Support WBUR
Coronavirus Coverage
Health Care Workers Turn To Military Techniques To Deal With Trauma

It was early in the pandemic last year when Dr. Joshua Morganstein started receiving calls from military veterans who were staffing hospitals. They were calling to tell him how part of their combat training was helpful in dealing with the stress of fighting COVID-19.
Morganstein, the assistant director at the Center for the Study of Traumatic Stress in Maryland, said likening COVID to fighting a war is true in a lot of ways.
"You're going into a situation that is extremely stressful, that is likely to go on for an extended period of time and is going to involve situations that are dangerous," he told WBUR.
But there are differences. Health care workers had to fight a battle there was no training for. American soldiers train for wars.
"We can see our enemies when we go into battle. We know when we've been injured," Morganstein said. "And we don't worry about the enemy coming home and killing our family."
For over a year, health care workers have been combating an invisible enemy, worried they could bring the danger home to their loved ones. And for that length of time, Morganstein has been working with hospitals to create, what the military calls Combat Operational Stress Control. It's an approach that emphases early intervention to reduce stress, improve well-being and decrease the chance of people burning out.
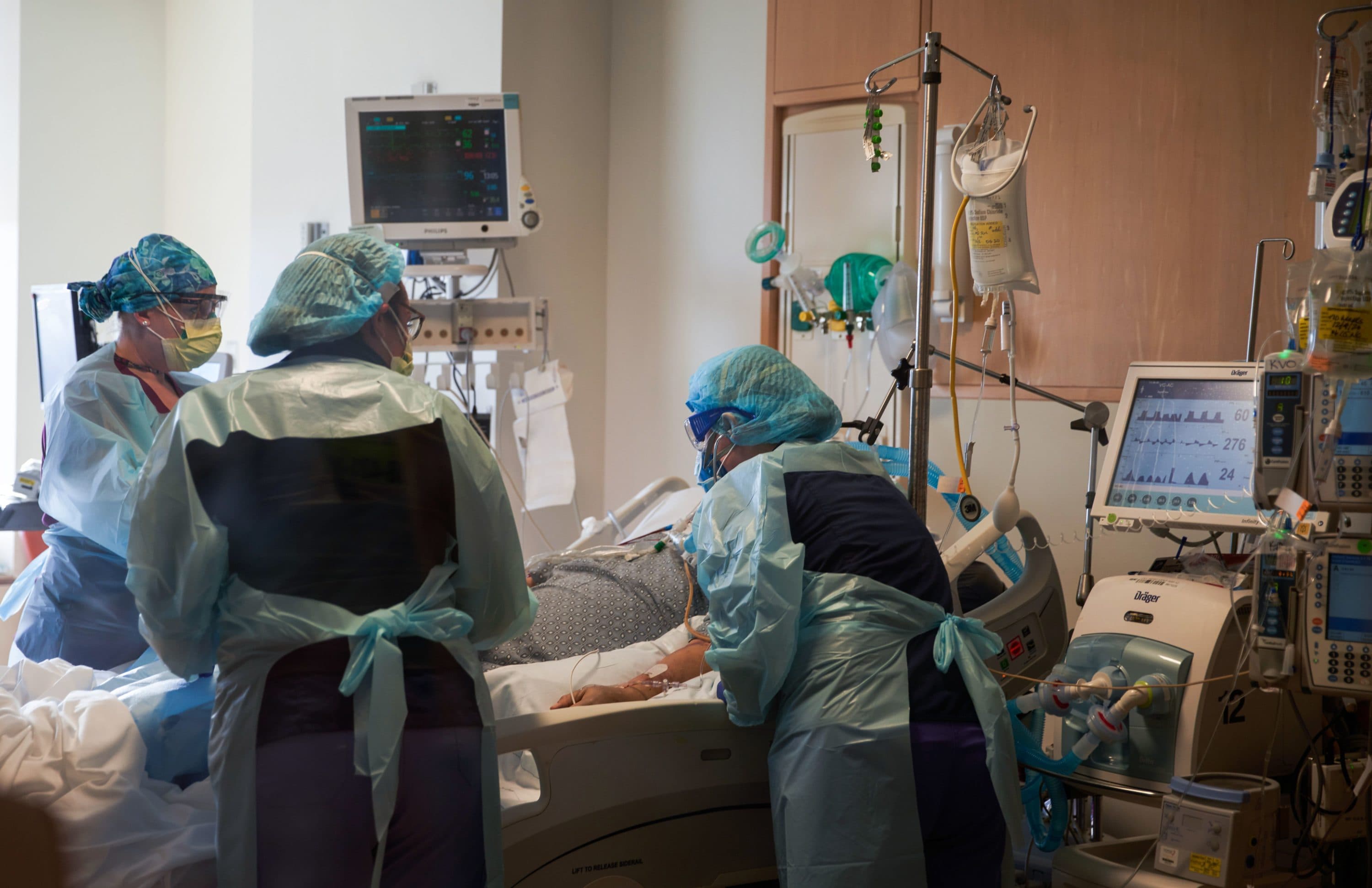
Morganstein personally has experience with the military's approach to reducing stress.
In 2009, Morganstein — a member of the Air Force — was deployed to Afghanistan as the lead psychiatrist for soldiers. There, he got paired up with someone called a "battle buddy." Each was charged with looking after their buddy's mental and physical health.
Now, during the pandemic, hospitals have been asking him how to apply the same concept with health care workers.
Morganstein believes hospitals can use the same strategy to help health care workers deal with the pandemic by pairing them with a colleague to check on their well-being.
"I think there are three main areas someone can quickly ask about: How are things at home? How are things at work? And how are you sleeping?"
Massachusetts General Hospital (MGH) is one of the latest hospitals to start a battle buddy program. Dr. Kerri Palamara is a physician at MGH and also helms a group there called the Workplace Well-Being Collaborative. And there was a moment last year when things became overwhelming.
"I felt like no matter what, I couldn't give enough of myself to any of the people who needed me," Palamara said. "I remember it was one of those 'How's the week going?' and I was like 'I'm drowning. I am absolutely drowning. And I haven't had a day off, but I feel like I can't take a day off because I'm so overwhelmed.'"
Palamara says she's in charge of helping people maintain their well-being at MGH.
"How does it look if the well-being lady can't keep it together?" she said.
But Palamara says she felt lucky, because she had an informal support group. She knows, however, everyone who works at the hospital isn't so fortunate. . . and then she remembered a Q&A with Morganstein last summer.
"I think there are three main areas someone can quickly ask about: How are things at home? How are things at work? And how are you sleeping?"
Dr. Joshua Morganstein
"There's a bunch he's done about the battle buddy program and he got me thinking about it," she remembered.
Since MGH launched its own version of the battle buddy program two weeks ago, 45 people have signed up. And Palamara says it's not just aimed at pairing up nurses and doctors — anyone with an MGH badge can be a part of the program. Meaning, theoretically, a custodian and a brain surgeon could get paired together.
Palamara said the first step will be giving guidance on ways to check in on each other. Like asking how's your day going? Or what's making you feel good?
"Giving people language," Palamara explained. "Questions to ask, prompts that they can use but also responses so that if you hear certain language you can say 'I'm worried about you.' "
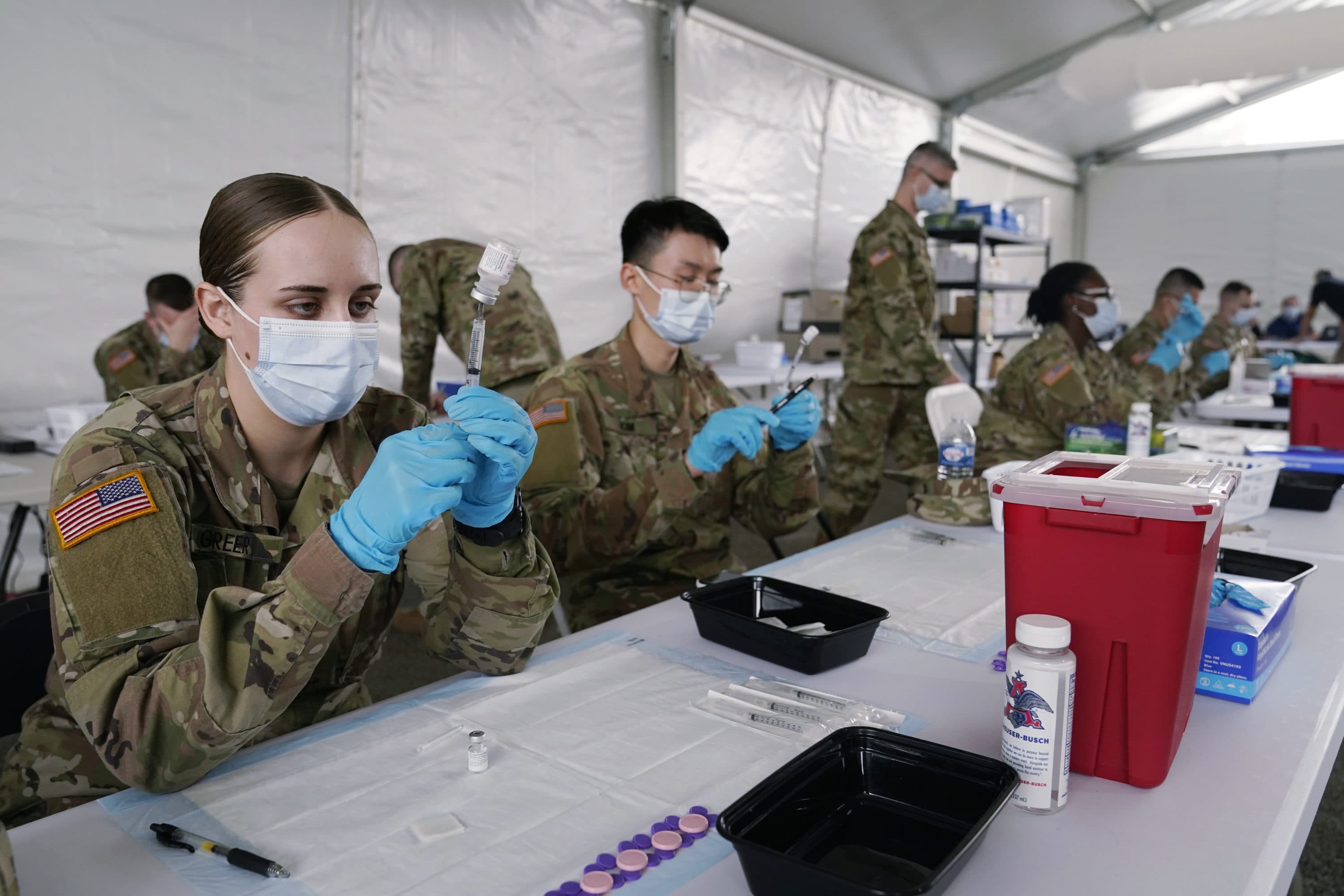
NYC Health + Hospitals began using a battle buddy program late last year.
Jeremy Segall is the chief wellness officer there and said it's already started to show results.
"I got a cold call from an emergency room physician that said that they were contemplating suicide, and it was getting worse and worse and worse and worse," he recounted. "And moving toward a plan. This is a real story."
Then Segall said this physician started going to monthly emotional support meetings with colleagues where they found out about mental health resources.
"And they're now in counseling," Segall said. "And I got a call for them to tell me that that saved their life. True story."
The program at MGH is much newer, but Dr. Palamara thinks it will be a success if it manages to build community and quell loneliness. And she hopes the battle buddy system will remain at the hospital long after the pandemic is over.
"There is no going back to normal, because we're all different now. And our world is different," Palamara said. "But also, clinician well-being and health care worker well-being was a problem before COVID, so even going back to normal doesn't mean that we're okay."
Resources: You can reach the National Suicide Prevention Lifeline at 1-800-273-TALK (8255) and the Samaritans Statewide Hotline (call or text) at 1-877-870-HOPE (4673). Call2Talk can be accessed by calling Massachusetts 211 or 508-532-2255 (or text c2t to 741741).
This segment aired on May 3, 2021.
