Support WBUR
Disorganized Research Slows Discovery Of COVID-19 Treatments, Experts Say
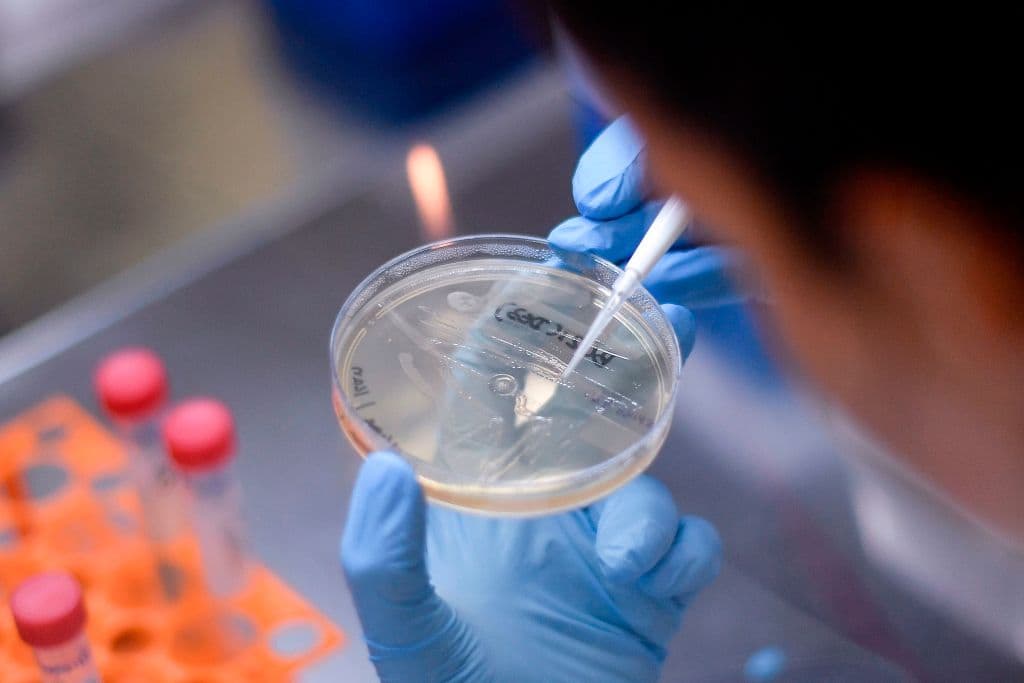
As researchers around the world race to develop treatments — and ultimately a cure — for COVID-19, some are saying a lack of coordination is slowing the process.
They point to the more than 90 trials for hydroxychloroquine, and the fact researchers end up competing with others to have their ideas tested in hospitals and labs.
Among those calling for collaboration is Dr. Derek Angus, chair of Critical Care Medicine at the University of Pittsburgh. This disease is inspiring people to want to fix the problem, he says, but a lack of coordination means everyone is flooding the marketplace trying to get their idea heard.
“Drug companies are all knocking on the door of every hospital or large academic medical center saying, 'Please do my study. My study is most important,' ” he says. “And it instantly put the whole world into a position of trying to choose.”
The National Institutes of Health is trying to fix this problem. Director Francis Collins is planning a global public-private partnership, including pharmaceutical companies and academic institutions.
But the project has been under wraps because organizers are struggling to get people to buy in. The problem, Angus says, is that our system rewards tribalism.
“Federal funding agencies tend to fund national projects because they're responsible to their taxpayers. Investigators that work at universities do have some responsibility to the universities, and pharmaceutical companies are in a marketplace in competition with each other,” he says. “So there are legitimate barriers to one effective large collaboration.”
Experts also don’t have a sense of what drugs are effective against COVID-19 because fewer than 2,000 people have participated in clinical trials when more than 3 million have had the disease, Angus says. If one in 10 people participated in a trial, he says, scientists could have tested nearly 100 different drugs by now.
But many patients don’t want to participate in trials because with such a deadly disease, they don’t want to take the 50/50 chance of receiving a placebo, he says. Doctors feel like they have to make a choice when considering clinical trials, too.
“You can either take care of the patient or you can test the drug, and that is in part because some of the designs that are best for testing the drug don't feel very friendly toward taking care of the patient,” he says. “And at the heart of it, no one wants to be a guinea pig.”
During the H1N1 outbreak in 2009, researchers began to realize that traditional randomized trials were inefficient in a pandemic. So scientists launched a fast-track remap trial, where they test combinations of drugs together. Now Angus is leading a similar trial for COVID-19 at the University of Pittsburgh School of Medicine.
“Nearly everyone is getting the opportunity to try something that we think will help. The other thing we do in the design is the trial learns as it goes,” he says. “The combinations that are doing best get a bigger and bigger share of the pie over time.”
The trial is part of an international effort involving hundreds of investigators, and Angus says the goal is to continue rolling it out globally.
At the end of the day, Angus says researchers need to be willing to surrender their ideas in order to work as a team.
“I have lots of opinions about which drugs I think might work best. I've ended up deciding to not even voice my opinion, but rather try to really just think more about what's a trial design that can be as modular as possible and let as many people in as possible,” he says. “There's no question that we have to do some compromising for the joint good.”
Karyn Miller-Medzon produced and edited this interview for broadcast with Peter O'Dowd. Samantha Raphelson adapted it for the web.
This segment aired on April 29, 2020.

