Support WBUR
Some States Allow Authorities To Use Ketamine To Subdue Suspects In The Field. But Is It Safe?
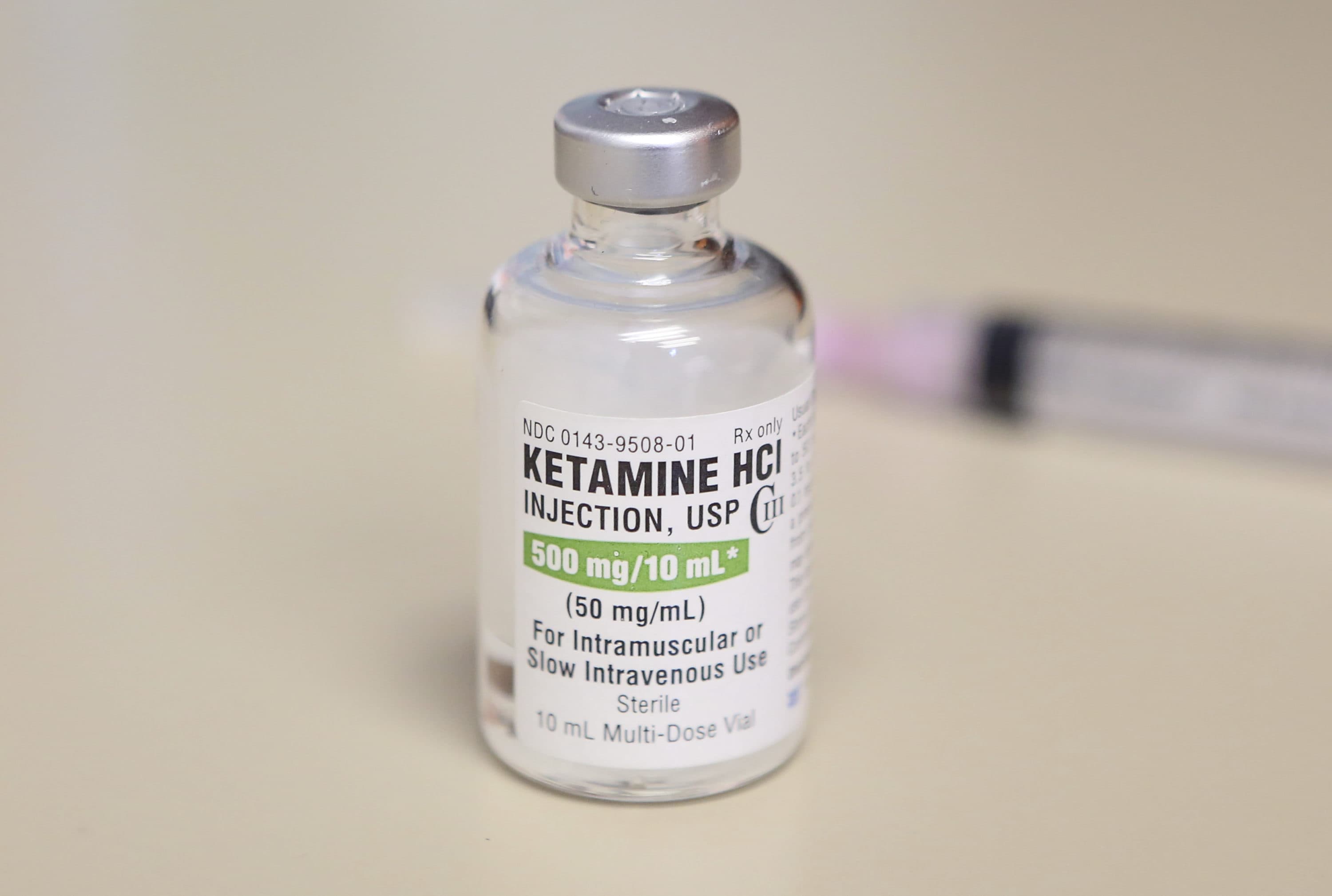
Two recent incidents involving police force are raising concerns over the use of anesthetic ketamine — a powerful sedative normally used in hospitals — as a law enforcement tool to subdue suspects in the field.
In a four-day period in Aurora, Colorado, last August, 23-year-old Elijah McClain and 25-year-old Elijah McKnight were both given doses of ketamine in separate police incidents. McClain went into cardiac arrest and died several days later. McKnight was hospitalized on life support but survived.
Video footage of both incidents shows that neither McClain nor McKnight was resisting arrest when the ketamine was administered.
In Minnesota, a former emergency medical services worker recently filed a whistleblower lawsuit alleging that he was pressured by police to use ketamine when it wasn't warranted. And in the state’s largest city, Minneapolis, The Intercept reports ketamine use grew from an average of four police incidents per year before 2015 to 62 in 2017.
The American Society of Anesthesiologists has issued a statement opposing the use of ketamine and other sedatives to "chemically incapacitate" suspects.
Dr. Mary Dale Peterson, president of ASA, says like with any anesthetic, “dangerous complications” can occur with ketamine. That’s why it should be given strictly for medical reasons with well-trained professionals monitoring the situation, she says.
There are several medical justifications for administering ketamine in settings outside of the hospital, she says. These include medical distress at the scene of a car accident or someone having a seizure in their home. But cases where an individual is truly in danger of hurting themselves or others — where ketamine use might be justified — occur “very rarely,” she says.
Police have pointed to excited delirium — defined by the National Center for Biotechnology Information as “bizarre and aggressive behavior, shouting, paranoia, panic, violence toward others, unexpected physical strength, and hyperthermia” — to justify use of ketamine on a suspect.
Police officers aren’t trained to diagnose excited delirium and the role of doing so should be reassigned to medical personnel, Peterson says. Plus, even within the medical community, the definition of excited delirium is complicated, she says. The syndrome is not recognized by major medical organizations such as the American Medical Association.
Aurora police officers cited excited delirium in their decision to administer ketamine to McClain. In Colorado over the past two and a half years, police injected suspects with ketamine more than 900 times for excited delirium, according to the Colorado Sun.
In Colorado, an officer must apply for a ketamine waiver from one of the state’s 90 fire departments or emergency medical service agencies, saying that the suspect in their custody is suffering from excited delirium, according to the Denver Post.
“But I think that to ask an EMT to give ketamine as a chemical restraint when the person is already restrained is inappropriate,” Peterson says.
Neither McClain nor McKnight exhibited signs of excited delirium, she says, adding that being upset or agitated after being arrested is not a sign of mental illness.
When used properly in a hospital setting, ketamine can help relieve pain and has neuroprotective, anti-inflammatory and anti-tumor effects, according to a study in the NCBI.
Yet it’s not without risks. About 20% of people will have hallucinations or bad reactions when they wake up after taking the dissociative anesthetic, she says, and it can have effects on the respiratory and cardiac systems.
“You have to understand all the pros and cons of giving ketamine and in the correct dosages and with monitoring, and really having somebody there that can be available and ready to step in as somebody stops breathing or becomes hypoxic or their blood pressure rises or the heart rate goes up too fast,” she says.
Complications with ketamine can also happen with dosage issues. McClain only weighed 143 pounds at the time of his arrest, yet was given a ketamine dose for a 200-pound man.
Police have defended the use of ketamine, saying suspects can be belligerent and even dangerous when they have mental health issues or have taken drugs — two issues afflicting the country. While Peterson says she sympathizes with first responders navigating the nation’s “mental health crisis,” she believes police officers need more behavioral health training and that more crisis intervention teams need to be created.
States should also review their ketamine waiver programs and determine how to avoid complications, she advises.
“I think any time it's being given in the field, those cases should be reviewed,” she says. “They should be scrutinized and overseen.”
While there are legitimate medical reasons for giving ketamine in the field, she says restraining an agitated suspect handcuffed on the ground isn’t one.
“It is about doing it for the right reasons in the right dosages with monitoring and well-trained personnel under medical direction,” she says, “but not just for law enforcement purposes.”
Karyn Miller-Medzon produced and edited this interview for broadcast with Todd Mundt. Serena McMahon adapted it for the web.
This segment aired on September 8, 2020.

