Support WBUR
Coronavirus Coverage
COVID-19 Hit Mass. Nursing Homes Hard — Especially Those Serving People Of Color

Like a lot of people with loved ones in long-term care facilities, Priscilla Flint-Banks spent much of the spring worried about her 87-year-old mother, Ruby Kinney. Kinney, who had dementia, lived in the Edgar P. Benjamin Healthcare Center, a predominantly Black nursing home in Roxbury.
In early April, Flint-Banks called to check on her mom and spoke to a nurse. She says she asked whether the home had any COVID-positive residents.
“She’s like, ‘No. Nobody got COVID here,’ ” Flint-Banks says. “So I said, ‘OK, thank you.’ And then two weeks later, my mom dies.”
Ruby Kinney died from COVID-19 on April 22. Flint-Banks says a doctor at the nursing home, which declined to comment for this story, called to tell her the news.
“I didn't have any clue that they even thought she had COVID,” Flint-Banks says. “I just started crying, me and my husband both.”
In Massachusetts, nursing homes were hit hard and early by the coronavirus. Thousands of residents in these facilities have died from COVID-19, and the death rate from the virus in nursing homes is 90 times that of the statewide death rate.
But nursing homes across the state did not bear this burden equally.
Twenty people died from COVID-19 in Kinney’s nursing home. This is higher than the statewide average in facilities with coronavirus outbreaks: 15.5 deaths. State data also shows that nursing homes serving more residents of color had, on average, more COVID-related deaths.
This is partly explained by the fact that these facilities tend to have more residents. But even when you look at the rate of death, the disparity persists.
"It’s like if you’re Black you’re doomed... We live in two Bostons. We live in two Massachusetts. We live in two United States of America."
Priscilla Flint-Banks
A WBUR analysis of Massachusetts nursing homes reveals, for the first time, a higher COVID-19 death rate at more diverse nursing homes compared to overwhelmingly white facilities. The analysis used data from Brown University’s LTCFocus, the Centers for Medicare & Medicaid Services and the state of Massachusetts.
Because of how race data is reported in the state, and the fact that Massachusetts nursing homes are 88% white, the analysis compared nursing homes that were “overwhelmingly white” (at least 82.5% of residents were white) to nursing homes that were “more diverse” (less than 82.5% of residents were white).
Our analysis only looked at nursing homes that reported coronavirus cases, and used the number of licensed beds as a proxy for number of residents. It also controlled for age — one of the biggest risk factors of dying from COVID-19.
We found that majority-white nursing homes had an average of 11.8 virus deaths for every 100 residents, while nursing homes that served more people of color had an average of 14.8 deaths. This means that more diverse nursing homes had, on average, 25% more COVID-19 deaths than predominantly white facilities.
Our analysis also found that in Massachusetts, residents in more diverse nursing homes are, on average, six years younger than people in overwhelmingly white nursing homes. (Black and Latinx older adults are less likely to be able to afford things like in-home care, assisted living or continuing care retirement communities, so tend to enter nursing homes earlier in life, experts say.)
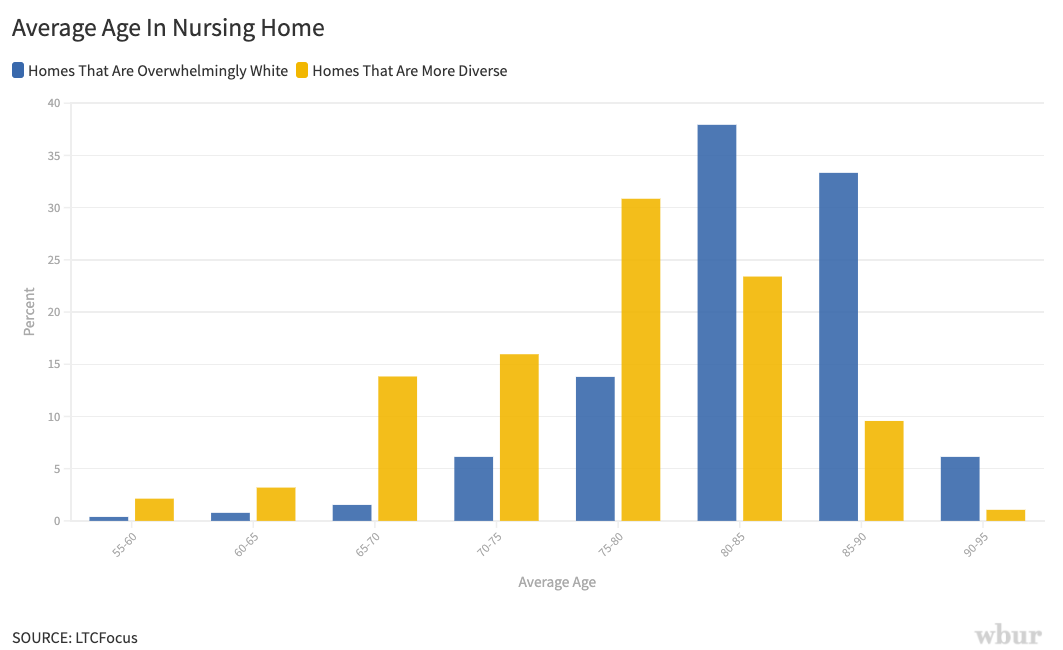
A younger group, with a higher average death rate, is striking.
WBUR’s findings align with other studies showing that Black, Latinx and Indigenous Americans are dying from COVID-19 at higher rates, and that nursing homes with more Black and Latinx residents are more likely to have COVID outbreaks.
“One of the go-to explanations for the racial disparities in COVID mortality have been what people call ‘comorbidities,’ ” says Dr. Mary Bassett, director of the François-Xavier Bagnoud Center for Health and Human Rights at Harvard. “In other words, people were sick and vulnerable for other reasons, even before they encountered this novel coronavirus.”
But this framing, Bassett says, overemphasizes the degree to which underlying health problems contribute to racial disparities in coronavirus mortality rates. She points to a more important factor: whether someone was exposed to the virus in the first place.
“In order to die of COVID-19, you first have to get infected. And that may have to do with the kinds of practices that exist in a nursing home,” she says.
A nursing home’s ability to respond to a pandemic is related to its overall ability to deliver quality care. And this often comes down to money, staff numbers, and other resources.
“Preventing COVID spread in a nursing home, of course, would take resources, whether it be training and retraining, purchasing adequate [personal protective equipment], creating isolation wings, using staff dedicated solely for COVID patients,” says Jennifer Gaudet Hefele, a fellow at the Gerontology Institute at UMass Boston and a senior scientist at the consulting firm Booz Allen Hamilton.
“What's causing this is systemic racism...disadvantage that accumulates over the course of a life.”
Jennifer Gaudet Hefele
And, she says, “Black and Latino older adults don't have equal access to high-quality nursing homes.”
When experts talk about nursing home quality, they’re usually talking about indicators like the number of beds in a facility, staff ratings, a facility’s Medicare star rating and the percent of residents covered by Medicaid. Black and Latinx older adults are on average less wealthy than their white counterparts, and they tend to rely more on Medicaid, which pays nursing homes less than someone paying out of pocket.
These factors help explain racial disparities in nursing homes, but they don’t tell the whole story. The reality is “really complex and really tough to disentangle because there's multiple layers of disadvantage accumulating through the life-course,” Gaudet Hefele says.
But she says one thing is clear: “What's causing this is systemic racism, and disadvantage that's associated with systemic racism. Discrimination in employment, discrimination in education, discrimination in housing. This is disadvantage that accumulates over the course of a life.”
For Flint-Banks, her mother’s death from COVID-19 is just one more example of how structural racism affects the health of Black people.
“It’s like if you’re Black, you’re doomed,” she says. “We don't get the same care as white folks do — it’s just the honest-to-God truth. We are treated different. We live in two Bostons. We live in two Massachusetts. We live in two United States of America. And Black people have always been on the bottom.”
WBUR reported this story with help from Lacey Loomer, PhD, an assistant professor of Health Care Management at the University of Minnesota-Duluth.
This segment aired on October 23, 2020.

