Support WBUR
Knowing How To Remove PPE Is A Matter Of Life And Death, One ER Doctor Says
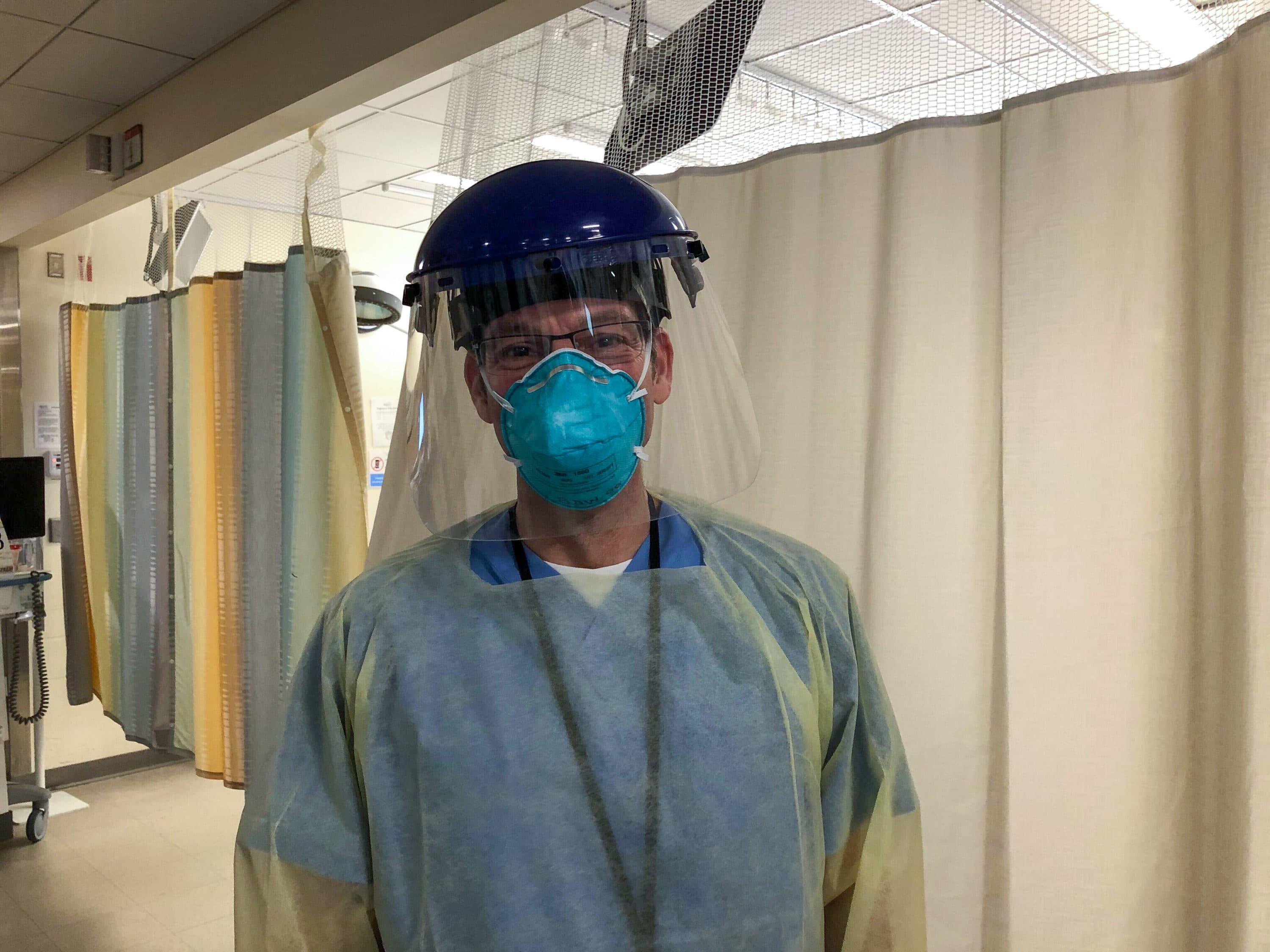
Massachusetts now has the third-highest number of COVID-19 infections in the U.S. with nearly 27,000 cases. The death toll is close to 850, and hospitals are bracing for a surge in new patients as the outbreak reaches its peak in the state.
The intensive care unit reached capacity more than a week ago at Boston Medical Center, the city’s fleet-footed hospital accustomed to crisis. They are temporarily diverting ambulances to other hospitals and plan to add more beds.
Dr. Ron Medzon, an emergency physician and director of the Solomont Clinical Simulation Center, says the situation at the hospital is “really hard to describe.”
“We have patients who are coming in off the street just looking for testing because they have a cough and they've been in contact with someone,” he says, “all the way to people who really are struggling to breathe, have very low oxygen and are at death's door.”
Medzon, who teaches hospital staff how to properly put on and take off personal protective equipment [PPE], says health care workers have to be extra vigilant about protecting themselves “first and foremost.”
“You have absolutely no room for error — and it's exhausting,” he says.
When a new patient enters the hospital, most doctors and nurses will instinctively want to help the patient before protecting themselves, Medzon says. This happened recently when a nurse wanted to quickly hook a patient up to oxygen before putting her equipment on, and Medzon says he had to stop her.
“The nurse sort of ran in and wanted to get oxygen going, and I actually had to stop her physically and hold her back,” he says. “And I said, 'Wait. We need to put our equipment on, and we've got to be careful.’ ”
Medzon says the best way for health care workers to keep themselves safe is to “get a buddy” for donning and removing PPE.
“Have somebody watch you put the stuff on and take the stuff off,” he says. “It seems silly, but you're going to save a life. And you might save your own.”
(Note: Dr. Ron Medzon is the husband of Here & Now producer Karyn Miller-Medzon.)
Interview Highlights
On how to properly put on and remove PPE
“Putting them on is actually the easy part because you're clean. So even if you forget a step in its order, we usually use something called the buddy system, and I make sure that after I put on all of my stuff, somebody takes a look and makes sure that nothing is exposed. So I've got a pair of gloves on, a gown, a second pair of gloves, an N-95 mask, a head covering, and then I put on a visor. And that's just if I'm going to go in and do a nasal swab. So that's the easy part.
“The hard part is taking this off without getting contaminated. And that's why I train and have people pair off and actually read off a checklist because as great as we think we are, we are not. And we can't see it. We can't see ourselves. I can't tell you how many times I've done a training where I've been the example and I'm pulling off my gown, and somebody says, 'Your shoulder is exposed,' or 'you're touching your elbow here.' And if that was coronavirus, I would have touched it to my clothing, and now I become someone who can infect myself, my family, my patients and my staff. And that is serious business.”
Click here for educational videos on donning and doffing PPE such as N95 masks and face shields.
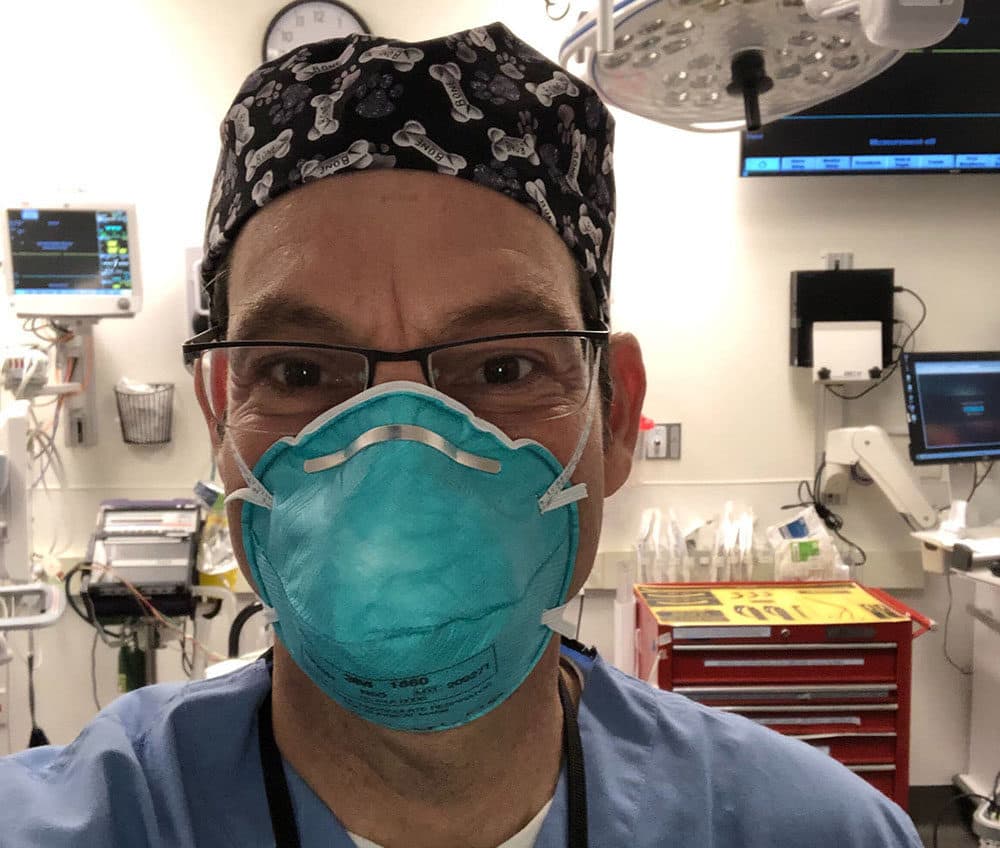
On sanitizing and washing his hands “over and over again”
“So let's say I've taken a swab. I deposit that, someone's standing outside the door, so I don't leave the room, and I drop that bag in the clean bag. I turn around, sanitize my hands, take off that set of gloves, sanitize my hands, take off my gown in a special way where I roll it forward so that I don't touch any of the exposed area, throw that out, sanitize my gloves again. These are gloved hands. And I exit the room, sanitize my hands. Then I take off my head covering, wipe the visor, sanitize my hands again, wipe the inside of the visor, put the visor down, sanitize my hands again. Take off my gloves, sanitize my hands. And then I walk over the sink and I do a full hand washing.
“The other thing that's important to point out is that while I'm doing this, there are other patients being wheeled in who could be really sick, and I can't just rush into the next room, even though I have people saying we've got someone with low oxygen who's sitting next door. I have to go through this whole thing again just to get through the door and then to leave again. And so as they come in and as this surge comes, that's really my biggest fear and concern is when the place is full and we're overwhelmed, the urge will be just to go and try to do something. But you have to stop and be careful.”
On seeing patients with the coronavirus
“Seeing the patients I find very difficult because I like to connect with people, and it's really hard when all you've got is your eyes above the mask and you're talking through two masks and the visor. And you can see the fear in their eyes and that fear should be there. So I can't just comfort somebody, and I certainly can't say, 'Everything's going to be okay.' My patient … with the low oxygen, she's probably not going to do well. She might wind up on a ventilator in the next few days, and she might not pull through. So I can't make a false narrative, and it's really painful. And I'm getting into discussions with family saying, 'Why can't I come in?' I've got a 97-year-old. Odds are she's not going to make it. And they all want to come see her. They said, 'How can you keep us from seeing her?' And you know, what do you say to someone like that? All I could say is this narrative is playing out with thousands of people across this country. And it's the worst thing to have to tell you this, but right now, we can't accept visitors because it's too much of a risk.”
Karyn Miller-Medzon produced and edited this interview for broadcast with Tinku Ray. Samantha Raphelson adapted it for the web.
This article was originally published on April 14, 2020.
This segment aired on April 14, 2020.
