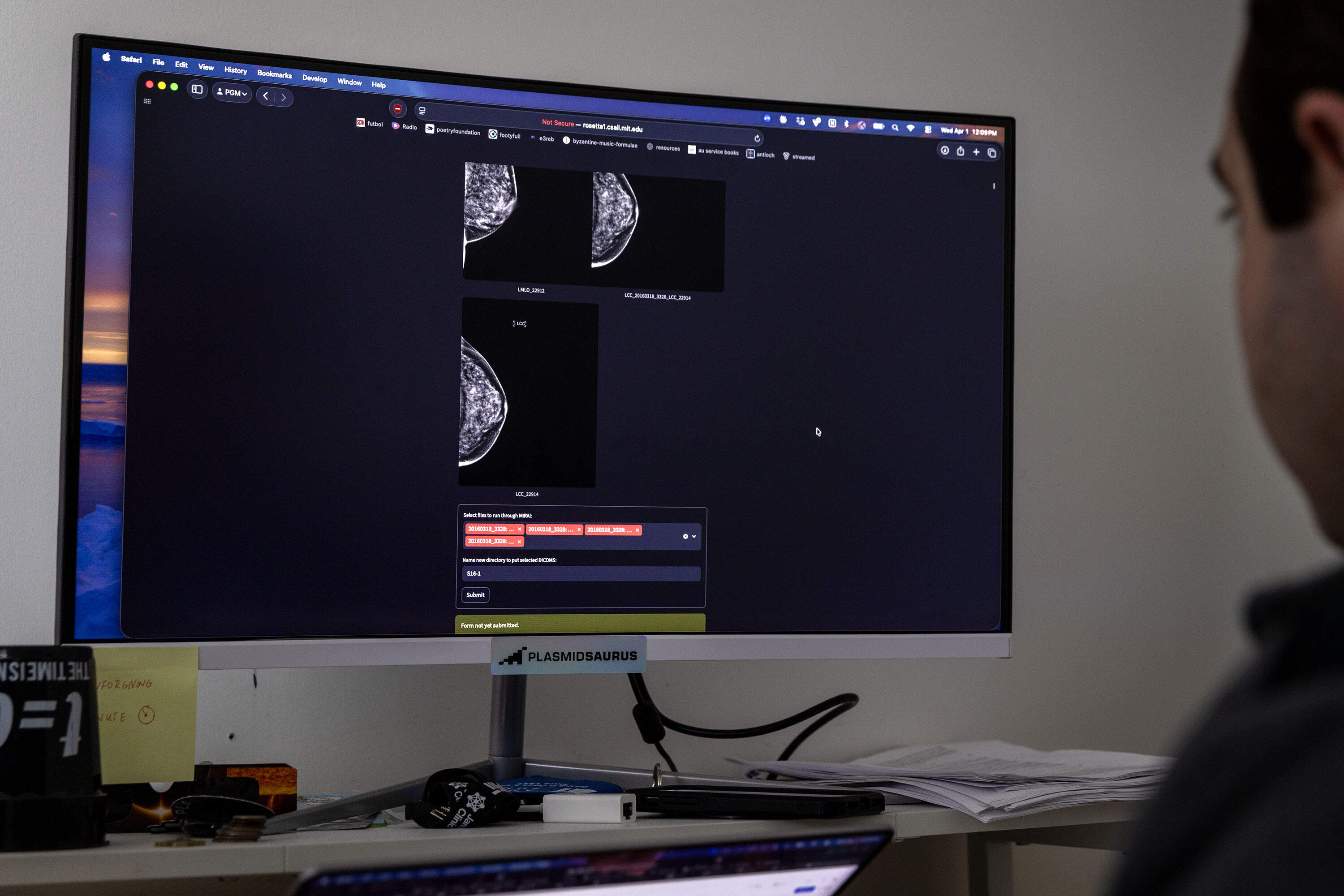
A mammogram is like a thumbprint: “everyone is unique,” said Dr. Connie Lehman, a Boston-based breast imaging specialist and founder of Clairity. “No two women have the same mammogram.”
AI can extract data from the mammogram to give patients information tailored to their individual lives, said Lehman, who previously worked with Barzilay on the development of the Mirai tool.
“ We're going to be changing the face of breast cancer,” she said. “We're going to be finding all of those women in my practice that used to say, ‘That's impossible that my biopsy came back as cancer. No one in my family's ever had cancer. How can it be?’ ”
Lehman said she heard those words often and wondered how she could offer help to patients sooner.
“And we haven't been able to,” she said, “ until now.”
This series is funded in part by a grant from the NIHCM Foundation.
This segment aired on May 5, 2026.
