Support WBUR
Commentary
Stop Debating COVID Vaccine Doses And Fix The Rollout
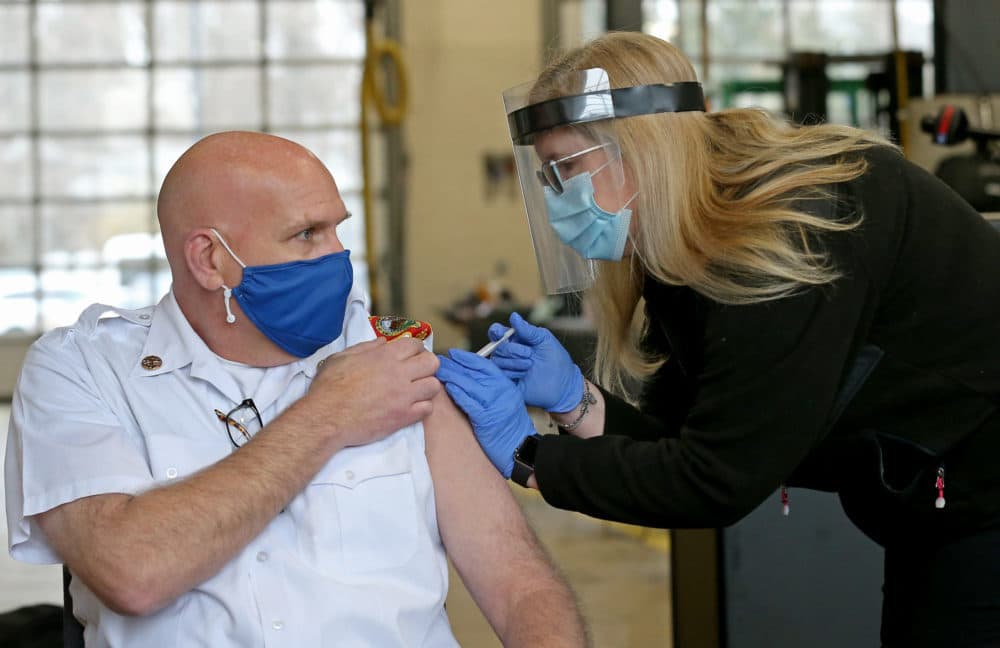
Each passing day in the coronavirus pandemic brings an onslaught of new cases and a mounting death toll. Since distribution and administration of the COVID-19 vaccine have lagged significantly behind the goal set by leaders of Operation Warp Speed — 20 million vaccinated people by the end of December -- public health experts and other scientists around the globe are now debating how to proceed. The central questions: How can we get as many people vaccinated as quickly as possible with a vaccine that requires two doses, several weeks apart? How can vaccine rollout be sped up?
On one side, some experts argue for vaccine dose or schedule adjustments. This would entail either giving two half-doses of the vaccine or delaying the administration of the second dose beyond the studied time period. The argument for these strategies is that giving a “half-dose” or delaying the second dose will maximize early vaccination and allow production and distribution to catch up. On the other side of the debate are those who argue that we should maintain the current schedule and dose, but rapidly ramp up and deploy resources to allow more rapid administration. Central to this approach is that since less than one-quarter of the distributed doses have been administered, the problem is currently one of logistics and infrastructure rather than supply.
Simply changing the vaccine dose or schedule does not address the root cause: lack of infrastructure.
As an infectious diseases physician and public health expert who has worked on the ground throughout this pandemic, I plant myself firmly in the “maintain the current schedule and dose” camp. Over the next few weeks, it’s worth maximizing early vaccination — a strategy that the Biden administration has committed to — knowing that pharmaceutical companies will be able to produce sufficient second dose supply for the vast majority of people without delay.
First, there is no scientific evidence to support a dose or schedule adjustment. The vaccine studies were conducted in a rigorous and transparent fashion to determine the optimal dose on a given schedule. Neither study demonstrated the efficacy of half-doses or delayed dosing. Furthermore, there are potential risks of changing the dosing or schedule including inadequate protection from the virus, waning immunity and selection of variants that can evade immunologic protection.
Second, changing the dose or schedule is not just scientifically questionable — it is also lazy. Like other aspects of this pandemic — testing and personal protective equipment, for example — there has been no national strategic plan. Operation Warp Speed did not include plans to ramp up production of dry ice or specialized freezers for vaccine storage, increase access to transport vehicles, or train and mobilize a vaccination workforce. Simply changing the vaccine dose or schedule does not address the root cause: lack of infrastructure. It will take time to make up for the lack of planning to build this infrastructure.
If we have learned anything from the current pandemic, it is that community trust in science and public health is essential to controlling the spread of the virus.
Third, and most importantly, building trust around vaccines is paramount to the success of this and future vaccination campaigns. For months, health professionals have implored people to “trust us” and “trust the science.” We have held listening sessions with communities, deployed public health messages on social and mainstream media, and debunked myths and misinformation about vaccines. Changing the vaccine dose or schedule in the absence of evidence is experimentation — something that we have assured communities that we are not doing with this vaccine. All of the efforts to build trust have begun to pay off — vaccine confidence continues to increase. Changing the vaccine dose or schedule in the absence of efficacy data is not only hypocritical but will undermine public trust and give people more reasons to be hesitant about vaccines.
Finally, if we destroy trust now by altering the plan at the eleventh hour, it will have ripple effects for years to come. While we are in the midst of the largest pandemic of our generation, it is unlikely to be the last. As deforestation, climate change and worldwide poverty continue to grow, so too does the risk of future pandemics. A central component of control of those pandemics will surely be vaccine development and acceptance. If we have learned anything from the current pandemic, it is that community trust in science and public health is essential to controlling the spread of the virus.
While the current debate is perhaps an important academic exercise, it is detracting from real solutions. We are in the midst of a public health emergency with real lives being lost by the thousands on a daily basis and real resource limitations. In the time spent debating options that are not based on science and will erode public trust, public health officials could devise multiple plans that include rapid infrastructure scale-up and the mobilization of vaccination teams. Doing so would not only improve vaccine rollout but also continue to build the public’s trust in science. This is how we’ll survive the pandemic.
