Support WBUR
Commentary
'I Can't Accept Not Knowing The Answers': Why I Call My COVID-19 Patients At Home
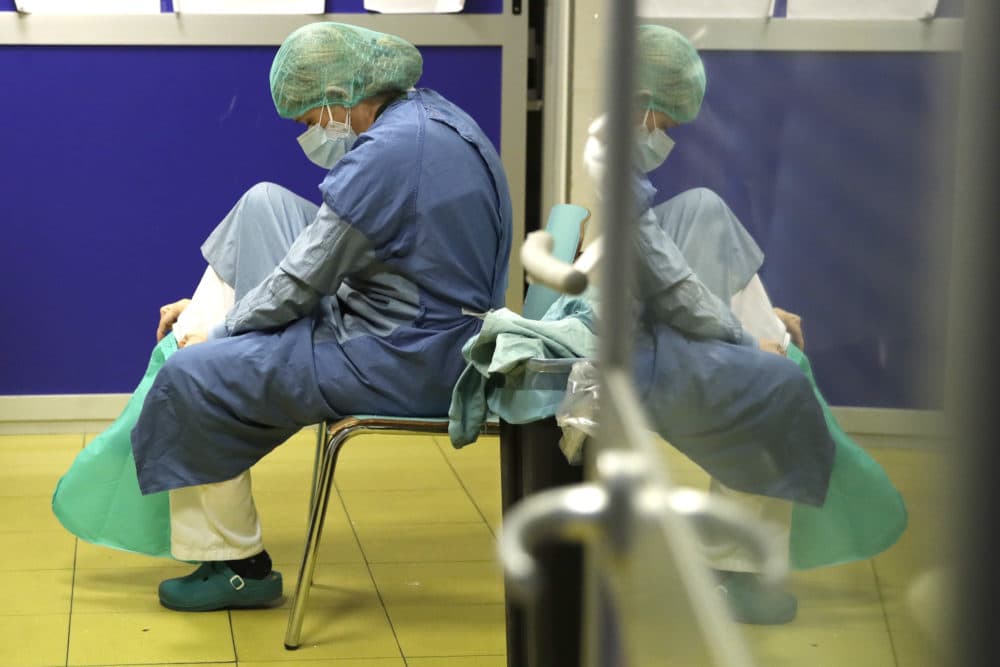
As an emergency room doctor, I have resigned myself that my field of medicine means I usually get to see my patients just once. My role is to stabilize, to triage, and, ultimately, to send my patients to the place I feel that they are safest. Sometimes, that means keeping my patients overnight in the hospital.
More often, that means sending my patients home. I go through a careful checklist of needs in my mind before I make that decision. Is home safe for my patient or is she in physical danger, as are my patients who experience domestic violence? Will my patient be able to eat and drink sustainably or do I think he will need IV fluids? Will he be able to control his pain? Do I think that her illness will get better or worse?
This last question is perhaps the hardest question to answer. It requires us, as physicians, to look into a crystal ball and try to read the future. We are not completely blind in doing this. We rely on the lenses of our medical knowledge and our understanding of the patient’s disease process, our cumulative wisdom and our individual clinical intuition — what we call our “clinical gestalt.”
[We] proposed to do the unthinkable in our field of emergency medicine: Call our patients and see how they are doing.
But coronavirus has made it infinitely more difficult to see clearly into the future. Our lenses are so foggy because our medical knowledge about this illness is so limited. All of us — newly minted doctors and those in our fourth decade of practice — are seeing these cases for the first time. There is a new variable we can’t ignore: scarce hospital resources. We know from watching colleagues in China and Italy that we'll have many more patients than hospital beds. Our hospitals may soon have no vacancies.
When I send a patient home whom I normally would feel confident will be fine — young, only a mild fever and cough, able to take care of all her physical needs — I worry. I am stuck on this question: Will she get better or worse? New questions pop into my mind. What will happen to the other people at home with these patients? Am I sure that they will have access to food while our society is shut down? What about my patients who can’t afford to stock up on two weeks' worth of food because they live paycheck-to-paycheck? Do they have the means to avoid work and public transportation so that others won't get sick?
Even though I am an emergency doctor, a see-you-one-time type of doctor, I can’t accept not knowing the answers to these questions. Not when my patients’ lives, their family members’ lives and my city’s public health are all at stake. So my colleagues and I proposed to do the unthinkable in our field of emergency medicine: Call our patients and see how they are doing.
We developed a system to periodically phone patients who came into the emergency department with COVID. By reaching out to patients at home through telephone or video-enabled virtual visits, we could monitor our patients whose symptoms got worse and instruct them to come back to the hospital if necessary. We could also reinforce self-isolation and infection control, and check on family members who became exposed, developed symptoms and/or need evaluation. We move beyond the step of simply acknowledging that challenges exist to self-isolation for our patients, particularly those who are socioeconomically disenfranchised, and do everything in our power to screen patients for unmet basic needs — food, housing, transportation — and facilitate referral to resources.
Some patients have told us that they receive comfort from hearing the voice of a health care worker and knowing that they are not forgotten at home.
A few of my colleagues have asked patients to come back to the emergency room for a re-evaluation. When patients receive our follow-up calls, many of them express sincere appreciation. Some patients have told us that they receive comfort from hearing the voice of a health care worker and knowing that they are not forgotten at home.
I am lucky enough to practice in a hospital system that is progressive and committed enough to accept seemingly radical ideas that should be common sense. My hospital is poised to try this strategy in our emergency departments and we are furiously, urgently working to establish an infrastructure to make this work as soon as possible. But our system should not be novel. Although it is hard work and those of us in our healthcare systems may already feel like we're operating at full capacity, we cannot ignore the dreaded sense that our patients at home may need us. It is our duty to be sure, even in times of crisis.
