Support WBUR
New Study Finds Formerly Redlined Neighborhoods Are More At Risk For COVID-19
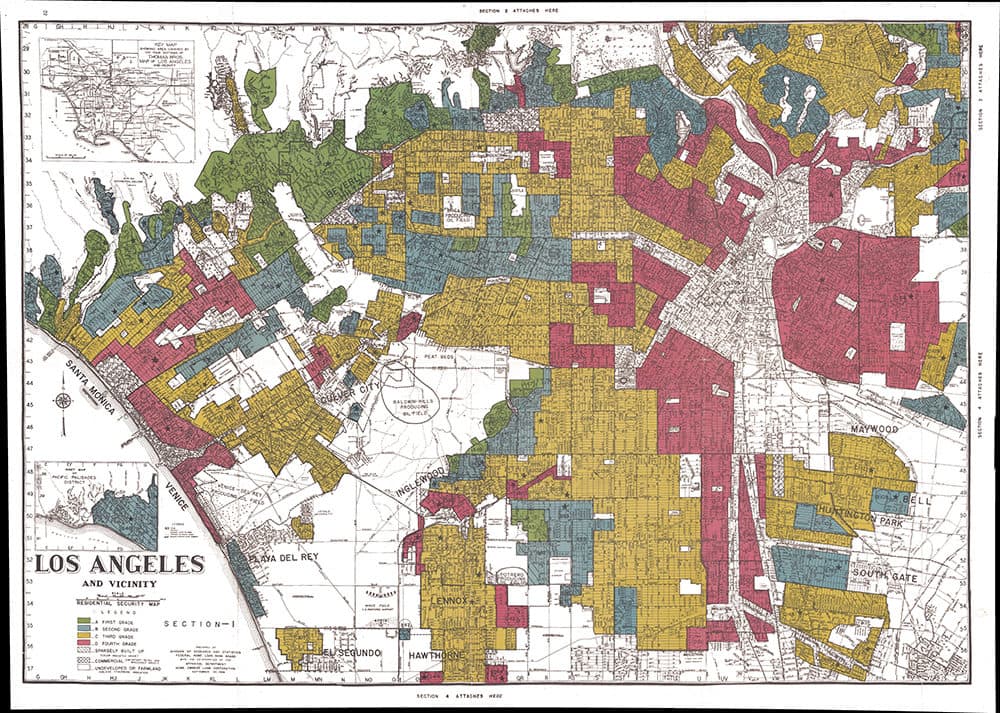
People living in formerly redlined neighborhoods are more susceptible to having COVID-19 complications, according to a new study by the National Community Reinvestment Coalition.
In collaboration with researchers from the University of Wisconsin–Milwaukee and the University of Richmond, the NCRC study found neighborhoods where discriminatory lending practices once limited access to credit for Black, immigrant and poor Americans have higher rates of COVID-19 comorbidities, such as asthma, chronic obstructive pulmonary disease, diabetes and obesity.
“This is no longer an abstract discussion or theoretical discussion,” says Jason Richardson, NCRC’s director of research and evaluation and one of the report’s co-authors. “Redlined areas mean that people die a lot more frequently from COVID-19.”
The practice of redlining was codified by a series of maps created as part of the New Deal by the Home Owners’ Loan Corporation, which evaluated the mortgage lending risk of neighborhoods.
From the 1930s until the passage of the Fair Housing Act in 1968 banned redlining, neighborhoods that were predominantly Black, immigrant or poor were deemed “hazardous” to lend to compared to white neighborhoods.
“The policies of almost a century ago have had an unintended consequence … of locking in place this pattern of segregation,” Richardson says.
Today, areas that were historically rated “hazardous” continue to be segregated with larger Black and Latino populations, higher rates of poverty, lower life expectancy and worse health outcomes, according to the NCRC report.
The study concludes that these health disparities cannot be fully explained by individual lifestyle choices and are instead a result of few healthy options and resources due to years of structural disinvestment.
“When your choices are a McDonald's or the local convenience store for your groceries, you're not going to be eating a healthy diet,” says Richarson. “Obesity is going to be more of an issue for you and that’s part of the story here.”
Multiple studies have shown that obesity increases risk of death from COVID-19. The NCRC study found that one in three people living in historically redlined areas is obese, compared to lower obesity rates in neighborhoods that were not redlined.
“It is no surprise that the COVID-19 pandemic has made existing racial health inequities devastatingly clear,” Helen Meier, Ph.D and assistant professor of epidemiology at the University of Wisconsin, Milwaukee and co-author of the report, said in a press release. “Disparities in COVID-19 infection and illness severity are a result of widespread social and economic inequities produced by structural racism.”
Nationwide, the pandemic continues to disproportionately sicken and kill people of color. According to data from American Public Media’s Research Lab’s ongoing Color of Coronavirus project, Black Americans are dying from COVID-19 at rates 3.6 times higher than white Americans. Compared to white Americans, the mortality rate is 3.2 times higher for Latinos and 3.4 times higher for Indigenous people, the data shows.
The authors of the NCRC study claim this nationwide analysis is the first of its kind to drill down to the neighborhood level to look at how historic redlining impacts the transmission of COVID-19, but they don’t think it will be the last.
Richardson expects to see a lot more research around affordable housing and ongoing segregation as the pandemic continues.
“My hope is that a report like ours or the others that I'm sure are going to be coming out are going to help communities think about affordable housing as a health issue,” he says. “They should be concentrating on providing affordable housing throughout the community, so they are not concentrating their severe health issues among minority and low-income families.”
