Support WBUR
New Discovery Raises Hope For Universal Cancer Treatment
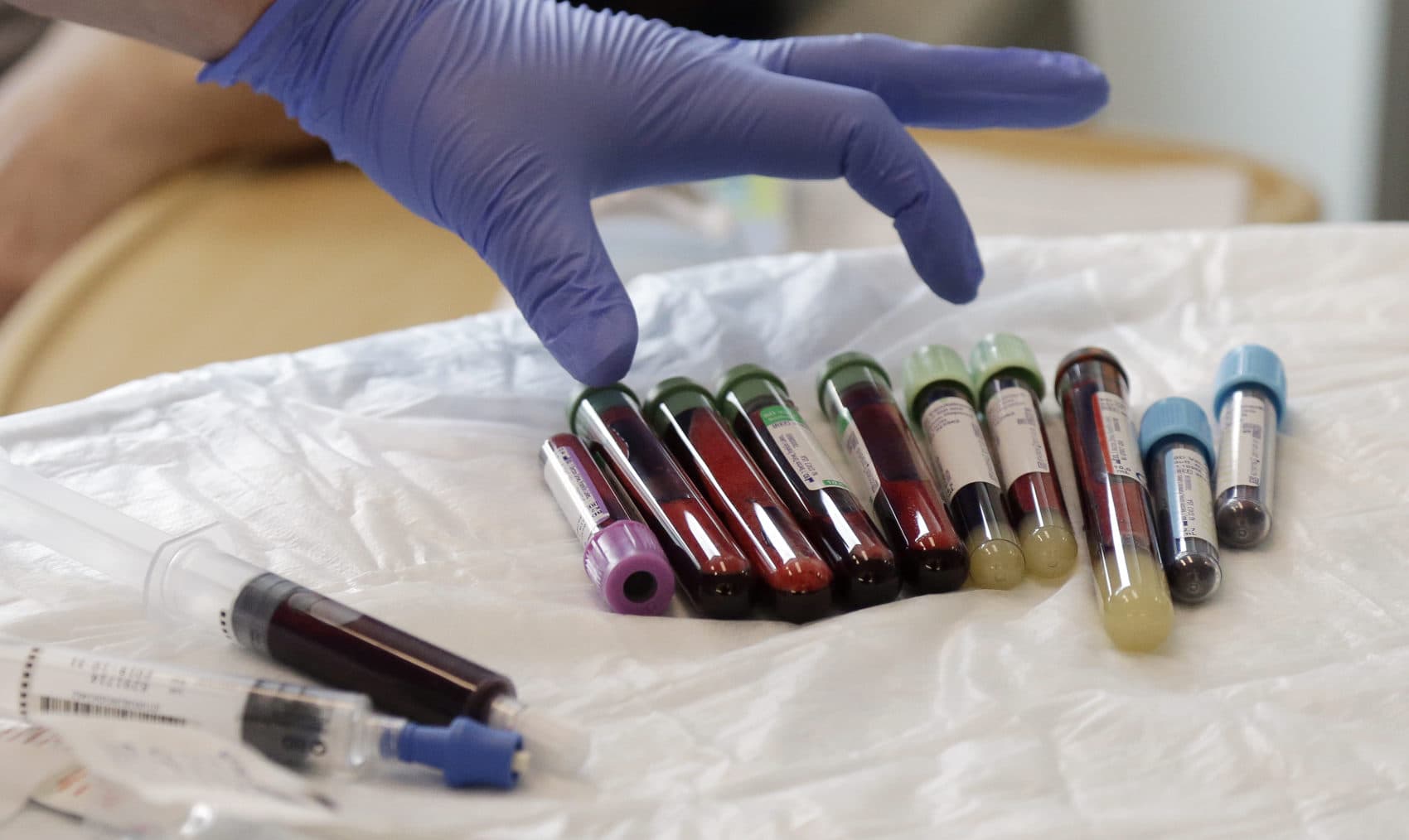
Scientists are still a long way off from finding a cure for cancer, but researchers in the United Kingdom have recently made a significant step toward the creation of a universal treatment for cancer.
Researchers at Cardiff University’s School of Medicine in Wales say they discovered a new method for killing a wide range of cancers, including prostate, breast, lung and others.
The process utilizes T-cell receptors within the immune system, says researcher Michael Crowther. The body’s immune system naturally attacks cancerous cells, but what scientists found is one T cell inside the blood that attacks a variety of cancers.
“Cancer is basically a collection of diseases. So it's not one disease. It's all different types,” Crowther says. “And this immune cell that I found ... that didn't seem to matter.”
The method has not been tested in humans, but Crowther says he is “excited” about what it could mean for the future of cancer treatment.
Interview Highlights
On how the method works
“When I first started the project, the goal was to try and find, as you say, T cells that could react to multiple different bacteria. We do know that these already exist. We were just trying to find new versions of these that would recognize bacteria in multiple different people. And while I was doing that, I basically had these cancer cells that we used to activate the T cells, but what we normally do is load bacteria onto these cancer cells. It's actually the bacteria and products that then activate the T cells usually. But I also had in my experimental setup a cancer cell line that didn't have any bacteria just as like a control, so we can work out if it is actually the bacteria that are activating these immune cells. What I found was actually it was the ones that didn't have any bacteria that were activating some immune cells the best. So what I did next was I screened against a couple of different cancers. Then it recognized all the cancers that we tested against in the beginning.”
On the results when tested on mice
“With the mouse model, what we did is we take a cancer cell and then it's actually a human cancer cell line. We put that into the mouse and then we let that attach itself inside the mouse. When that has happened, we can then put the immune cells into the mouse. And what that did is basically it cleared away the cancer from the mouse. It extended the survival of these mice by weeks. Weeks is actually a very long time.”
On how this practice could work on cancer patients
“Well, it's very early to talk about actually taking it to patients yet, but because with patients who are very sick, we can actually, hopefully get an advanced timeline on taking these immune cells into patients. And it will probably work similar to CAR T cells, which is basically when you take a patient's own immune cells and then you put in the receptor from these T cells. You can then put those immune cells back into a patient and then hopefully clear their own cancer. So that's how it's normally done. Hopefully we will just be able to have a bank of immune cells, and then we can just directly just give that to the patients without having to expand their own immune cells. And we can basically shorten the timeline for treating these patients.”
On why it has taken so long to discover a universal cancer treatment
“When you're looking at the T cells, they usually recognize a subset of proteins called HLA. And the trouble with HLA is it's actually everyone has a different set of HLA. So when their immune cells are given to another person, they don't react to these cancer cells because they will have a different HLA. And this HLA is extremely important for the T cells in order to recognize whatever they recognize on the cancer. So that's why finding these universal targets, especially for T cells, has been so difficult. So that's what's exciting about this research, is that this MR1 protein is the same, so then that means that we don't have this HLA problem.”
On what’s next for this research
“So first, what we want to do is ensure that it's actually safe. We've already shown an example of one in the study that we published. But we want to actually take more immune cells from patients and then put in this new receptor, and then make sure that it's still safe in the lab with their own healthy cells and their own cancer cells and make sure it kills only the cancer cells. Another arm of the research that we want to find is specifically what it is about these cancers that is enabling them to be recognized by this immune cell. So that'll be quite important just to make sure that there's no other side effects. Once we know exactly what that molecule and that process that leads to this immune activation, that is really what we need to find out.”
Marcelle Hutchins produced and edited this interview for broadcast with Kathleen McKenna. Samantha Raphelson adapted it for the web.
This segment aired on February 6, 2020.
