Support WBUR
'It Didn't Need To Happen': UMass Memorial Chief On Bed Shortage And COVID Surge
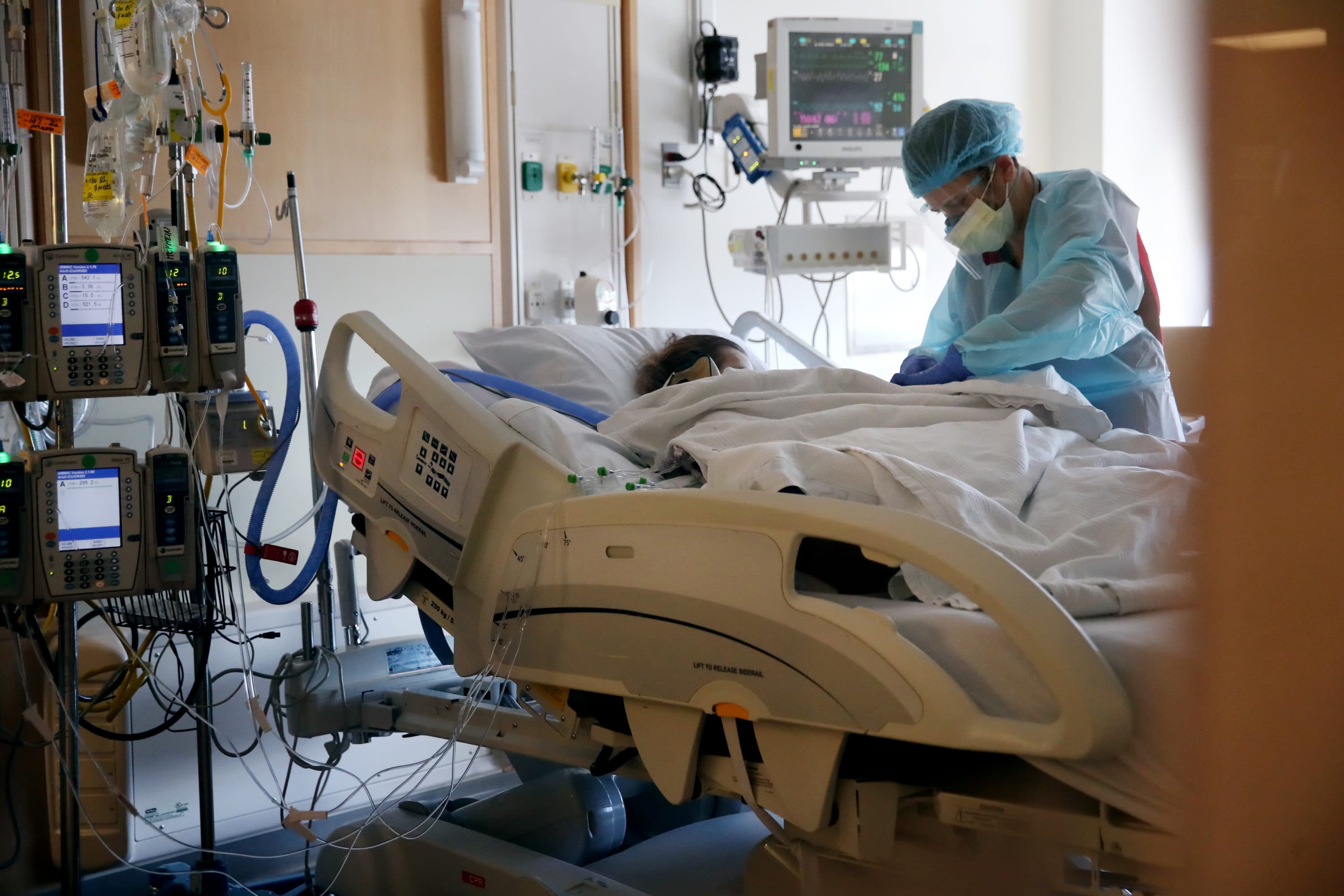
Dr. Eric Dickson is weary. He says the hospital system he heads has reached a crisis point.
He's the president and CEO of UMass Memorial Health, based in Worcester. He says the region has almost 20 times more COVID patients hospitalized than in June, and that as of Tuesday, there is not a single intensive care hospital bed available in central Massachusetts. When a bed opens, there's a patient waiting to take it.
On top of that, St. Vincent Hospital in Worcester and its nurses have yet to reach a settlement. Nurses have been on strike since March. St. Vincent says it has taken more than 100 beds off line due to a reduction in nurse staffing. The contract dispute centered on staffing levels is at an impasse.
Dr. Dickson says things didn't have to get this bad for hospitals in the region. He welcomes the indoor mask mandate that went into effect in Worcester Monday. But, he says, there should have been more widespread mask mandates and capacity limits sooner, given the spread of the highly contagious delta variant of the coronavirus.
Dickson spoke with WBUR's All Things Considered host Lisa Mullins.
Interview Highlights
On what he considers a slow response by elected officials to this recent surge in COVID cases:
"This is getting bad again; and you can tell me we're the second most vaccinated state in the country all you want, and you can tell me we have the second lowest number of COVID cases in the hospital all you want. I have to go in and look at an exhausted emergency room staff with 30 and 40 patients waiting for [inpatient] beds. And they don't care what our vaccination rates are — they're not high enough. And they don't care where we rank relative to other states. They just know that they have it real bad right now, and it's making it hard for them to take good care of their patients."
On what kinds of patients are waiting for hospital beds:
"Mostly they are patients of any kind, with a lot of illnesses that have really pent up over time. For example, when we were in lockdown during the first phase — the first COVID wave — cancer screening went down by 90%. Cancer screening works, and when it goes down by 90%, there's a price you pay for that later. COVID didn't cure cancer, but it sure did make it hard for us to detect it early. So it's those kind of things that are pent up. And now you have all the normal summer traumas that are occurring. People are getting other infections because they're congregating again, plus COVID, plus a workforce shortage across industries and beds offline at St. Vincent Hospital. And all of that is adding up to an incredibly, incredibly stressed-out staff here at UMass Memorial and patients that are frustrated, as well, with long waits in the emergency department or [operating room] cancelations. And a lot of it — I just believe it didn't need to happen."
On how the St. Vincent Hospital nurses strike is affecting the UMass hospital system:
"To put it in perspective, right now across UMass Memorial, we have 80 to 100 patients waiting for a bed. They're sitting in post anesthesia care units, coming out of the OR, they're sitting in the ER, and that's the number of beds that are closed now at St. Vincent ... So now you have a public health crisis here in central Massachusetts, and you have good qualified nurses sitting on the sidelines. Most of our problem could be averted by those two parties coming together and getting those nurses working again."
On whether patients coming to UMass Memorial hospitals tonight because of heart attacks, pneumonia or other conditions would be able to get the help they need:
"They, of course, could get help. And the emergency departments are still functioning. They're just functioning at a suboptimal level, because instead of having emergency department patients in there that require emergency care, a lot of the space is being taken up with patients that are waiting to go upstairs [to general medical and intensive care units]. And it's not uncommon for any of us that work in emergency medicine — I'm an emergency physician — to get overwhelmed from time to time, right? You can't plan for everything that's going to occur. But when it goes on day after day after day, you start making a decision if you're going to operate on the person with pancreatic cancer versus breast cancer, and which one of them is likely to progress fastest. And we've had days recently where those are the kind of decisions that we were making.
"It's certainly delaying care that you don't want to delay. And so everybody gets done, and then you ask the staff to do elective cases on Saturdays and Sundays ... and it becomes an enormous challenge."
On having to say he's sorry to patients and employees:
"It's been a very common word around here — not just sorry to the patients, who I feel horrible about not being able to get in and sometimes having long waits and having to put off scheduled surgeries. But sorry to the [nurses, doctors and other] caregivers. I mean, they've been through so much already. That's probably the hardest part for me right now."
This segment aired on September 21, 2021.

