Support WBUR
Coronavirus Coverage
Some good COVID news: Deaths were at pre-pandemic levels in Mass. this spring, study finds
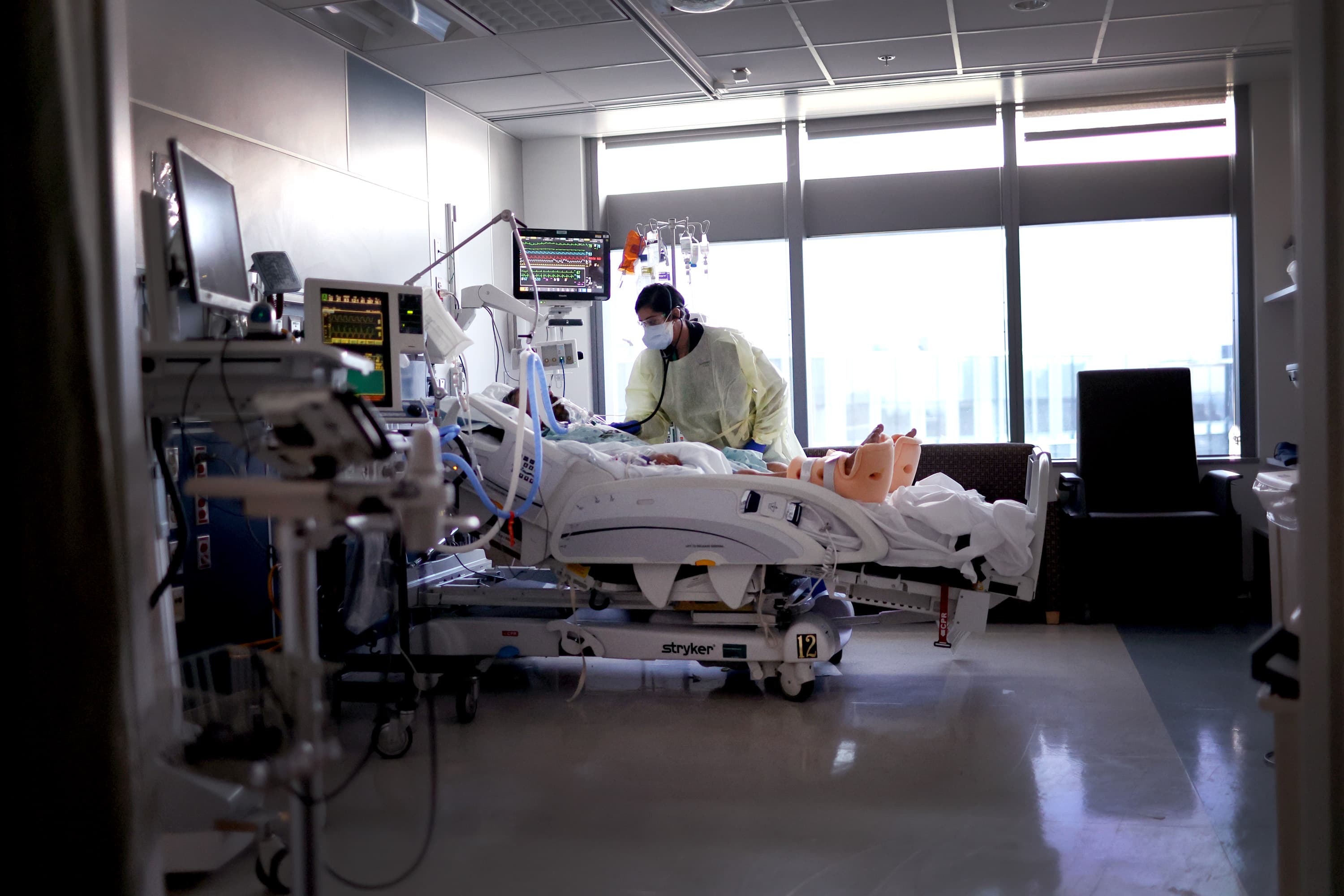
New research shows that between late February and late June, the number of deaths in Massachusetts stayed within a range normally seen before the pandemic. The numbers are notable because they were recorded during a period of high COVID spread due to the omicron variant.
In previous COVID waves, researchers noted large numbers of “excess deaths,” or deaths above and beyond what is considered normal.
While a return to pre-pandemic mortality levels is encouraging, the authors of the study, published this week in The Lancet Infectious Diseases, argued it does not mean the pandemic is over.
Jeremy Faust, lead author and an emergency room physician at Brigham and Women’s Hospital, spoke with WBUR about the findings and their implications.
This interview has been edited and condensed for clarity.
Tell us about the findings. What's new here?
"These findings, I think, are pretty important.
"We found that during the spring — despite the fact that there was a pretty impressive wave of COVID-19 — there were actually no more deaths overall in the state than there usually would be during the same period of time.
"And that's really important because, in every other major COVID wave we've had, we've always seen not just COVID deaths go up, but [deaths from all causes] go up. We've seen incredible deviations from normal during all of our major waves.
"We call this new finding uncoupling. We had a COVID wave. We had cases; we had hospitalizations. But the number of deaths that happened during this period of time was not out of the normal range."
Why did this happen?
"What I think happened was we had a lot of boosters in the fall and winter, and then we had a ton of infections during late Delta and Omicron [in late 2021 and early 2022].
"So, the population of Massachusetts in the spring was pretty highly enriched with people who had recently seen either the virus itself and had immune protection from that, or they had recently been vaccinated or boosted.
"Then, when they did get an infection in the spring, the immunity protected them against, at least, dying."
"This is a combination of our success in vaccinating and our failures in letting so many people already get it. And the future is completely unknown."
Jeremy Faust
This is a morbid thought, but could it be that people who were going to die of COVID had already died?
"There's a grain of truth to that. Every day we get further in this pandemic, the sad truth is that our most vulnerable members of society are always a risk, and we have allowed these people to die. It's just absolutely tragic.
"So, what you have is a healthier survivor cohort, meaning the population that entered the spring wave was not only smaller but also healthier than the one that entered the winter wave.
"But we are not etched in stone. People enter and exit risk pools. So, the spring population might have been a little healthier, but then every day somebody gets a cancer diagnosis, or every day someone gets an organ transplant. The population is constantly evolving.
How does Massachusetts compare with other states?
We do study every state in the country. It's just that Massachusetts is my home state and, also, the best state when it comes to the Department of Public Health providing us data that is very, very up to date.
So, I can't compare yet because there are so many places that are lagging on their data. Ironically, some of the places with the worst excess mortality tend to drag their feet on reporting it. But what I can say is there were dozens of states this spring where there was absolutely excess mortality. Massachusetts just wasn't one of them.
You are not saying the pandemic is over!
"No, we're not!
"My immediate response to seeing good news like this is to worry that people will take that to mean that we no longer have to worry about COVID. And that's not the takeaway.
"The takeaway is that this is a combination of our success in vaccinating and our failures in letting so many people already get it. And the future is completely unknown.
"If there's not excess mortality during a period of time, it's a piece of good news. But then you want to say: ‘Well, wait a minute, are there other forms of suffering that are happening? What are the hospitalizations? Are people missing working or school because of the disease? Are there other longer-term consequences, like long COVID?' It just makes you ask deeper questions.
"But the one thing that we see over and over and over again is if you want to avoid excess mortality, there are two sure ways to do that. Number one: Vaccinate your population, and boost your high-risk population. Number two: Control the amount of virus in your community.
Anything you want to add?
"Yes, the paper found that hospitalizations did still go up during this period of time, we just didn't have excess mortality. There is a line of thinking that says, ‘Oh, a lot of these hospitalizations are with COVID, not for COVID.’ And there's definitely a grain of truth to that. But it misses a really important point: There are actually three kinds of hospitalizations.
"There's for COVID, like you wouldn't be there except that you have COVID, and that's the only reason you're there. That's for COVID.
"Then there's with COVID, but it's not incidental. I call this a tip over. This is a person who has a medical condition and, if they get COVID, that's going to tip the scales. And they're going to have to go to the hospital because they have a life-threatening exacerbation of their heart failure or their diabetes.
"To people who say, ‘Oh, look at all these hospitalizations that are actually not for COVID, but with COVID,’ I would say a majority of those are actually because of COVID still. And those folks really, really need to stay up to date on their vaccinations.
"And then there's a small number of people who are getting admitted to the hospital with a broken bone or something. And they happen to test positive for COVID. That group is probably growing a bit as well, but you cannot shrug off that middle group. It is a huge, huge part of it.
And so I really want people to understand that these hospitalizations are still important and that preventing COVID in high-risk individuals is still worth doing a lot for."
